Novo Nordisk expects high demand for its obesity drugs in India, says country head
Team Metabolic Health
Popular weight-loss drug Wegovy maker Novo Nordisk (NOVOb.CO) expects high demand and acceptance for its anti-obesity drug, when launched in India, a top executive said.
The company is still “evaluating” the price of the drug, but is confident that the price-sensitive Indian population will be able to afford it, Novo’s India Managing Director Vikrant Shrotriya said.
“It is going to be a very promising launch in India where the acceptance of the medication is going to be higher than what we have seen in many of the other therapy areas,” Shrotriya said.
Government intervention is necessary to raise awareness among the larger Indian population about obesity being a chronic disease, Shrotriya said on Wednesday, while presenting a 2022 Novo-funded study on India’s obesity market.
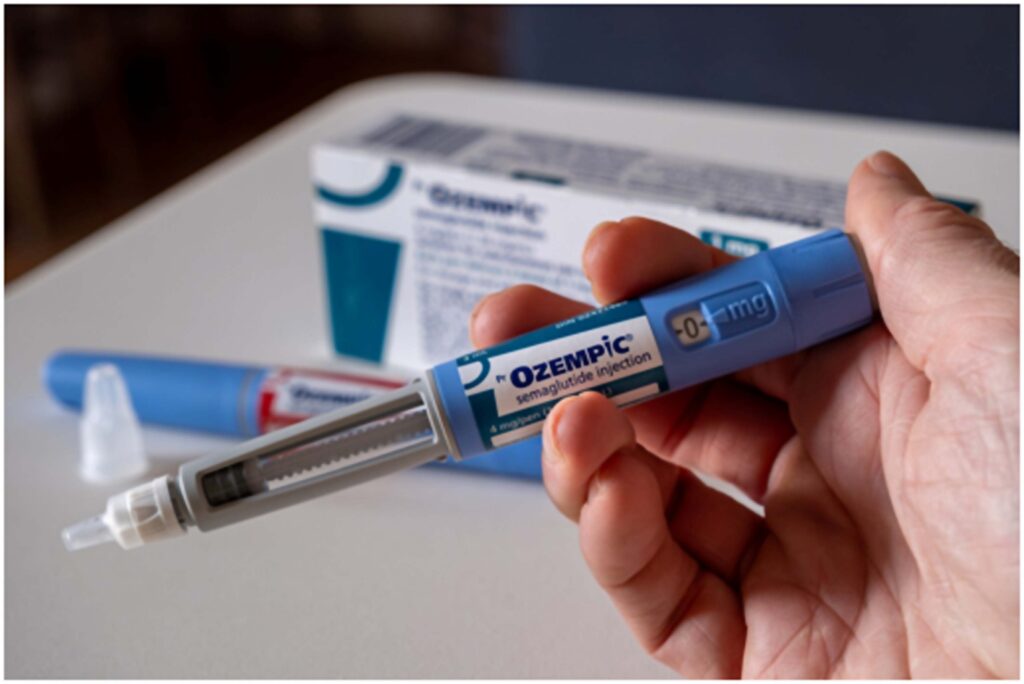
The Danish drugmaker’s blockbuster drug Wegovy and related diabetes drug Ozempic belong to a class of therapies known as GLP-1 receptor agonists that help control blood sugar and slow digestion, making people feel fuller for longer.

Boxes of Wegovy move along a packaging line at Novo Nordisk’s facility in Hillerod, Denmark, March 8, 2024. REUTERS/Tom Little//File Photo
Soaring global demand for these drugs, including U.S. rival Eli Lilly’s (LLY.N), opens new tab Zepbound and Mounjaro, has made the companies among the world’s valuable as they aggressively compete in a global weight-loss market that some analysts predict could reach $150 billion in the next decade.
Novo, which last year told Reuters about plans to launch Wegovy in India in 2026, refused to comment on if it was on track for the same, adding the company has some “reservations about it at this point of time” given the global demand has surpassed their production capacity.
“There are (other) countries in the list for launch,” he said.
Lilly plans to launch its obesity drug in India by next year. Both companies are expected to face competition from Indian drugmakers who are developing generic versions of weight-loss drugs for the global and price-conscious Indian market.
Credit: Reuters
Novo Nordisk affirms 25% weight-loss expectation for experimental drug CagriSema
Team Metabolic Health
Novo Nordisk (NOVOb.CO), opens new tab said the side effects in trials so far for its experimental obesity drug CagriSema were similar to its GLP-1 drugs already on the market, and reiterated its expectation the new injection will deliver 25% weight loss.
Martin Holst Lange, Novo Nordisk’s head of development, made the comments to Reuters after the company released better-than-expected third-quarter results.
The Danish drugmaker is due to release data from a late-stage trial of CagriSema, a two-drug combination obesity treatment that, like its popular obesity drug Wegovy, is injected, by the end of 2024.
CagriSema targets the same gut hormone as Wegovy does, but also targets a pancreas hormone called amylin.
Novo Nordisk has previously said that CagriSema has a potential of up to 25% weight loss, compared with the 15% weight loss of Wegovy.

Flags with the Novo Nordisk logo flutter outside their Danish company’s offices in Copenhagen, Denmark. REUTERS/Tom Little/File Photo
Lange said on Wednesday the company still expects the data from its Phase 3 trial to reflect this higher weight loss.
“No change in our confidence level,” he said.
Analysts view this data as “a must-win” for Novo’s obesity-driven investment case, given the hot competition among pharma companies to deliver higher weight loss than Wegovy and Zepbound, the rival obesity injection that U.S. company Eli Lilly (LLY.N), opens new tab launched last year.
Novo’s share price could go up to 20% higher or lower depending on it, predict ABG Sundal Collier analysts.
Lange said that Novo needed to collect more data on the psychiatric side effects of another experimental obesity treatment, monlunabant, in a Phase 2b trial before it could progress to a Phase 3 or late-stage trial.
The company’s shares fell nearly 5% in September after results from a Phase 2a trial of monlunabant, a pill, came in below market expectations. Novo acquired the drug last year as part of its $1 billion purchase of Canadian biotech firm Inversago Pharmaceuticals.
Novo had already planned to conduct a Phase 2b trial even before it got the data from the latest trial, Lange said, but the Phase 2a trial did reveal new psychiatric side effects and suggests that perhaps excessively high dose strengths were tested. The new trial will involve a lower-dose strength, he said.
Credit: Reuters
Novo Nordisk lifts curbs on Wegovy prescriptions in the U.S., says CEO
Team Metabolic Health
Novo Nordisk (NOVOb.CO), opens new tab is lifting curbs on prescriptions of its weight-loss drug Wegovy in the United States and is increasing supply in that market, its CEO said on Wednesday.
“In our guidance for the full year, you can assume that there is a step up in the fourth quarter and that’s partly driven by increased products including Wegovy into the U.S.,” Lars Fruergaard Jorgensen told Reuters in an interview.

Boxes of Wegovy move along a packaging line at Novo Nordisk’s facility in Hillerod, Denmark, March 8, 2024. REUTERS/Tom Little/File Photo
He said that the slower pace of weekly prescriptions for Wegovy in the United States in the last couple of months was due to lower starter doses being supplied into the market.
“You can find different periods of times where you can say it’s plateauing but it’s not because of plateaued demand, it’s simply because of the supply into the market,” Fruergaard said.
Credit: Reuters
Weight loss drug semaglutide may offer relief for knee arthritis pain
Team Metabolic Health
New research highlights the potential for weight-loss medication to ease arthritis symptoms, offering hope for improved mobility and pain relief.
In a recent study published in The New England Journal of Medicine, researchers used a 68-week-long, extensive (61 centers across 11 countries), randomized clinical trial to evaluate Semaglutide’s pain- and weight-relieving performance in overweight arthritis patients.
A once-weekly 2.4 mg subcutaneous injection of the novel antidiabetic wonder drug was observed to reduce body weight (13.7%) and pain (WOMAC = 41) substantially more than similar placebo dosages (3.2% and 27.5 points, respectively).
Semaglutide consumption almost doubles physical function gains compared to placebo (12.0 versus 6.5 points), further promoting somatic health, weight loss, and healthy aging. Safety was similar between case (Semaglutide) and control (placebo) cohorts.
Together, these findings add yet another feather in Semaglutide’s growing cap of notable achievements, underscoring the drug’s potential to replace conventional pharmacological interventions not only in treating excessive body weight and diabetes but also associated conditions without added side effects over existing antidiabetic modalities.
Background
Arthritis is an umbrella term for several diseases characterized by painful and often debilitating inflammation in joints and connective tissues between adjoining bones. Osteoarthritis of the knee (OK) is the most common of these conditions, causing patients substantial pain, impaired mobility, and significantly reduced quality of life.
Several risk factors associated with OK genesis and progress have hitherto been identified, with obesity (excessive body weight) highlighted as a major contributing to the disease. High body mass index (BMI) has been shown to increase joint inflammation, exacerbating pain. Studies have elucidated that weight reductions following arthritis onset can noticeably improve pain and stiffness outcomes.
Conventional weight loss clinical interventions have historically helped improve short-term Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC). Unfortunately, with bariatric surgery representing a notable exception, most conventional weight loss modalities (dietary- and physical activity-based interventions) are found to provide highly patient-specific, short-term weight benefits that rarely persist for more than a few months and may involve significant alternations to patients’ daily routines.
Despite almost guaranteeing positive weight loss outcomes, bariatric surgery is an extensively invasive procedure with potential adverse side effects, making it a ‘last-case scenario’ in severe obesity. Unfortunately, today’s prevalent lifestyle (sedentary) and dietary choices (suboptimal diets such as the Western Dietary Pattern) are driving an unprecedented escalation in obesity incidence, underscoring the need for safe, long-lasting, efficient, and non-surgical interventions that both obesity-induces OK pain and addresses excessive body weight.
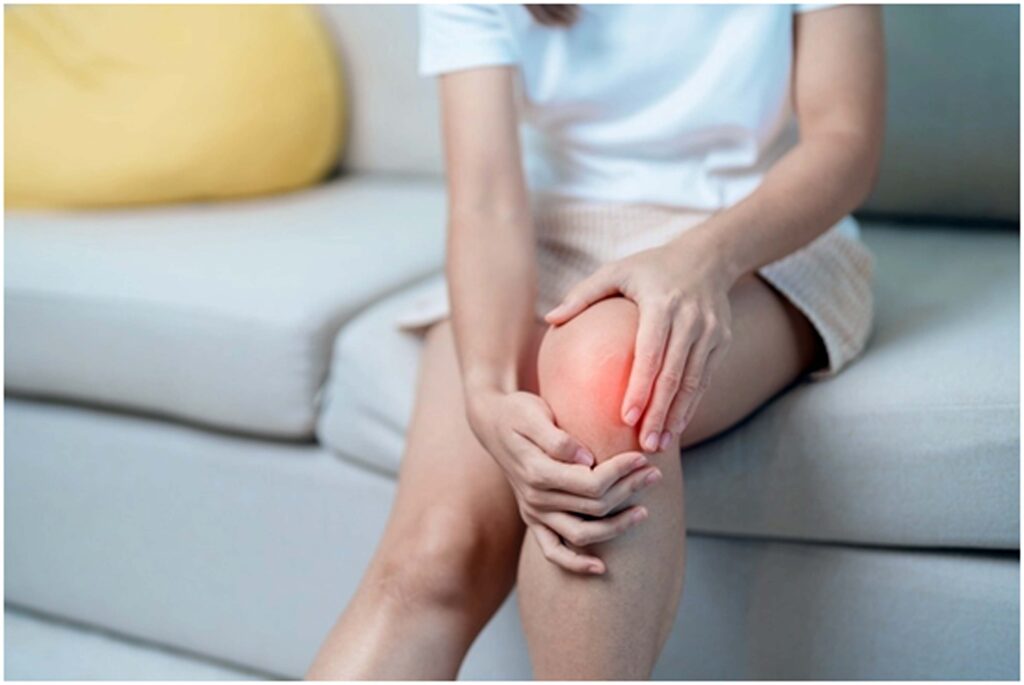
Study: Once-Weekly Semaglutide in Persons with Obesity and Knee Osteoarthritis. Image Credit: Jo Panuwat D/Shutterstock.com
About the study
The present study leverages a placebo-controlled clinical trial methodology to elucidate the potential application of Semaglutide, a recently developed antidiabetic drug, in treating weight-associated knee osteoarthritis.
Semaglutide is a glucagon-like peptide-1 (GLP-1) receptor agonist belonging to the incretin mimetic class. The drug has been extensively validated in obese/overweight and diabetic cohorts, with subcutaneous (usually 2.4 mg) injections administered weekly demonstrating generation-defining gains in long-term weight loss and diabetes management at reduced side-effect costs (compared with conventional pharmacological interventions).
While the benefits of weight management for OK pain relief have been previously established, the efficacy and safety of the drug in elderly OK patients remain unknown.
The study cohort was derived from the Semaglutide Treatment Effect in People with Obesity (STEP) 9 trial, a multicentre (61 sites across 11 countries) long-term Semaglutide assessment adopting double-anonymized, randomized, placebo-controlled study methodologies. Adult STEP participants (>18) presenting clinically validated OK and reporting WOMAC scores >40 (100-point scale) were included and randomized into cases and controls (2:1 ratio).
Experimental procedures included weekly intervention administrations (2.4 mg Semaglutide and equivalent placebo injections) alongside guidance on physical and dietary interventions that may improve weight- and/or OK outcomes. Outcomes of interest were reductions in BMI, WOMAC pain scores, or stiffness following 68 weeks of consistent intervention.
Study findings
Out of the thousands of STEP 9 trial participants, 407 met the study inclusion criteria and were assigned to the case (n = 271) and control (n = 136) cohorts. A majority of participants were female (81.6%), belonging to the White ethnicity (60.9%), and having a mean BMI of 40.3 kg m-2 (obesity is usually diagnosed using BMI ≥30 as a cutoff).
Study findings highlight Semaglutide’s performance, with the drug inducing a 13.7% decrease in BMI and a 41.7 point reduction in WOMAC scores in case-cohort members. In contrast, in tandem with dietary and physical activity advice, the placebo resulted in only 3.2% and 27.5 point reductions in placebo cohort members. Secondary endpoint analysis validated these findings and revealed that Semaglutide consumption almost doubled SF-36 physical-function scores (12.0 versus 6.5), underscoring its vast biological influence and multiorgan benefits.
Safety assessments presented statistically similar findings across both cohorts—10.0% of cases and 8.1% of controls reported adverse side effects (the most common being gastrointestinal tract distress). Severe adverse effects (requiring study discontinuation) were reported in 6.7% of cases and 3.0% of controls. These findings demonstrate that Semaglutide substantially outperforms placebos in excessive weight reduction, resulting in a cascade of OK benefits.
Conclusions
The present study provides clinical evidence for the knee arthritis-relieving benefits of Semaglutide compared to conventional pharmacological interventions against excessive BMI and its OK-associated outcomes (primarily pain and stiffness).
Study findings highlight that Semaglutide can achieve more than 10% additional weight loss compared to current non-surgical interventions, resulting in substantial 41.7-point pain reductions in OK patients.
While present, semaglutides’ side-effect inducting potential is comparable to conventional modalities. Together, these findings highlight Semaglutide as a safe and efficient means of promoting weight loss and reducing chronic pain in OK patients.
Credit: news-medical.net
Semaglutide may reduce Alzheimer’s risk in diabetics
Team Metabolic Health
Semaglutide linked to 40-70% lower risk of first-time Alzheimer’s diagnosis in type 2 diabetes patients compared to other antidiabetic medications.
A recent Alzheimer’s and Dementia study uses real-world data in the United States to evaluate the protective role of semaglutide against Alzherimer’s disease (AD).
Could semaglutide prevent AD?
In 2014, approximately 6.9 million American citizens 65 years of age and older were diagnosed with AD, with the prevalence of this disease predicted to reach 13.8 million by 2060. Although there is no cure for AD, several modifiable risk factors have been identified that can be targeted to reduce or delay the onset of both AD and dementia.
Study: Associations of semaglutide with first-time diagnosis of Alzheimer’s disease in patients with type 2 diabetes: Target trial emulation using nationwide real-world data in the US. Image Credit: Marc Bruxelle/Shutterstock.com
The U.S. Food and Drug Administration (FDA) has approved semaglutide, a glucagon-like peptide receptor agonist (GLP-1RA), to treat type 2 diabetes mellitus (T2DM) and obesity.
In addition to these indications, semaglutide can also support the management of various health conditions, including cardiovascular disease, depression, alcohol use, and smoking, all of which are also considered modifiable risk factors for AD. Thus, clinical trials are needed to assess whether semaglutide can delay or prevent AD.
About the study
The researchers of the current study hypothesized that semaglutide reduces the risk of developing AD in high-risk patients. To this end, an emulation target trial was conducted using the TriNetX Analytics platform based on real-world electronic health records (EHRs) of T2DM patients without a history of AD.
Seven target trials were emulated using 1,094,761 eligible patients from a nationwide database of U.S. patients. All study participants, both men and women, were 60 years of age or older.
None of the study participants used any antidiabetic medications within the past six months of the study commencement and were considered ‘new users.’ However, these patients received semaglutide prescriptions due to a history of hypertension, obesity, hypercholesterolemia, heart disease, or stroke.
For every patient population, a specified trial was conducted to compare semaglutide with other drugs used to treat T2DM including sodium-glucose cotransporter-2 inhibitors (SGLT2i), insulins, metformin, sulfonylureas (SUs), thiazolidinediones (TZDs), dipeptidyl-peptidase-4 inhibitors (DPP-4i) and other GLP-1Ras.
Based on EHR data, the first-time diagnosis of AD was considered the primary outcome, whereas AD-related medication prescriptions, such as donepezil, lecanemab, rivastigmine, aducanumab, memantine, and galantamine, were considered secondary outcomes. Each outcome was separately analyzed.
Study findings
The study cohort consisted of 17,104 new users of semaglutide and 1,077,657 new users of other antidiabetic medications. The effectiveness of semaglutide was compared with each of the studied antidiabetic medications.
Significant heterogeneity was observed between insulin and semaglutide recipients regarding ethnicity, age, sex, diagnosis of obesity, certain cardiovascular conditions, and AD-related risk factors. However, these groups were balanced after matching their propensity score.
T2DM patients who were prescribed semaglutide were significantly less likely to be diagnosed with AD during a three-year follow-up visit as compared with those prescribed other antidiabetic medications, irrespective of sex, gender, and obesity. The overall three-year risk of first-time AD diagnosis was almost two-fold higher in the general older population.
The three-year cumulative incidence curves comparing semaglutide with each antidiabetic medication indicated a divergence in the curve within 30 days that continued to separate thereafter. This finding highlights the role of semaglutide in delaying AD development with persistent effects.
Similarly, the subpopulation analysis indicated that semaglutide reduced the risk of first-time AD diagnosis as compared to other antidiabetic medication groups. The secondary outcomes analysis also indicated that semaglutide decreased AD-related medication prescriptions as compared to other antidiabetic medications in diabetic patients, with or without obesity.
How does semaglutide protect against AD?
Existing evidence suggests that GLP-1RAs like semaglutide may protect cognitive function by increasing authophagy and brain glucose uptake. Preclinical studies have also demonstrated that semaglutide can reduce neurotoxicity by preventing the proliferation of amyloid β (Aβ) plaques and tau tangles.
Clinical studies have produced similar results, with GLP-1RAs reducing cognitive impairment in patients with T2DM. In fact, one study conducted in Denmark found that patients with T2DM prescribed GLP-1RAs were at a 53% reduced risk of developing all-cause dementia.
Importantly, several other diabetic medications, including SGLT2i, may also reduce the risk of first-time AD diagnoses. SGLT2i, for example, reduces neuroinflammation, oxidative stress, and mitochondrial dysfunction. Nevertheless, the current study reports that semaglutide was significantly more protective against AD than other anti-diabetic medications, including SGLT2i.
Despite these observations, additional research is needed to elucidate the mechanisms through which semaglutide reduces the risk of developing AD.
Study limitations
The current study has several limitations, including the retrospective observational study design that used patient EHRs. This study design may not consider overdiagnoses, underdiagnoses, misdiagnoses, and unmeasured or uncontrolled confounders, which could generate biased results.
Furthermore, since semaglutide received FDA approval relatively recently, the follow-up period was limited to only three years.
Patient data was obtained from the TriNetX Analytics platform; therefore, the results require additional validation in analytics platforms. EHRs in TriNetX lack data on medication adherence and cognitive impairment tracking, which may influence study outcomes.
Conclusions
Semaglutide prescription reduced the risk of a first-time AD diagnosis by 40-70% in older populations with T2DM and other comorbidities.
Future studies are needed to investigate the effectiveness of this drug in other populations. The effect of semaglutide in mild cognitive impairment and other neurodegenerative diseases should be investigated.
Credit: news-medical.net
Weight-Loss Meds Like Wegovy Could Battle Alcoholism
Team Metabolic Health
Weight-loss and diabetes drugs like Ozempic, Wegovy, Mounjaro or Zepbound appear to help people battle alcoholism and opioid addiction, a new study finds.
People taking this class of drugs, called glucagon-like peptide-1 receptor agonists (GLP-1), have a 50% lower rate of drunkenness than people with addiction disorders not on the meds, researchers reported Oct. 17 in the journal Addiction.
GLP-1 patients also have a 40% lower rate of opioid overdose, results show.
GLP-1 drugs “exhibited a strong protective association with alcohol intoxication among those with alcohol use disorder,” concluded the research team led by Fares Qeadan, an associate professor of biostatistics at Loyola University in Chicago.
“Related prescriptions additionally displayed a strong protective association with opioid overdose among individuals with opioid use disorder,” the researchers added in a journal news release.
Key Takeaways
- Weight-loss drugs might help people battle addictions
- Alcoholics taking GLP-1 drugs had a 50% lower rate of intoxication
- Opioid users taking the drugs had a 40% lower risk of overdose

Credit: Adobe
GLP-1 drugs promote weight loss by mimicking a hormone produced in response to eating. Taking the drug helps stabilize blood sugar levels, decrease feelings of hunger and slow digestion, researchers noted.
The brain region targeted by GLP-1 “overlaps with the same processes that are responsible for the development and maintenance of addictive behaviors such as chronic substance use,” the researchers said.
For this study, researchers analyzed data on more than 500,000 people with a history of opioid addiction and 817,000 with a history of alcoholism. The data, drawn from 136 U.S. health systems, spanned January 2014 to September 2022.
Researchers tracked these folks’ use of GLP-1 drugs, as well as any bouts of intoxication or overdose they experienced.
“This study may introduce a promising new treatment for substance use disorders,” researchers said.
Credit: healthday.com
How will weight-loss drugs change our relationship with food?
Team Metabolic Health
Decisions on how these drugs will be used look likely to shape our future health and even what our society might look like.
And, as researchers are finding, they are already toppling the belief that obesity is simply a moral failing of the weak-willed.
Weight-loss drugs are already at the heart of the national debate. This week, the new Labour government suggested they could be a tool to help obese people in England off benefits and back into work.
That announcement – and the reaction to it – has held a mirror up to our own personal opinions around obesity and what should be done to tackle it.
Here are some questions I’d like you to ponder.
Is obesity something that people bring on themselves and they just need to make better life choices? Or is it a societal failing with millions of victims that needs stronger laws to control the types of food we eat?
Are effective weight-loss drugs the sensible choice in an obesity crisis? Are they being used as a convenient excuse to duck the big issue of why so many people are overweight in the first place?
Personal choice v nanny state; realism v idealism – there are few medical conditions that stir up such heated debate.
I can’t resolve all those questions for you – it all depends on your personal views about obesity and the type of country you want to live in. But as you think them over, there are some further things to consider.
Obesity is very visible, unlike conditions such as high blood pressure, and has long come with a stigma of blame and shame. Gluttony is one of Christianity’s seven deadly sins.
Now, let’s look at Semaglutide, which is sold under the brand name Wegovy for weight loss. It mimics a hormone that is released when we eat and tricks the brain into thinking we are full, dialling down our appetite so that we eat less.
What this means is that by changing only one hormone, “suddenly you change your entire relationship with food”, says Prof Giles Yeo, an obesity scientist at the University of Cambridge.
And that has all sorts of implications for the way we think about obesity.
It also means for a lot of overweight people there is a “hormonal deficiency, or at least it doesn’t go up as high”, argues Prof Yeo, which leaves them biologically more hungry and primed to put on weight than someone who is naturally thin.
That was likely an advantage 100 or more years ago when food was less plentiful – driving people to consume calories when they are available, because tomorrow there may be none.
Our genes have not profoundly changed in a century, but the world we live in has made it easier to pile on the pounds with the rise of cheap and calorie-dense foods, ballooning portion sizes and towns and cities that make it easier to drive than walk or cycle.
These changes took off in the second half of the 20th Century, giving rise to what scientists call the “obesogenic environment” – that is, one that encourages people to eat unhealthily and not do enough exercise.
Now one in four adults in the UK is obese.
Wegovy can help people lose around 15% of their starting body weight before the benefits plateau.
Despite constantly being labelled a “skinny drug” this could take someone weighing 20 stone down to 17 stone. Medically, that would improve health in areas like heart attack risk, sleep apnoea and type 2 diabetes.
But Dr Margaret McCartney, a GP in Glasgow, cautions: “If we keep putting people into an obesogenic environment, we’re just going to increase need for these drugs forever.”
At the moment the NHS is planning to prescribe the drugs only for two years because of the cost. Evidence shows that when the injections stop, the appetite comes back and the weight goes back on.
“My big concern is the eye is taken off the ball with stopping people getting overweight in the first place,” says Dr McCartney.
We know the obesogenic environment starts early. One in five children is already overweight or obese by the time they start school.
And we know that it hits poorer communities (in which 36% of adults in England are obese) harder than wealthier ones (where the figure is 20%), in part due to the lack of availability of cheap, healthy food in those less affluent districts.
But there is often a tension between improving public health and civil liberties. You can drive, but you have to wear a seatbelt; you can smoke, but with very high taxes alongside restrictions on age and where you can do it.
So here are some further things for you to consider. Do you think we should also tackle the obesogenic environment or just treat people when it’s starting to damage their health? Should government be far tougher on the food industry, transforming what we can buy and eat?
Should we be encouraged to go Japanese (a rich country with low obesity) and have smaller meals based around rice, vegetables and fish? Or should we cap the calories in ready meals and chocolate bars?
What about sugar or junk-food taxes? What about wider bans on where calorie-dense foods can be sold or advertised?
Prof Yeo says if we want change then “we’re going to have to compromise somewhere, we’re going to have to lose some liberties” but “I don’t think we’ve come to a decision within society, I don’t think we’ve debated it”.
In England, there have been official obesity strategies – 14 of them across three decades and with very little to show for it.
They included five-a-day campaigns to promote eating fruit and veg, food labelling to highlight calorie content, restrictions on advertising unhealthy food to children and voluntary agreements with manufacturers to reformulate foods.
But although there are tentative signs that child obesity in England may be starting to fall, none of these measures have sufficiently altered the national diet to turn the tide on obesity overall.
There is one school of thought that weight-loss drugs may even be the event that triggers the change in our meals.
“Food companies profit, that’s what they want – the only ray of hope I have is if weight-loss drugs help a lot of people resist buying fast foods, can that start the partial reversal of the food environment?” asks Prof Naveed Sattar from the University of Glasgow.
As weight-loss drugs become far more available, deciding how they will be used and how that fits into our wider approach to obesity will need to be addressed soon.
At the moment we are only dipping our toes in the water. There is limited supply of these drugs and because of their huge expense, they are available on the NHS to relatively few people and for a short time.
That is expected to change dramatically over the next decade. New drugs, such as tirzepatide, are on the way and the pharmaceutical companies will lose their legal protections – patents – meaning other companies can make their own, cheaper versions.
In the early days of blood-pressure-lowering medicines or statins to reduce cholesterol, they were expensive and given to the few who would benefit the most. Now around eight million people in the UK are taking each of those drugs.
More from InDepth
This young disabled man dreamed of having a job – the system had other ideas
A Japanese boy was killed in China. Was cyber-nationalism to blame?
How have social media algorithms changed the way we interact?
Prof Stephen O’Rahilly, director of the MRC Metabolic Diseases Unit, says blood pressure was tacked with using a combination of drugs and societal change: “We screened for blood pressure, we advised about lower sodium [salt] in foods and we developed cheap, safe and effective blood pressure drugs.”
That’s analogous, he says, to what needs to happen with obesity.
It is still not clear how many of us will end up on weight-loss medication. Will it only be for those who are very obese and at medical risk? Or will it become preventative to stop people becoming obese?
How long should people take weight-loss drugs for? Should it be for life? How widely should they be used in children? Does it matter if people using the drugs are still eating unhealthy junk food, just less of it?
How quickly should weight-loss medications be adopted when we still do not know the side-effects of long term use? Are we OK with healthy people taking them entirely for cosmetic reasons? Could their availability privately widen the obesity and health gap between rich and poor?
So many questions – but, as yet, few clear answers.
“I don’t know where this is going to land – we’re on a voyage of uncertainty,” says Prof Naveed Sattar.
Credit: BBC
Eli Lilly vs. Novo Nordisk: Which Weight Loss Stock is The Better Opportunity Over The Next 10 Years?
Team Metabolic Health
Glucagon-like peptide-1 (GLP-1) agonists have taken the healthcare world by storm, emerging as mainstream treatments for patients with diabetes or obesity. Some of these medications include Novo Nordisk’s (NYSE: NVO) Ozempic, Wegovy, Rybelsus, and Saxenda, and Eli Lilly’s (NYSE: LLY) Mounjaro and Zepbound.
Below, I’ll dig into which pharmaceutical stock I think is the better buy for the long run. While Novo Nordisk and Lilly each carry encouraging prospects, I see one of these companies as the superior opportunity.
Image source: Getty Images
The case for Novo Nordisk
Right now Novo Nordisk has a considerable lead on Lilly in GLP-1 market share, and a couple of notable wins have me thinking this lead will widen.
Earlier this year, J.P. Morgan released a report outlining the potential for GLP-1 treatments in other markets. Specifically, research suggests that GLP-1 drugs have applications outside of weight loss. Such areas include sleep apnea, arthritis, kidney disease, cardiovascular disease, and Alzheimer’s.
Although becoming a multi-platform breakthrough could serve as a catalyst for both Novo Nordisk and Lilly, I think Novo Nordisk has the edge for now. Back in March, Wegovy received an expanded indication from the Food and Drug Administration (FDA) to treat obesity care patients who are also at risk of major cardiovascular events.
A few months later, Wegovy was approved to enter yet another market: China, a geographic region where obesity rates are quite high.
All things considered, I think Novo Nordisk’s momentum in the GLP-1 realm could be kicking into a new gear.
The case for Eli Lilly
To be fair, while Novo Nordisk has the lead in the GLP-1 arena, I have to note that Lilly’s Mounjaro and Zepbound have not been on the market nearly as long as its competitor’s medications have. And although Mounjaro and Zepbound have already reached blockbuster status, Lilly’s own CEO admits that the company hasn’t been investing as heavily in marketing campaigns for these medications as it could be.
I see this as a strategic move on Lilly’s end; it seems the company is content taking its time building a presence in the market, and is not in a rush to oversell its products. Such patience could be a wise move in the long run as Mounjaro and Zepbound become more popular.
Where Eli Lilly starts to really separate itself from Novo Nordisk is in other markets. For example, over the summer Lilly’s Alzheimer’s drug received approval from the FDA. More recently, the company also received the nod to enter the eczema market via its newly approved drug Ebglyss.
Lastly, Lilly is making some interesting moves relating to the use of artificial intelligence (AI) in the healthcare world. The company is working with OpenAI to help develop new medications to combat antimicrobial resistance (AMR).
The bottom line
At a high level, both Novo Nordisk and Eli Lilly appear to have strong road maps ahead. But thinking long-term, I see Lilly as the clear-cut winner. Novo Nordisk’s position as ruler of the GLP-1 realm should eventually normalize as Lilly gains more market share and other potential players enter the space as well.
Beyond weight loss treatments, Lilly has some billion-dollar opportunities both with its Alzheimer’s and eczema medications, and in the use of AI in drug development — but none of these efforts have started bearing fruit for the company yet.
For me, Lilly’s diverse platform compared to Novo Nordisk’s is attractive, and I’m confident that Eli Lilly has more upside potential than its competition does.
Credit: Yahoo
Novo’s trial of weight-loss drug shows improvement in fatty liver disease
Team Metabolic Health
Novo Nordisk (NOVOb.CO), opens new tab said on Friday its weight-loss drug met the main goal of a late-stage trial in patients with a type of fatty liver disease by reducing scarring of the organ without worsening the condition.
The study used 2.4 milligram dose of semaglutide to treat a liver condition called metabolic dysfunction-associated steatohepatitis, or MASH, in one part of the trial involving 800 patients.
Semaglutide is sold as Wegovy for weight-loss and Ozempic for diabetes.
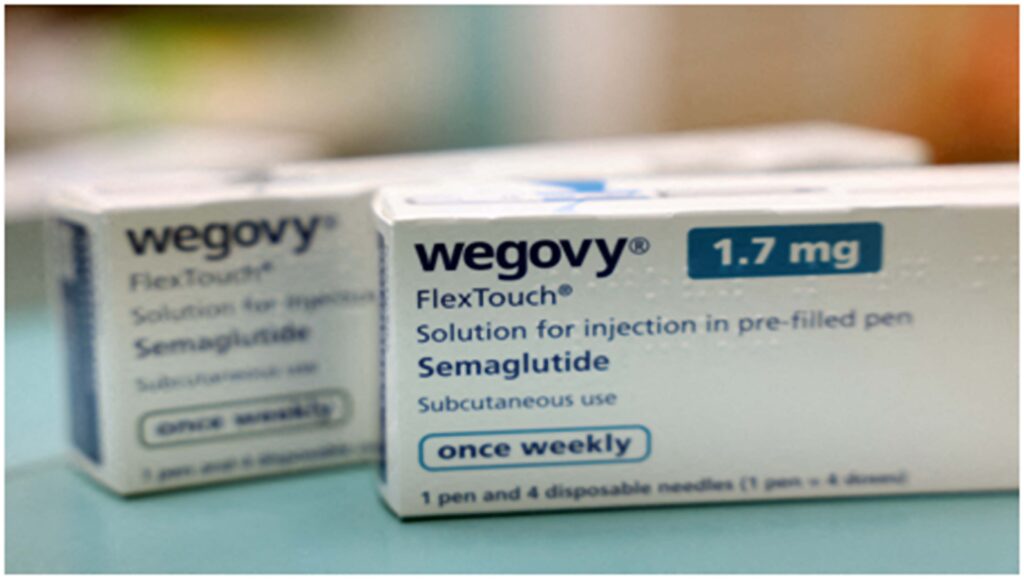
Boxes of Wegovy made by Novo Nordisk are seen at a pharmacy in London, Britain. REUTERS/Hollie Adams/File Photo
At 72 weeks, 37% of patients on the drug showed improvement in liver scarring, with no worsening of steatohepatitis, an inflammation of the organ due to excess fat deposits, compared with 22.5% of those on placebo.
In the trial, 62.9% of those on the drug also achieved resolution of steatohepatitis compared with 34.1% on placebo.
MASH, which was earlier known as NASH or non-alcoholic steatohepatitis, affects around 5% of adults in the U.S., according to the American Liver Foundation, making it a large patient population.
But Madrigal Pharmaceuticals’ (MDGL.O), opens new tab Rezdiffra is the only approved treatment.
“The long-term perspective paints a positive picture as large pharma has resources to substantially grow this market to create an even larger opportunity for Rezdiffra,” said Piper Sandler analyst Yasmeen Rahimi.
Shares of Novo Nordisk rose 1% in Copenhagen, while Madrigal added 22% in New York. Drug developer Akero Therapeutics (AKRO.O), opens new tab rose 5%.
Novo’s drug showed a 14.5% difference between improvement in fibrosis after adjusting for the placebo, compared to 12% shown by 100 mg dose of Rezdiffra in a separate late-stage trial, opens new tab.
Lilly’s tirzepatide – the active ingredient popular diabetes drug Mounjaro and weight-loss drug Zepbound – helped up to 74% of patients achieve absence of the disease with no worsening of scarring in a mid-stage trial.
Jefferies analyst Peter Welford expects Wegovy to generate $2 billion at the peak of its sales outside of obesity from MASH patients.
Novo Nordisk expects to file for regulatory approvals in the U.S. and the European Union in the first half of 2025.
Novo and Lilly are also testing their weight-loss drug for several other conditions, including Alzheimer’s disease.
Credit: Reuters
Health Rounds: No need to stop GLP-1 drugs before surgery for most patients
Team Metabolic Health
In a practice-changing guideline reversal, medical societies advised, opens new tab on Tuesday that most patients do not need to stop taking GLP-1 diabetes and weight-loss drugs before surgery, a ruling supported by a study presented this week at a medical meeting of gastrointestinal doctors.
The study also suggests that patients might benefit from following a clear liquid diet for a day in advance, although that was not included in the new guidelines.
Patients typically fast before undergoing anesthesia in order to empty the stomach. An empty stomach allows for better examination via endoscopy and lowers the risk of aspiration, a life-threatening complication involving inhalation of gastric contents.
Because GLP-1 drugs such as Novo Nordisk’s (NOVOb.CO), opens new tab Ozempic and Wegovy and Zepbound and Mounjaro from Eli Lilly (LLY.N), opens new tab slow stomach emptying, surgeons had been requiring patients to stop those drugs well in advance of anesthesia in order to ensure an empty stomach.
But a new review of 35 studies involving more than 714,000 patients undergoing upper-gastrointestinal endoscopy found no extra risk of aspiration in patients who had not paused their use of GLP-1 drugs beforehand.
Boxes of Ozempic and Wegovy made by Novo Nordisk are seen at a pharmacy in London, Britain. REUTERS/Hollie Adams
They were compared with patients who either were not using the drugs or were using them but had stopped them well in advance of surgery.
The findings were presented by Dr. Violeta Popov of NYU Langone Health NY VA Harbor Health System on Wednesday at the American College of Gastroenterology, opens new tab meeting in Philadelphia.
Procedures more often had to be stopped early in patients who had not stopped the GLP-1 drugs, possibly because significant amounts of food remained in the stomach, her team found. However, retained gastric contents were not a problem in a subset of patients taking GLP-1 drugs who had been on a liquid diet for 24 hours because they were scheduled for colonoscopy.
Therefore, the researchers suggest, it might be best to follow a 24-hour clear liquid diet prior to GI endoscopy without discontinuing GLP-1 therapy.
Esophagus cancer precursor being seen at younger ages
A pre-malignant condition of the esophagus is becoming more common at younger ages, researchers have found, suggesting potential benefits from earlier screening.
Barrett’s esophagus is usually diagnosed around age 60, but a new study of more than 2.6 million patients found a significantly increasing trend of young-onset Barrett’s esophagus from 2014 to 2023, researchers reported at the gastroenterology meeting.
In Barrett’s esophagus, stomach acid has damaged the lining of the lower esophagus, increasing the risk for cancer.
Treatment may include medicines and surgery. Patients with mild cases are advised to undergo endoscopy on a regular basis to monitor the cells in the esophagus lining.
In the new study, 20% of participants had been diagnosed before age 50, with early-stage disease in nearly all cases.
Risk factors in younger patients were similar to those in older patients, including hiatal hernia, gastrointestinal reflux, smoking, and high body mass index, Dr. Anila Vasireddy of the University of Pennsylvania Health System reported.
“Our study validates that conventional risk-factors of Barrett’s esophagus in older patients also predict young-onset Barrett’s esophagus,” her team said in a written summary.
“Screening… before the age of 50 may have a significant impact on early detection of esophageal adenocarcinoma,” they said.
U.S. patients undertreated for alcohol use disorder
Drug treatment of alcohol use disorder is underused in U.S. patients and particularly in patients with alcoholic liver disease, researchers reported at the Philadelphia gastroenterology meeting.
Pharmacotherapy is an important tool for treating addiction and preventing progression of liver disease. But among 26,985 commercially insured patients with alcohol use disorder who did not have liver disease, only 14.5% had been prescribed medication. That rate dropped to 2.3% among 1,201 alcohol abuse patients with liver disease, the researchers said.
Patients with the most severe alcoholic liver disease had the lowest odds of receiving drug therapy for their alcoholism, Dr. Alex Jones of the University of Texas Southwestern Medical Center reported.
Gabapentin was the most commonly prescribed medication in the study, followed by oral naltrexone and topiramate.
“Providers caring for patients with alcoholic liver disease should consider this underutilized therapy, or refer for psychiatric consultation when appropriate,” the researchers said.
Credit: Reuters
Leading Generics Drugs Maker Slapped With €467 EU Antitrust Fine
Team Metabolic Health
Teva described the EU regulator’s decision as “extreme, untested and factually unsupported.”
The European Commission has hit the world’s largest maker of generic drugs with a €462.6 million fine for breaching the bloc’s competition rules.
It is the first time in the history of the EU’s antitrust division that a company has been fined for misusing the EU patent system and systematically disparaging rivals.
In a statement posted to its website, Teva, an Israel-headquartered multinational, described the decision as being underpinned by “extreme, untested, and factually unsupported” legal theories. Noting that the company was “well prepared financially to mount a defense,” it said it would appeal the decision.

Credit: olrat/Adobe Stock
Teva described the EU regulator’s decision as “extreme, untested and factually unsupported.”
The European Commission has hit the world’s largest maker of generic drugs with a €462.6 million fine for breaching the bloc’s competition rules.
It is the first time in the history of the EU’s antitrust division that a company has been fined for misusing the EU patent system and systematically disparaging rivals.
In a statement posted to its website, Teva, an Israel-headquartered multinational, described the decision as being underpinned by “extreme, untested, and factually unsupported” legal theories. Noting that the company was “well prepared financially to mount a defense,” it said it would appeal the decision.
“Temu takes its obligations under the DSA seriously, continuously investing to strengthen our compliance system and safeguard consumer interests on our platform,” the company added in a statement sent to Law.com International. “We will cooperate fully with regulators to support our shared goal of a safe, trusted marketplace for consumers.”
According to Brussels officials, the Israeli drugmaker abused its dominant position in Belgium, Czechia, Germany, Italy, the Netherlands, Poland and Spain with the goal of slowing down competition and artificially extending the exclusivity of its prize multiple sclerosis drug Copaxone. The company did this, officials said, by obstructing the market entry and the uptake of competing, lower-cost medicines that relied on the same active ingredient as Copaxone.
The EU’s Luxembourg-based General Court will rule on Teva’s appeal, which could take up to two years. Jonas Koponen, a partner in Cooley’s Brussels office, told Law.com International that patent, regulatory and marketing strategies are “normal and legitimate means of competition.” He said the EU court had made clear in its previous rulings that dominant firms are allowed to resort to “aggressive strategies,” as long as they are based on “competition on the merits” and not prone to foreclose rivals.
“If this decision is appealed, a key question for the Court would be to determine whether the conduct that the Commission found abusive amounts to “competition on the merits” in the specific context of the pharma sector,” he said. “But this is a nebulous notion, and it would be important for the Court to clarify when legitimate business strategies ‘cross the line’—a blurred line risks stifling legitimate and healthy competition.”
Another large company also has ended up in the EU’s crosshairs: EU officials have opened an investigation against Temu under the bloc’s Digital Services Act over concerns that the popular Chinese online retail platform sold illegal products and designed the service in an addictive way.
Over the next few months, the EU regulator will also look into the systems used by Temu to recommend purchases to users, as well as the data access the company has offered researchers. If Brussels officials find the company has indeed breached the bloc’s online safety law, Temu could face a fine of up to to 6% of its worldwide annual turnover.
Credit: law.com
How Asian pharma suppliers cash in on Ozempic copies
Team Metabolic Health
Just over a year ago, New Zealand customs officials started to intercept batches of injectable medications labelled Fitaro and Orsema, developed by a little-known Bangladeshi drugmaker, Incepta Pharmaceuticals.
The injectable pens, 14 of which were seized at the border, contained semaglutide, a patented substance that helps control blood sugar levels and appetite and is the key ingredient in Novo Nordisk’s (NOVOb.CO), opens new tab blockbuster drugs Ozempic and Wegovy, according to data from New Zealand’s medicines regulator Medsafe, reviewed by Reuters.
The Incepta drugs are part of an Asia-based supply chain manufacturing and exporting cheaper copies of Ozempic across the world, Reuters has found, driven by a spike in global demand for the drug.
Ozempic was developed for type 2 diabetes but its active ingredient semaglutide is effective in promoting weight loss. The market for such weight-loss treatments, which Novo Nordisk is targeting with anti-obesity treatment Wegovy, is forecast to reach $150 billion by the early 2030s.

People sit in a booth of Shanghai LongTide Biotechnology at a pharmaceutical exhibition in Shenzhen, Guangdong province, China. REUTERS/Andrew Silver/File Photo
According to a Reuters review, at least 106,000 packs of semaglutide-based medicines made in Asia by Incepta have been shipped to 12 foreign markets including countries like the United States and Britain where Ozempic is protected by patents.
Incepta did not respond to multiple requests for comment about Fitaro and Orsema, which are approved for sale in Bangladesh, according to public records and information provided by a local regulatory official. The official with the Bangladesh Directorate General of Drug Administration, who declined to be named because he was not authorized to speak to the media, said Bangladeshi regulators had given Incepta permission to export Fitaro or Orsema but only provided it had won approval from receiving countries. The injectable pens, which are not authorised for use in New Zealand, were referred to Medsafe between August 2023 and May 2024 and destroyed, data from the regulator showed.
Medsafe told Reuters the Fitaro and Orsema batches that were destroyed appeared to be for personal use but did not comment on whether the medicines carried any health risk.
“Medicines that have been imported from overseas will not have been assessed and approved by Medsafe, so carry a significant risk as there is no assurance they have been made to an acceptable level of quality,” the regulator added in response to a Reuters query about imports of semaglutide-based drugs.
Reuters has previously reported that semaglutide drugs from Bangladesh were sold on India-based online marketplace IndiaMART. The latest reporting shows that the international distribution of semaglutide drugs not made by Novo Nordisk is much wider.
The data surveyed by Reuters came from pharmaceutical regulators in Australia, Brazil, New Zealand and the United States; information from a commercial customs data provider for Kenya, Uzbekistan, Venezuela, Hong Kong and the United Arab Emirates; and records of intercepted drugs from Britain, Switzerland and Ireland.
In addition, an interview with a trade show exhibitor, a review of data from the commercial customs data provider, and from Brazil’s Justice Ministry showed that six little-known companies, four of which are based in Asia, manufacture semaglutide-based medicines and that their products are shipped overseas.
At least three of these firms imported the key ingredient from China and at least one of their products was promoted online and in person outside the country of origin, according to the commercial customs data provider’s data, an interview with an employee at Chinese supplier Nanjing Hanxin Pharmaceutical Technology, and a website and social media app reviewed by Reuters.
These players take advantage of global patent exemptions allowed for less developed countries and instances of loose patent enforcement in countries including in China, the Reuters review shows.
Novo Nordisk told Reuters it is the only approved manufacturer of semaglutide globally, and it could not vouch for the safety or effectiveness of products claiming to contain semaglutide made by other manufacturers.
Even though Novo Nordisk’s semaglutide is protected by international licences, countries like Bangladesh and Laos, classified as least developed nations by the United Nations, enjoy exemptions from industry patent rules.
The Danish firm, which has quickly become Europe’s most valuable company with a market capitalisation of around $400 billion, states on its website that it does not enforce patents in less developed countries. Given the frenzied demand for Ozempic, the financial impact of possible patent infringement on Novo Nordisk is currently limited. “Illegal versions of the drugs today do not cannibalize Novo’s sales given they are selling every dose they can produce,” said Nicholas Anderson, portfolio manager and managing director at global asset management firm Thornburg Investment Management, which owns Novo Nordisk stocks.
However, such copies are raising healthcare concerns. Medicines regulators in at least six countries including the U.S., Britain and Ireland have rejected, destroyed or seized some of Incepta’s semaglutide-based drugs, according to drug regulator records and responses from regulators to Reuters’ queries. In one case, unauthorised semaglutide was recalled in South Africa in December, because of potential health risks, according to a public notice posted in January by the local medicines regulator. The authority told Reuters the ingredient was sourced from a supplier in China not authorised to produce the ingredient in Ozempic, without providing more details.
“The semaglutide, said to be found in this unauthorised substance, may contain unexpected impurities or degradation products which can have unknown effects on patients,” the notice said.
Reuters found no evidence that these products would have caused any harm to patients, but their spread could add to public health concerns about a sector also threatened by fake Ozempic.
Supply of semaglutide drugs across the world
PARALLEL SUPPLY CHAIN
The official with the Bangladesh Directorate General of Drug Administration said Orsema was approved in Bangladesh and considered safe. Fitaro is also approved for sale, public records show.
A clinic in the capital Dhaka has prescribed Incepta’s Fitaro injector pens to around 20 patients, all foreigners based in Bangladesh, according to a manager, who declined to be named or identify the clinic due to the sensitivity around the treatment. “When patients found out that Fitaro was available in Bangladesh at a maximum monthly cost of around $60 a month, (against) $650 in the U.S. (for Wegovy), they didn’t seem particularly focused on who the manufacturer was,” the manager said. In Laos, semaglutide-based medicines can only be legally produced and distributed for national use, Davone Duangdany, director of the drug and medical device control division within the Laos health ministry, told Reuters. But some Chinese companies have been promoting Laos-produced semaglutide tablets in China, where Novo Nordisk’s patent is due to expire in 2026 or earlier if it loses a legal challenge. At an industry exhibition in Shanghai in June that Reuters attended, ingredient manufacturer Nanjing Hanxin Pharmaceutical Technology displayed boxes of Semagcare semaglutide tablets, manufactured by Laos-based Boten Elemento Pharma.
Abdu Zoghbi, business development director of Nanjing Hanxin, told Reuters that his company provides semaglutide to the Laos-based drugmaker.
“We don’t know which countries (Semagcare is sold to) but we are doing the promotion because once they sell more, we sell more API (active pharmaceutical ingredient) to them,” he told Reuters when asked about why it was showcasing the drug at the expo.
Boten Elemento Pharma’s Semagcare tablets appeared on sale on a Chinese language website and also a Chinese social media app, according to a Reuters review. Sales of semaglutide by a Chinese company could amount to an infringement of Novo Nordisk’s China patent, said Frank Yang, senior associate at Marks & Clerk Intellectual Property Agency in reply to a Reuters query about possible licences breaches.
A spokeswoman for Novo Nordisk said the company does not produce the ingredient in China.
The China National Intellectual Property Administration declared the Danish drugmaker’s patent invalid in September 2022. However, Novo Nordisk successfully appealed this decision.
Novo Nordisk told Reuters it is now awaiting a court decision on a subsequent appeal.
“We hope to see a continued trend in supporting and protecting innovation during patent invalidation proceedings,” a Novo Nordisk spokesperson said in response to questions about whether it was enforcing its patent in China.
Contacted by Reuters by fax, the Chinese medicine regulator did not reply to queries about quality controls at the Chinese firms making semaglutide.
A second Chinese firm, Shanghai Longtide Biotechnology, which described itself as a biotechnology company, also displayed a box of Semagcare tablets at its booth at a separate trade show in Shenzhen that Reuters also attended. Reuters contacted Boten Elemento Pharma through its website but the company did not respond. A business registered as Shanghai Longtide Biotechnology did not reply to requests for comment.
BENDING BOUNDARIES A third Chinese biotechnology firm, Zhejiang Peptites Biotech, is among the suppliers of semaglutide to Incepta, the data from the commercial customs data provider showed. The Bangladeshi drugmaker has imported at least 892 grams of semaglutide valued at about $805,000 between 2020 and 2024 from mainland China and Hong Kong, according to a Reuters calculation based on the customs data provider’s shipment data for Zhejiang Peptites Biotech and other suppliers. Zhejiang Peptites Biotech also supplied at least 25.6 kg of semaglutide, valued about $2.8 million, to Russian drugmaker Geropharm in 2023 and 2024, according to Reuters calculations based on the customs data provider’s data.
Geropharm can use inventions protected by Russian patents to provide semaglutide-based medication to the local population without Novo’s consent until the end of December, according to a Russian government decree issued in December 2023.
The Russian company said Zhejiang Peptites Biotech’s supply of semaglutide is carried out in accordance with a contract and it does not export the finished drug, Semavic, abroad.
However, Semavic was exported from Russia multiple times to the breakaway Georgian region of Abkhazia, information from the commercial customs data provider reviewed by Reuters showed.
Zhejiang Peptites Biotech did not respond to a request for comment on shipments of semaglutide to Incepta and Geropharm.
The customs data showed that it was not only Chinese firms supplying semaglutide: Incepta has imported the ingredient from Swiss generic drugmaker Bachem. (BANB.S), opens new tab A spokesperson for Bachem said it produces semaglutide for pharmaceutical companies for research and development purposes only and declined to comment on its relationship with Incepta. Medicines regulator Swissmedic told Reuters Bachem was authorised to export semaglutide, but added Swissmedic was “not supervising patents”.
Credit: Reuters
Health Rounds: Acupuncture reduces leg pain from a herniated disk
Team Metabolic Health
Acupuncture eases leg pain caused by a herniated disk
Acupuncture can alleviate pain and improve function in patients with chronic sciatica from a herniated disk, according to a Chinese study.
At six hospitals in China, researchers recruited 216 patients with herniated disks causing sciatica for at least three months and randomly assigned them to receive 10 sessions of acupuncture or sham acupuncture over 4 weeks.
Two standard scoring tools showed significantly greater improvements in the acupuncture group, they reported in JAMA Internal Medicine, opens new tab.
At week 4, scores on the visual analog scale for leg pain had decreased by an average of 30.8 mm in the acupuncture group versus 14.9 mm in the sham group.
Scores on the Oswestry Disability Index decreased by 13.0 points in the acupuncture group compared with 4.9 points in the control group after four weeks.
The improvements in the acupuncture group were still evident a year later, the researchers found.
An editorial, opens new tab published with the study called it methodologically rigorous and said “acupuncture adds an effective, evidence-based, non-pharmacological treatment to address a common chronic condition.”
Experimental electric patch kills wound bacteria
Early testing of a patch that delivers imperceptible electric currents to the skin demonstrated promising results as a potential alternative to antibiotics for killing bacteria in wounds and skin infections, researchers say.
“This opens up exciting possibilities for drug-free treatments, especially for skin infections and wound healing, where antibiotic-resistant bacteria pose a serious challenge,” Bozhi Tian of the University of Chicago, who is helping to develop the patch, said in a statement.
Tian’s team tested whether Staphylococcus epidermidis, a common bacterium that can cause serious infections if it enters the body, would respond to electrical stimulation.
They found that small electric currents can elicit responses from S. epidermidis, but only in an acidic environment that’s found on healthy skin. Under the ideal acidic condition, the electricity treatment stopped 99% of the biofilm, a cluster of bacteria that blocks drugs and leads to persistent infections.
That was not the case in wounds that have trouble healing, because they are not acidic. To get around that, the researchers designed a skin patch that contains electrodes and a gel that provides an acidic environment.
In tests on pig skin inoculated with S. epidermidis, the team observed a significant decrease in biofilm coverage and nearly 10 times reduction in S. epidermidis cells compared to an untreated sample, according to a report in the Cell Press journal Device, opens new tab.
The researchers saw the same effect when they tested the patches on catheter surfaces.
With further research, they said they hope to develop a wearable patch with a wireless circuit to control infections without drugs.
Vigorous, not moderate, exercise curbs hunger
A vigorous workout does more to suppress hunger levels in healthy adults than moderate exercise, and females may be especially susceptible to this response, according to a small study.
“Our research suggests that high-intensity exercise may be important for appetite suppression, which can be particularly useful as part of a weight loss program,” study leader Kara Anderson of the University of Virginia said in a statement.
“Exercise should be thought of as a ‘drug,’ where the ‘dose’ should be customized based on an individual’s personal goals,” she added.
In eight men and six women, researchers analyzed the effects of exercise intensity on appetite and on levels of ghrelin, a hormone associated with perceptions of hunger.
After high-intensity exercise, ghrelin levels and appetites were lower than after moderate intensity exercise, Anderson said.
“Moderate intensity either did not change ghrelin levels or led to a net increase,” the researchers reported in the Journal of the Endocrine Society, opens new tab.
Along with appetite, ghrelin is known to affect energy balance, glucose homeostasis, immune function, sleep, and memory.
The report points out that ghrelin is present in the blood in two different forms. Females had higher levels of total ghrelin at baseline compared with males, and one form of the hormone was reduced after intense exercise only in females, but the implications of these sex differences are unclear, the researchers said.
Credit: Reuters
Low-level arsenic exposure in water linked to increased heart disease risk
Team Metabolic Health
Participants exposed to arsenic levels at or above the EPA limit had a 42% higher risk of ischemic heart disease, while even moderate exposure increased risk by 20%.

Study: Gut microbiome dysbiosis is associated with lumbar degenerative spondylolisthesis in symptomatic patients. Image Credit: CandyRetriever/Shutterstock.com
In a recent study published in the Environmental Health Perspectives, a group of researchers evaluated the relationship between long-term exposure to inorganic arsenic in drinking water (wAs) supplies and the risk of ischemic heart disease (IHD) (a condition caused by reduced blood flow to the heart muscle, often due to narrowed coronary arteries) and cardiovascular disease (CVD) among women in the California Teachers Study (CTS) cohort.
As is a significant environmental concern linked to various chronic diseases in the United States (U.S.), particularly CVD. Health organizations, including the American Heart Association, acknowledge the increased CVD risk associated with arsenic exposure, particularly at high levels (>100 μg/L). Although the U.S. Environmental Protection Agency lowered the maximum contaminant level for arsenic in community water supplies from 50 μg/L to 10 μg/L in 2006, lower levels may still pose risks. Limited studies have explored the effects of long-term exposure to these lower concentrations on CVD, highlighting the need for further research to understand their safety.
Credit: news-medical.net
Rise in weight-management glucose-lowering drug prescriptions in type 1 diabetes patients
Team Metabolic Health
Prescriptions of GLP-1RAs and SGLT2 inhibitors in type 1 diabetes patients rose from 2010 to 2023, especially among those with elevated cardiorenal risk.
In a recent study published in JAMA Network Open, researchers from the United States of America (US) examined the prescribing trends for glucagon-like peptide-1 receptor agonists (GLP-1RAs) and sodium-glucose cotransporter 2 inhibitors (SGLT2i) in individuals with type 1 diabetes (T1D) from 2010 to 2023.
They found a significant increase in prescribing rates for both drug classes, with higher prescriptions for GLP-1RAs in patients with obesity and for SGLT2i in patients with cardiovascular and renal conditions.

Receptor Agonist and SGLT2 Inhibitor Prescribing in People With Type 1 Diabetes. Image Credit: Alones/Shutterstock.com
Background
GLP-1RAs and SGLT2i are newer glucose-lowering drug classes that have been reported to offer significant cardiorenal benefits and weight management advantages. Although these drugs have not been approved for the management of T1D, there is evidence suggesting their current use in this population.
In the present study, researchers investigated the prescription trends of GLP-1RAs (albiglutide, dulaglutide, semaglutide, exenatide, liraglutide, lixisenatide, and tirzepatide) and SGLT2i (canagliflozin, empagliflozin, dapagliflozin, and ertugliflozin) in patients with T1D.
About the study
The present study utilized data from Epic Cosmos, a large electronic health record (EHR) database covering over 257 million US residents, to examine trends in prescribing GLP-1RAs and SGLT2i for individuals with T1D. A total of 405,019 were included in the broader T1D population.
The mean age of the overall T1D population was 41.5 years, 50.5% of the participants were men, and 70% were non-Hispanic White. Out of these, 18,725 individuals were newly prescribed GLP-1RAs, and 7,210 individuals were newly prescribed SGLT2i.
Patients with T1D were identified using a validated EHR-based algorithm. Patient characteristics (demographics, laboratory investigation values, complications, comorbidities) of the overall T1D population in 2023 were compared with patients who were newly prescribed GLP-1RAs or SGLT2i.
Prescription trends for these medications from 2010 to 2023 were analyzed across T1D subgroups with obesity, cardiovascular disease, and chronic kidney disease, as well as by specific GLP-1RA products.
Data extraction and analysis were performed, and statistical analysis involved using chi-square and Student’s t-tests. Owing to the use of deidentified data, the study was exempted from review by Emory University’s Institutional Review Board.
Results and discussion
From 2010 to 2023, the prescribing of GLP-1RAs and SGLT2i for individuals with T1D was found to increase significantly from 0.7% to 8.3%. The profiles of patients newly prescribed these medications were notably different from the broader T1D population. Individuals on SGLT2i had higher rates of cardiovascular issues (e.g., heart failure: 16.6% vs. 2.8%) and kidney disease (26.9% vs. 15.9%), while those prescribed GLP-1RAs showed a higher prevalence of obesity (69.4% vs. 45.7%).
The most prominent growth in the GLP-1RA category came from prescribing semaglutide, which increased from 0.2% in 2018 to 4.4% in 2023, and tripeptide, approved in 2022, which reached 1.3% in its first year. SGLT2i use was found to increase particularly in T1D patients with cardiovascular disease, while GLP-1RAs were found to be more commonly used among those with obesity.
The findings highlight a growing off-label use of these drugs, possibly to manage additional health risks in T1D patients. While the study is strengthened by its use of large-scale data, the findings are limited by a lack of data on the reasons for prescribing these drugs, the potential bias from health system variations, potential misclassification of T1D patients, and limited generalizability beyond one EHR database.
Conclusion
In conclusion, the study suggests that the prescription of GLP-1RAs and SGLT2i in people with T1D increased from 2010 to 2023, particularly among those with higher cardiorenal risk profiles. Despite their benefits in weight management and cardiorenal health, these medications are not approved for T1D due to risks like euglycemic diabetic ketoacidosis and concerns about significant weight loss.
Further research is needed to evaluate the safety and efficacy of these treatments in the T1D population, so the researchers have advised physicians to exercise caution when prescribing GLP-1RAs and SGLT2i to patients with T1D.
Credit: news-medical.net
