Pharmacy Administration Software Program: Key Options & Integrations
This comprehensive approach to stock management empowers hospital pharmacies to streamline their processes and supply optimum affected person care. A barcode is placed when medicines are delivered to pharmacies and retail institutions. A pharma inventory management software program allows automatic drugs labeling and shows Which Sdlc Methodology Is True For You medication expiration dates. A pharmacist can use a file to document each drugs they store in an individual register.
Why Is Stock Management Essential In Pharmacies?
The world pharmacy inventory management software options and cupboards market measurement was valued at USD 6.10 billion in 2023 and is projected to grow at a CAGR of seven.9% from 2024 to 2030. The market development could be credited to the elevated adoption of automation options including dispensing cupboards with barcode and RFID technology. As the healthcare sector expands quickly, it faces an alarming rise in the quantity of prescriptions. Healthcare suppliers have more and more sought automated pharmacy inventory administration methods to scale back medicine errors.
Begin Your Journey Toward True Dscsa Compliance
We’ll explore the obtainable expertise stack potentialities beneath, however the two most important considerations when deciding on a technology are its scalability and growth prices. A distinctive Pharmacy inventory software program developed by our expert team to deal with the operation of pharmacy operation management, gross sales information, patient records and independent stores. Our software program generates common and on-demand stories, illustrating pharmacy KPIs with crisp graphics and enabling comprehensive business analysis with “what-if” measurement tools. We develop compounding administration platforms with Material Requirements Planning (MRP) modules for the optimized production of medication for specialty pharmacies. Pharmacy stock administration software program is vital for any modern-day pharmacy intending not just to remain competitive but to thrive in an ever-evolving business panorama.
- Systems like ScriptAbility plug in to PMSs and create accessible labels with massive print, Braille, Controlled Substance Safety and Dual Language labels.
- In this weblog, you will read the options to incorporate into the system and the method to manage pharmacy stock software.
- PioneerRx is a pharmacy administration software program famend for its complete suite of tools tailor-made to unbiased pharmacies.
- We implement cloud-based and on-premise pharmacy administration methods, guaranteeing their interoperability, scalability, and security.
Global Pharmacy Stock Management Software Program Options And Cabinets Market Report Segmentation
Act now to enable your pharmacy to succeed in its most potential by collaborating with CMARIX. Get in touch with us proper now to see how our experience and tailored technique might help your organization succeed. We build e-Prescribing systems that accelerate the filling, renewal, modification, and cancelation of medical scripts, in addition to the procurement of prior authorization. Read about Itransition’s 10+ years lengthy cooperation with a US-based multinational to create their flagship pharmaceutical information analytics merchandise. We always implement software with the most user-friendly UX/UI and supply sufficient consumer training to the pharmacy personnel in order to make their person expertise flawless.
The long-term care (LTC) phase is predicted to develop substantially during the forecast period. The growing geriatric population has increased the demand for specialized treatment administration, including LTC pharmacies. These pharmacies handle various drugs, including persistent disease remedies, ache administration, and palliative care.
A system with superior options like robotic integration, AI-powered forecasting, or patient-centric companies will value greater than a basic system with important capabilities like stock monitoring and order administration. With Datarithm®, the advantages you will see from our inventory administration solution will pay for themselves in less than three months. Serving USA, Canada, and Puerto Rico, Datarithm® software program serves impartial pharmacies together with single and multi-store operations in addition to regional chains, hospital outpatient pharmacies, and long-term care providers. So, regardless of the nature of measurement of your organization, Datarithm® will deliver our core benefits through our pharmacy inventory system and RX software program. We develop Point of Sale (POS) platforms with digital signature capture capabilities, inventory management APIs, and entry to Flexible Spending Account (FSA) and Health Savings/Reimbursement Account (HSA/HRA) networks. We integrate POS software with Customer Relationship Management (CRM), EHR/EMR, and external Practice Management System (PMS) modules for coordinating prescription histories inside your retail pharmacy.
Best of all, Datarithm® is cost-effective, So, take control of your pharmacy inventory as a substitute of letting it control you. Chetu’s pharmacy management expert builders design software that meet regulatory requirements set by the National Council for Prescription Drug Programs (NCPDP), United States Pharmacopeia (USP), the united states We develop accounts receivable platforms for managing insurer reimbursements, automating invoices, and processing payments.
Many providers provide training and assist that can assist you and your staff adapt to the new system. Over time, you may doubtless discover that the software program saves you time and reduces errors in comparison with handbook monitoring. Rx30 is a pharmacy administration software program that caters to a various client base, including unbiased pharmacies and pharmacy chains. Rx30 focuses on enhancing efficiency, enhancing patient care, and guaranteeing compliance with industry rules. Here, you specify the core functionalities of your pharmacy software, corresponding to prescription administration, inventory control, billing, affected person information, reporting, and integration needs with other healthcare systems.
This creates a place focused on top-notch pharmaceutical care and sensible resource use. Discover the highest finance app improvement companies recognized for creating secure and innovative financial solutions. Explore our listing to search out one of the best developers to convey your finance app thought to life. Online pharmacies dispensing managed substances must register with the DEA and comply with the Controlled Substances Act (CSA). For apps and software that sells drugs on-line, the Food and Drug Administration (FDA) is another essential regulation.
A pharmacy database management system is certainly one of its subdivisions, essential for keeping all medicine data in order, including names, licensing info, unique barcodes, registration, and expiration dates. PMS encompasses options to optimize medication ordering, deal with documentation, process payments, and streamline interactions between pharmacies, warehouses, sufferers or prospects, and healthcare institutions. Supply-side processes are additionally streamlined via extra efficient buying and cost mechanisms. Thus, permitting the pharmacy to maintain up with growing demand while sustaining sturdy business relationships.Ultimately, stock techniques guarantee a wholesome business so pharmacies can focus on maintaining their customers happy.
They dispense all kinds of medicines with important expiration dates and storage requirements, which must be managed efficiently. Inventory administration additionally helps cut back waste by making certain drugs are used before expiration and optimizing stock ranges to reduce prices. Additionally, pharmacy inventory administration software can be linked up with buyer relationship management (CRM) instruments.
Depending on the complexity of your PMS, your group requires information of virtual machines, managed databases, serverless computing, and international content material supply networks (CDNs). The price to hire builders from Western Europe and North America would price you greater than hiring developers from an EHR software growth firm. Although custom creation is normally more expensive, it provides total control and suppleness. For easy PIMS necessities, pre-built templates is often a cost-effective resolution, though their diploma of customization could additionally be limited. This is where you outline the efficiency, platform support, regulatory compliance, and different standards for your system that characterize its infrastructure.
It helps with inventory administration and improves workflows, making every day tasks simpler and keeping patients protected. The act is critical for healthcare software that offers with ePHI or involves sharing digital health info, by which pharmacy administration software is the case. It’s optional, nonetheless, for life-style apps or other healthcare software that doesn’t involve a high degree of personal knowledge sharing. Customer relationship management methods are the guts of every healthcare software.
NanoVation Therapeutics Announces Multi-Target Partnership with Novo Nordisk to Develop Genetic Medicines Targeting Cardiometabolic and Rare Diseases
Team Metabolic Health
NanoVation will receive research funding and is eligible to receive up to approximately US$600 million in up-front cash and potential milestone payments, as well as tiered royalties on future product sales as part of a multi-year deal
Partnership focuses on enabling nucleic acid delivery to cells outside of the liver
NanoVation Therapeutics, a platform company developing innovative technologies to overcome the barriers of nucleic acid delivery, today announced a multi-year partnership with Novo Nordisk to advance the development of novel genetic medicines targeting cardiometabolic and rare diseases. The partnership combines NanoVation Therapeutics’ proprietary long-circulating lipid nanoparticle (lcLNP™) technology for RNA delivery to cells outside of the liver with Novo Nordisk’s expertise in cardiometabolic and rare disease R&D and clinical translation.
“We founded NanoVation to enable partners to overcome the challenges of conventional nucleic acid delivery systems”
Under the terms of the agreement, Novo Nordisk and NanoVation will collaborate on two lead programs to develop base-editing therapies for certain rare genetic diseases, and up to five additional future targets for cardiometabolic and rare diseases. Novo Nordisk will receive a defined exclusive, worldwide license to use NanoVation’s LNP technology for the two lead programs. NanoVation will receive research funding and is eligible to receive up to approximately US$600 million in up-front cash and potential milestone payments, as well as tiered royalties on future product sales as part of the multi-year deal.
“We founded NanoVation to enable partners to overcome the challenges of conventional nucleic acid delivery systems,” said Dominik Witzigmann, PhD, co-founder and CEO of NanoVation Therapeutics. “This agreement with Novo Nordisk and ongoing work with companies in the cell and gene therapy space is validation of the potential of our LNP technologies to enable the next generation of life-changing genetic medicines. We are very excited to collaborate with the team at Novo Nordisk.”
“Every genetic drug has a cargo and delivery component, which require dedicated innovation on both,” said Karina Thorn, PhD, Corporate Vice President, Head of Research, Global Nucleic Acid Therapies at Novo Nordisk. “We look forward to partnering with NanoVation, as the company’s differentiated delivery platform could help Novo Nordisk to advance genetic medicine candidates with curative potential.”
NanoVation was co-founded by Pieter Cullis, PhD, current Board Chair, who is widely regarded as the founding father of LNP technology. “Genetic medicine is at a pivotal moment and this partnership marks a major milestone for NanoVation as an innovator in nucleic acid delivery,” said Cullis. “By combining NanoVation’s expertise in extrahepatic delivery with Novo Nordisk’s expertise in cardiometabolic and rare diseases we have the potential to create truly transformative therapies.”
NanoVation has an extensive and continuously growing library of novel lipids and LNP compositions. The company works in partnership with industry leaders from concept to lead development to create fit-for-purpose solutions for nucleic acid delivery. NanoVation’s lcLNP technology has demonstrated the ability to deliver nucleic acids to various cell types beyond the liver in preclinical studies, with improved potency, safety and stability compared to conventional systems. The company’s toolbox provides a “one-stop-shop” IP portfolio for LNP-based genetic medicine development, offering comprehensive solutions spanning novel lipid design, RNA modification and LNP formulation.
Credit: Businesswire
Semaglutide vs. liraglutide: One-year weight loss efficacy in obesity and type 2 diabetes
Team Metabolic Health
New study reveals semaglutide outperforms liraglutide in weight loss for obesity, highlighting key factors that contribute to significant weight reduction in patients.
A recent JAMA Network Open study compares the weight loss efficacy of injectable liraglutide and semaglutide, in addition to identifying the factors associated with a weight reduction of 10% or more after one year of treatment.
Treating obesity
Obesity leads to or worsens the risk of various health disorders, some of which include cardiovascular disease, cancer, type 2 diabetes (T2D), osteoarthritis, and obstructive sleep apnea. Over the past two decades, the United States Food and Drug Administration (FDA) has approved two glucagon-like peptide-1 receptor agonists (GLP-1 RAs) for treating obesity, of which include liraglutide and semaglutide.
In randomized clinical trials, liraglutide and semaglutide have led to significant weight reductions. However, outside of clinical trials, weight loss data with liraglutide or semaglutide has been limited to a short follow-up period of six months.

Study: One-Year Weight Reduction With Semaglutide or Liraglutide in Clinical Practice. Image Credit: Pixel-Shot/Shutterstock.com
About the study
In the present study, weight outcomes among obese patients who received injectable forms of semaglutide or liraglutide at one year were assessed between January 1, 2015, and July 28, 2023. Outcomes were compared by GLP-1 RA agent, dosage, indication, and persistent coverage with the medication.
The main exposure variable was injectable forms of liraglutide or semaglutide approved for T2D or obesity. Comparatively, main outcome measures were categorical weight reduction of 10% or greater and percentage weight change at one year.
Adult patients with a body mass index (BMI) of at least 30 kg/m2 who completed a follow-up weight measurement at least 12 months after treatment initiation were included in the study. Patients prescribed these medications between January 1 and June 30, 2015, were excluded. Furthermore, patients with cancer diagnoses, were pregnant, and those who recently underwent bariatric surgery were excluded.
Study findings
A total of 1,718 and 1,671 patients filled an initial prescription for injectable semaglutide and liraglutide, respectively. The median BMI was 38.5 kg/m2 and the average age of the study participants was 50 years.
Approximately 55% of patients were female and about 82% reported T2D as a treatment indication. Moreover, 20.3% of the study participants were Black, 7% were Hispanic, 68.5% were White, and 3.4% belonged to other races or ethnicities. Most patients were privately insured and about 28% lived in the most disadvantaged area by quartile of the area deprivation index (ADI).
At one-year, the average weight change was -3.7% in the study cohort. The average changes with semaglutide and liraglutide were -5.1% and -2.2%, respectively.
In patients receiving T2D medication, the mean change was -3.2% as compared to -5.9% of those who were being treated for obesity. Among patients with fewer than 90 medication coverage days, between 90 to 275 medication coverage days, and coverage at one year, weight changes were -1.8%, -2.8%, and -5.5%, respectively. Patients prescribed high doses exhibited an average weight change of -6.6% as compared to -3.5% for those on a low-maintenance dose.
The reduction in body weight was -12.9% for semaglutide for obesity patients with persistent coverage with their medication at one year. For the same coverage, the reduction in body weight was -5.9% with semaglutide for T2D, -3.1% with liraglutide for T2D, and -5.6% with liraglutide for obesity.
About 37% of individuals prescribed semaglutide for obesity achieved 10% or more body weight reduction as compared to 16.6% of those prescribed semaglutide for T2D, 14.5% of those prescribed liraglutide for obesity, and 9.3% of those receiving liraglutide for T2D.
Among patients receiving persistent medication at one year, 61% of patients prescribed semaglutide for obesity achieved at least 10% weight reduction as compared to 23.1% among those prescribed semaglutide for T2D, 28.6% liraglutide for obesity, and 12.3% liraglutide for T2D groups.
Achieving 10% or greater weight reduction at one year was associated with several factors such as semaglutide or liraglutide, obesity as a treatment indication as compared to T2D, female sex, persistent coverage for one year, and high or low dosage of medication.
The likelihood of achieving 10% or more weight loss at one year was 2% higher for every unit increase in baseline BMI. When medication switchers were excluded, the multivariable model results remained robust.
Conclusions
Weight reduction one year after treatment initiation was associated with the medication’s active agent, patient sex, dosage, medication coverage, and treatment indication. Importantly, additional research is needed to better understand the reasons for discontinuing treatment and interventions to enhance long-term persistent coverage.
Credit: news-medical.net
In Every U.S. State, at Least 1 in 5 People Is Now Obese
Team Metabolic Health
Key Takeaways
- U.S. obesity rates keep rising, with 1 in every 5 people in every state reported to be obese in 2023
- In 23 states, 35% or more of the population is now obese
- Tackling unhealthy weight gain as early as childhood may be key to turning these numbers around

Pix Credit: Adobe Stock
Statistics from 2023 on U.S. obesity rates bring no good news: In every state in the nation, 1 in every 5 people is now obese, the new tally shows.
In 2013, not one state had an adult obesity rate topping 35%, but 10 years later 23 states had achieved that dubious distinction, according to data released Thursday by the U.S. Centers for Disease Control and Prevention.
Obesity is defined by the CDC as a BMI of 30 or higher. A person measuring 5 feet 11 inches and weighing 215 pounds has a BMI of 30; so does a person measuring 5 feet 6 inches with a weight of 186 pounds.
Millions more Americans struggling with their weight is really bad news, the CDC said in a statement.
“Obesity is a disease that can cause many health conditions such as asthma, heart disease, stroke, type 2 diabetes, some cancers and severe outcomes from respiratory illnesses,” the agency said. “In addition, the stigma and bias about a person’s weight can cause social and mental health consequences, such as anxiety and poor body image.”
Those 23 states where obesity has now affected at least 35% of the populace include: Alabama, Alaska, Arkansas, Delaware, Georgia, Illinois, Indiana, Iowa, Kansas, Louisiana, Michigan, Mississippi, Missouri, Nebraska, New Mexico, North Dakota, Ohio, Oklahoma, South Carolina, South Dakota, Tennessee, West Virginia and Wisconsin.
Race seemed to matter: In 38 states, 35% or more of Black adult residents struggled with obesity. That was true for Hispanic adults in 34 states, American Indians/Alaska Natives in 30 states and whites in 16 states.
Only Asian Americans did not have an obesity prevalence at or above 35% in any state, the new report found.
Overall, the new statistics “highlight the need for obesity prevention and treatment options, which start with building healthier communities where people of all ages have safe places for physical activity, and where health care and healthy food options are accessible and affordable for all,” said Dr. Karen Hacker. She directs the CDC’s National Center for Chronic Disease Prevention and Health Promotion.
Turning the 2023 numbers around will mean starting where weight gain often begins — in childhood.
“Obesity prevention at young ages is critical, because we know that children with obesity often become adults with obesity,” Hacker said in the CDC statement.
Shaming folks for their weight is definitely not the right approach, and it’s not even valid, according to Dr. Ruth Petersen, director of CDC’s Division of Nutrition, Physical Activity and Obesity.
“Obesity is a complex disease,” she explained. “There’s a common misconception that obesity is a result of lack of willpower and individual failings to eat well and exercise.”
However, “many factors contribute to obesity like genes, certain medications, poor sleep, gut microbiome, stress, access to affordable food, safe places to be active and access to health care,” Petersen said. “Understanding these factors helps us identify potential prevention and treatment strategies.”
Credit: healthday.com
US FDA approves Zevra’s treatment for rare genetic disease
Team Metabolic Health
The U.S. Food and Drug Administration has approved Zevra Therapeutics’ drug for a rare and fatal genetic disorder, making it the first treatment to get a nod for the condition, the health regulator said on Friday.
The company has been trying for years to bring the drug to market after the FDA previously declined to approve it and extended a review of the treatment.
The oral drug, branded as Miplyffa, has now been approved for the treatment of Neimann-Pick disease type C – a rare genetic condition that affects the nervous system and other organs.

On average, people affected by this disease only live for about 13 years.
“The first-ever approval of a safe and effective drug option for NPC will undoubtedly support the essential medical needs of those suffering,” said Janet Maynard, a director at the FDA’s Center for Drug Evaluation and Research.
Miplyffa, in combination with miglustat, which is branded as Zavesca, has been cleared to treat neurological symptoms associated with NPC in adults and children 2 years of age and older.
The drug is expected to be available in the U.S. in eight to 12 weeks, Zevra said.
The company did not immediately respond to a Reuters request for comment on pricing.
H.C. Wainwright analyst Oren Livnat expects the average net price of the drug to between $500,000 and $600,000 per year.
Livnat estimates peak sales of about $250 million in the U.S.
Miplyffa comes with a warning for hypersensitivity reactions including hives and angioedema, a condition that causes swelling under the skin.
Zevra gained access to the drug through its acquisition of Orphazyme, the original developer, in 2022.
Shares of the company rose more than 5% to $8.43 in afternoon trading.
Credit: Reuters
Study finds two common surgeries equally effective for treating blinding condition of the eyelid
Team Metabolic Health
Trachomatous trichiasis, a potentially blinding condition where inward-turned eyelashes scratch the front of the eye, can successfully be treated by either of the two most common types of eyelid surgery, according to findings from a large comparison trial. In light of previous, smaller studies, which suggested that one of the commonly used surgery types had poorer outcomes, this study provides reassurance that either technique can treat the condition.
The study, “The impact of modified incision height and surgical procedure on trichiasis surgery outcomes: Results of the Maximizing Trichiasis Surgery Success (MTSS) Randomized Trial,” is published in PLOS Neglected Tropical Diseases.
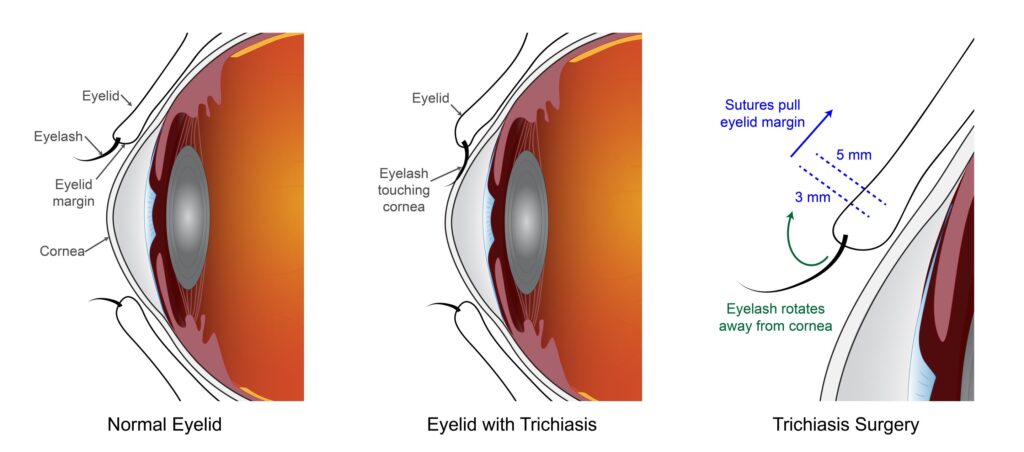
On a normal eyelid (left), eyelashes are turned outward away from the cornea. Eyelids affected by trichiasis (center) have eyelashes touching the eye. Surgery for eyelids affected by trichiasis (right), rotates the eyelash away from the cornea, returning them to their normal anatomic position. Surgical incisions were placed at either 3mm or 5mm away from the eyelid margin. Credit: National Eye Institute
“Some studies have reported post-operative trichiasis rates of 30% or higher for patients with trachomatous trichiasis following surgery, and repeat surgeries are more difficult,” said Emily Gower, Ph.D., University of North Carolina at Chapel Hill.
“This trial sought to determine if we could decrease the risk of post-operative trichiasis by modifying the surgical procedure. We found that existing approaches result in better outcomes.”
Trachomatous trichiasis affects approximately 1.7 million people worldwide, mostly in poor and rural areas of Africa. The condition arises after repeated or chronic eye infections with the bacteria Chlamydia trachomatis, which is spread by person-to-person contact.
Trachoma is very common in hot, dry areas of the world, and repeat infections can eventually lead to scarring and malformation of the eyelid. This malformation causes the edge of the eyelid to draw inward, so that eyelashes scratch the eye. If left untreated, trichiasis can result in corneal clouding, and eventually blindness.
The most common and effective treatment for trichiasis is surgery to correct the in-turning of the eyelid, which typically is performed in one of two different ways. A few smaller studies indicated that one of the surgery methods, posterior lamellar tarsal rotation (PLTR), might be more effective, so some programs in Africa began retraining surgeons to perform that method.
Additionally, previous analysis of eyelids treated with the other surgery, bilamellar tarsal rotation (BLTR), suggested that placing the surgical incision slightly further from the edge of the eyelid (5 millimeters above the lid margin instead of 3mm) might lead to fewer recurrences, but this change had not previously been tested.
The current study directly compared these three surgery approaches and evaluated the risk of post-operative trichiasis.
The study, which took place in southern Ethiopia, enrolled 4,914 patients with trichiasis in one or both eyes (6,940 eligible eyes). The participants were randomized to receive BLTR at 3mm incision height, BLTR at 5mm incision height, or PLTR. Researchers rechecked the patients for post-operative trichiasis at six weeks and again at 12–18 months. On average, approximately 17% of eyelids had post-operative trichiasis.
There was no difference in risk of post-operative trichiasis between the two methods with a 3mm incision height, while those who received the 5mm incision height BLTR were significantly more likely to have post-operative trichiasis. The results indicate that the current standard surgeries—either method at 3mm—are better options for trichiasis treatment than the 5mm method.
Credit: medicalexpress.com
GLP-1s Can Prevent Cirrhosis in People with Fatty Liver Disease
Team Metabolic Health
Researchers found that people with diabetes and metabolic dysfunction-associated steatotic liver disease taking glucagon-like peptide 1 receptor agonists (GLP-1RAs) like Ozempic had a slightly lower risk of developing liver complications.
Metabolic dysfunction-associated steatotic liver disease (MASLD), previously known as non-alcoholic fatty liver disease (NAFLD), impacts over 100 million people in the United States. The condition occurs when excess fat builds up in the liver, leading to liver inflammation.
People at higher risk for MASLD include those with obesity, high cholesterol, type 2 diabetes, and other conditions associated with metabolic syndrome.
Image by Alones via Shutterstock
Moreover, about 25% of people with MASLD develop liver damage, known as non-alcoholic steatohepatitis (NASH). Of those, 11% experience liver cirrhosis or liver failure. Each year in the U.S., around 26,000 deaths are attributed to cirrhosis. That’s why preventing the progression from non-alcoholic fatty liver disease to cirrhosis is critical.
Since there are no specific medications to treat MASLD, healthcare providers typically recommend diet and lifestyle changes to prevent further liver damage. In some cases, MASLD can be reversed if caught in the early stages.
Recently, researchers discovered that a trendy class of diabetes/weight loss medications called glucagon-like peptide 1 receptor agonists (GLP-1RAs), such as Ozempic and Wegovy, may be effective at lowering the risk of cirrhosis in people with MASLD.
The findings show that GLP-1s may be a new prevention strategy for cirrhosis that could help reduce mortality risks from this challenging condition.
Liver benefits from taking GLP-1s versus other diabetes drugs
The study, published on September 16 in JAMA Internal Medicine, used data from the National Veterans Health Administration Corporate Data Warehouse and Central Cancer Registry to compare liver outcomes of people with MASLD and type 2 diabetes.
Specifically, they looked at who took GLP-1RAs (exenatide, dulaglutide, liraglutide, or semaglutide) or dipeptidyl peptidase 4 inhibitors (DPP-4is), including sitagliptin, saxagliptin, linagliptin, or alogliptin, to see how these medications impacted liver health.
The scientists found that participants without cirrhosis who used GLP-1RAs had a slightly lower risk of developing cirrhosis compared to those using DPP-4is.
Moreover, people in the GLP-1 group had a lower risk of cirrhosis complications, liver cancer, and mortality compared to the DPP-4i group, but the difference in complications was not statistically significant.
In addition, the researchers found no differences in outcomes among participants taking GLP-1s or DPP-4is who already had cirrhosis.
Though the study results require confirmation in clinical trials, the team suggests that since both drugs offered no benefit to people who already had cirrhosis, treating MASLD early with GLP-1s may be critical for preventing this condition.
“While cirrhosis is a clear risk factor for [liver cancer] and reducing cirrhosis by GLP-1 RA use should prevent [liver cancer], an independent confirmation of this relationship requires even larger studies than this one,” the study’s authors wrote. “In the meantime, the presence of MASLD can help with the prioritization of GLP-1 therapy in persons with diabetes.”
Credit: healthnews.com
Microbial-immune interactions in severe asthma: Insights into pathogen dominance and treatment approaches
Team Metabolic Health
Study identifies treatable microbiome features in severe asthma, revealing potential for precision antibiotic therapies.
A recent study published in Allergy assesses the airway microbiome and host immune-inflammatory responses to identify treatable aspects of severe asthma.
Asthma and the airway microbiome
Asthma is characterized by reversible airway constriction. In severe asthma, it is important to identify treatable features that distinguish subsets of this condition. For example, in the type-2 high subset, both sputum and blood eosinophils are high, with most patients responding well to corticosteroids and anti-interleukin 5 (IL-5) agents.

Study: Species-level, metagenomic and proteomic analysis of microbe-immune interactions in severe asthma. Image Credit: Olga Rolenko/Shutterstock.com
Conversely, the type-2 low subtype, which affects 30-50% of individuals with severe asthma, is associated with a poor response to approved biologics or systemic corticosteroids. The type-2 low subtype includes both neutrophilic and paucigranulocytic asthma, the latter of which is also referred to as non-neutrophilic or eosinophilic asthma.
The lack of response to treatments in the type-2 low subtype may be due to bacterial infection and/or neutrophilic infiltration of the airways due to immunologic responses. This may also explain the observed efficacy of long-term macrolide antibiotics like azithromycin in this subset of patients.
Previous studies have identified Hemophilus and Moraxella as the most common microorganisms present in the airway microbiome, particularly the lower airway. Low commensal abundance, neutrophilic inflammation, and adverse outcomes often accompany H. influenzae infection.
About the study
The researchers of the current study were interested in determining whether the dominance of microorganisms in the airway microbiome could function as a treatable trait in severe asthma. They hypothesized that this shift would only be observed the lower airway and, as a result, contribute to treatment-refractory neutrophilic inflammation caused by type-1 cytokine release.
Sputum and nasal lavage samples were obtained from patients with severe asthma from the Oxford and Wessex cohorts. DNA extracted from these samples was examined by long read metagenomic sequencing, following which species-level genetic data was integrated with clinical and airway proteomics parameters.
Different immune responses
Participants in both cohorts had similar demographic, lung function, and inhaled corticosteroid use data. Oral corticosteroids were more common in the Wessex cohort, as these individuals were recruited before biologics were frequently used.
Neutrophilic asthma was identified in 25.5% of patients with severe asthma, whereas 39% had paucigranulocytic asthma. Current smokers comprised 33% of the study cohort, with less than ten mean pack years smoked.
Only severe asthma patients were included in the Oxford cohort. A high baseline blood eosinophil count was observed in these individuals, with eosinophilic sputum reported in 36.7%.
In both cohorts, disease control was often poor in patients with severe asthma.
Differing microbial profile in severe asthma
In the Wessex cohort, the sputum microbiome was similar between healthy individuals and those with mild asthma. However, among 81 patients with severe asthma, over 23% of the microbiomes exhibited dominance of one respiratory pathogen during clinical stability.
H. influenzae, M. catarrhalis , S. pneumoniae, and P. aeruginosa were the dominant species in ten, four, four, and one sample, respectively. Single-pathogen dominance by H. influenzae, M. catarrhalis, S. pneumoniae, and T. whipplei is associated with neutrophilic asthma, along with Firmicutes depletion, a known marker for poor outcomes.
Eosinophilic asthma patients were more likely to exhibit higher M. catarrhalis, S. intermedius and V. parvula abundance with lower abundance of H. influenzae and S. pneumoniae. Paucigranulocytic asthma was associated with lower abundances of M. catarrhalis, H. influenzae, and T. whipplei.
Neutrophilic asthma was associated with higher levels of type 1 cytokines and proteases. H. influenzae dominance predicted higher eosinophil cationic protein, elastase, and IL-10 levels, thus suggesting disruption of normal immunologic response, pathogen persistence, and airway remodeling.
Rothia mucilaginosa is a facultative anerobe that can thrive at lower oxygen levels in mucus-plugged airways. Increased abundance of this microorganism was observed in microbiomes without single-pathogen dominance.
Rothia mucilaginosa abundance was also associated with IL-6 levels and inversely correlated with fibroblast growth factor (FGF) levels. FGFs drive airway remodeling through smooth muscle and vascular hyperplasia, which is reduced by antibiotic treatment.
Using Bayesian analysis, H. influenzae and M. catarrhalis were independently but strongly associated with type-1 airway inflammation.
Not ‘one airway, one disease’
The upper airway microbiome and cytokine profile differed significantly from that of the lower airway.
Assuming that nasal lavage and sputum samples represent these two locations, respectively, the upper airway is enriched for S. epidermidis and S. aureus, whereas the lower airway is enriched for Firmicutes, mostly Streptococcus species. Nasal lavage specimens exhibited higher abundance of D. pigrum, M. catarrhalis and E. coli as compared to H. influenzae and H. parainfluenzae.
Azithromycin is effective for the treatment of both neutrophilic and non-neutrophilic phenotypes of severe asthma, which may be attributed to the dominance of H. influenzae, M. catarrhalis, and S. pneumoniae. However, targeted therapy after confirming this trait is important considering widespread resistance to this antibiotic.
Conclusions
The current study is the first to examine airway microbiome profiles at the species level in a large sample of individuals with severe asthma. Single-pathogen dominance was observed in 20-30% of these patients, the most common of which was H. influenzae, along with neutrophilic infiltration and type-1 inflammation.
The ‘one airway, one disease’ concept does not apply to the airway microbiome in severe asthma.”
The study findings also demonstrate the feasibility of Nanopore sequencing to identify pathogen dominance in ordinary medical practice. Future applications of this technology could guide the precise antibiotic management of patients with severe asthma and other airway diseases.
Credit: news-medical.net
Pfizer says its experimental drug for deadly condition that causes appetite and weight loss in cancer patients shows positive trial results
Team Metabolic Health
Key Points
- Pfizer said its experimental drug for a common, life-threatening condition that causes cancer patients to lose their appetite and weight showed positive results in a midstage trial.
- Patients with the condition, called cancer cachexia, who took Pfizer’s treatment saw improvements in body weight, muscle mass, quality of life and physical function.
- The results could pave the way for the drug, a monoclonal antibody called ponsegromab, to become the first treatment approved specifically for cancer cachexia.

Kena Betancur | Corbis News | Getty Images
Pfizer’s experimental drug for a common, life-threatening condition that causes cancer patients to lose their appetite and weight showed positive results in a midstage trial, the drugmaker said Saturday.
Patients with the condition, called cancer cachexia, who took Pfizer’s treatment saw improvements in body weight, muscle mass, quality of life and physical function, according to the drugmaker. The results could pave the way for the drug, a monoclonal antibody called ponsegromab, to become the first treatment approved in the U.S. specifically for cancer cachexia.
The condition affects about 9 million people worldwide, and 80% of cancer patients suffering from it are expected to die within one year of diagnosis, according to the company.
Patients with cancer cachexia don’t eat enough food to meet their body’s energy needs, causing significant fat and muscle loss and leaving them weak, fatigued and, in some cases, unable to perform daily activities. Cancer cachexia is currently defined as a loss of 5% or more body weight over the past six months in cancer patients, along with symptoms such as fatigue, according to the National Cancer Institute.
The symptoms of the condition can make cancer treatments less effective and contribute to lower survival rates, Pfizer said.
“We would see ponsegromab fitting into the treatment of cancer patients, really addressing that unmet need in cachexia, and through that, improving their wellness, their ability to care for themselves, and we would also hope their ability to tolerate more treatment,” Charlotte Allerton, Pfizer’s head of discovery and early development, told CNBC in an interview.
Pfizer has not disclosed the estimated revenue opportunity of the drug, which could potentially be approved for different uses.
The company presented the data Saturday at the European Society for Medical Oncology 2024 Congress, a cancer research conference held in Barcelona, Spain. The results were also published in The New England Journal of Medicine.
The phase two trial followed 187 people with non-small cell lung cancer, pancreatic cancer or colorectal cancer and high levels of a key driver of cachexia called growth differentiation factor 15, or GDF-15. It is a protein that binds to a certain receptor in the brain and has an impact on appetite, according to Allerton.
After 12 weeks, patients who took the highest dose of ponsegromab — 400 milligrams — saw a 5.6% increase in weight compared with those who received a placebo. Patients who took a 200-milligram or 100-milligram dose of the drug saw a roughly 3.5% and 2% increase in body weight, respectively, compared with the placebo group.
Allerton said a work group of experts defines a weight gain of greater than 5% as a “clinically meaningful difference in cancer patients with cachexia.” She added that the drug’s effect on other measures of wellness, such as increased appetite and physical activity, is “really what offers us the encouragement.”
Pfizer said it did not observe any significant side effects with the drug. Treatment-related side effects occurred in 8.9% of people taking a placebo and 7.7% of those who took Pfizer’s treatment, the company said.
The company said it is discussing late-stage development plans for the drug with regulators, and aims to start studies in 2025 that can be used to file for approval. Pfizer is also studying ponsegromab in a phase two trial in patients with heart failure, who can also suffer from cachexia.
Pfizer’s drug works by reducing the levels of GDF-15. Pfizer believes this can improve appetite and enable patients to maintain and gain weight.
“For most of us, we have low levels of GDF-15 in our tissues when we’re healthy, but we really do see this up regulation of GDF-15 in more of these chronic conditions, and in this case, cancer,” Allerton said.
Credit: CNBC
Is Ozempic Becoming The New Botox? Hollywood’s Latest Quick Fix Medication Taking Over The Industry
Team Metabolic Health
As a celebrity, always looking your best is essential. Whether this is achieved naturally through the help of a trainer or intense diets, staying in shape is a part of their high-profile careers. But, in recent times, there has been a shift in these regimes. In addition to hiring the most sought-after fitness gurus or tapping into beauty treatments, the latest trend that has circulated amongst the rich and famous is Ozempic.
Is Ozempic Becoming The New Botox? Hollywood’s Latest Quick Fix Medication Taking Over The Industry
Initially created to treat symptoms of type 2 diabetes and regulate blood sugar levels, this drug is now known to tackle weight loss quickly. Decades ago, Botox took first place as the “miracle treatment” in Hollywood. With just a few injections, the medication can smooth out wrinkles and prevent the side effects of aging. As a result, many people appeared flawless and younger. However, Ozempic might be taking its place as a quick-fix treatment but with a different goal. Of course, this doesn’t seem to bother celebrities now calling this drug the best-kept weight loss secret.
Remember when Botox was an easy fix and the industry’s biggest secret? The craze continued for quite a while, as no one seemed to be aging anymore, but they also didn’t reveal how they were achieving the look. This same secretive culture is slowly forming around Ozempic, with some celebs turning to the injectable for rapid weight loss. However, only a few are willing to open up about their usage, such as Tracy Morgan and Macy Gray.
Even though these medications are typically used as a shortcut, there are still risks that come along with using them. Despite Botox being safe in controlled doses, Ozempic isn’t a cosmetic treatment. As previously stated, the medication’s primary use is to manage diabetes, and using it without a proper prescription can lead to serious health complications, including nausea, vomiting, and diarrhea. Last year, Ozempic manufacturers were sued for such side effects. Additionally, since Ozempic has become such a popular drug, the increasing demand is reportedly leading to shortages for individuals who need the medication.
Nonetheless, there’s no denying the appeal of these fast-acting medications, especially in industries where appearance means everything. But, as the excitement surrounding Ozempic continues to grow, there’s also an increase in conversations about the importance of using prescriptions safely. To avoid long-term complications, it is best to consult with a health professional before using.
Credit: balleralert.com
Are you at risk for stroke: Learn warning signs, causes and path to effective rehabilitation
Team Metabolic Health
The alarming link between hypertension, diabetes and stroke you can’t afford to ignore!
A stroke occurs when blood flow to the brain is suddenly interrupted, either by a blocked blood vessel or a ruptured artery, leading to the death of brain cells due to oxygen deprivation. This neurological disorder can have profound consequences, including hemiplegia, difficulty speaking, depression and dementia.
Are you at risk for stroke: Learn warning signs, causes and path to effective rehabilitation (Photo by American Speech-Language-Hearing Association)
In an interview with HT Lifestyle, Dr Mahendra JV, HOD and Consultant – Department of Neurology at Ramaiah Institute of Neurosciences in Ramaiah Memorial Hospital, shared, “The risk of stroke increases significantly with age, particularly after 55, and is exacerbated by conditions such as high blood pressure, uncontrolled diabetes, coronary artery disease and high cholesterol.”
He revealed, “While we cannot alter factors like age and genetics, managing conditions like hypertension and diabetes, along with adopting a healthier lifestyle can significantly reduce the risk of stroke. Rehabilitation plays a critical role in recovery, with approaches like constraint-induced movement therapy, robotics, and fitness training showing promise in restoring motor functions.”
He highlighted, “Occupational therapy is vital for helping survivors regain the ability to perform daily tasks. Ongoing research into innovative therapies, including virtual reality, and drug augmentation, holds the potential to further enhance recovery outcomes. Understanding the causes and symptoms of stroke, as well as the importance of timely rehabilitation is the key to improving patient outcomes and reducing the global impact of this debilitating condition.”
Dr Khushbu Goel, Head and Consultant – Stroke Care Programme and Management and Neurology at Manipal Hospital in New Delhi’s Dwarka, echoed, “Stoke is a brain attack caused by a disruption in the blood supply, which prevents brain tissues from receiving enough oxygen and nutrients.”
There are major 2 types of stroke- Ischemic and hemorrhagic stroke –
- An ischemic stroke occurs when the blood supply to part of the brain is blocked or reduced. This prevents brain tissue from getting oxygen and nutrients.
- Another type of stroke is a hemorrhagic stroke. It occurs when a blood vessel in the brain leaks or bursts and causes bleeding in the brain
- Medical risk factors
- High blood pressure
- Cigarette smoking
- High cholesterol
- Diabetes
- Obstructive sleep apnea
- Cardiovascular disease, including heart failure, heart defects, heart infection or irregular heart rhythm, such as atrial fibrillation
- Personal or family history of stroke, heart attack or transient ischemic attack
Other factors associated with a higher risk of stroke include:
Age- People age 55 or older have a higher risk of stroke than younger people.
Sex- Men have a higher risk of stroke than women. Women are usually older when they have strokes, and they’re more likely to die of strokes than men.
Lifestyle risk factors:
- Being overweight or obese.
- Physical inactivity.
- Heavy or binge drinking.
- Use of illegal drugs such as cocaine and methamphetamine.
Symptoms of stroke are:
- Trouble speaking and understanding what others are saying. A person having a stroke may be confused, slur words, or may not be able to understand speech.
- Numbness, weakness, or paralysis in the face, arm or leg. This often affects just one side of the body. The person can try to raise both arms over the head. If one arm begins to fall, it may be a sign of a stroke. Also, one side of the mouth may droop when trying to smile.
- Problems seeing in one or both eyes. The person may suddenly have blurred or blackened vision in one or both eyes. Or the person may see double.
- Sudden onset imbalance can also be a symptom of stroke
What is stroke rehabilitation?
Stroke rehabilitation is a comprehensive program designed to help individuals recover and regain independence following a stroke. It involves a multidisciplinary approach, including physical, occupational, and speech therapies, aimed at restoring function and improving quality of life. Rehabilitation focuses on strengthening muscles, improving coordination and enhancing mobility through exercises and activities tailored to the patient’s specific needs. It also addresses cognitive and emotional challenges, helping patients relearn skills such as speaking, swallowing and daily activities.
Speech therapy focuses on helping patients who have difficulties with speaking or understanding language, addressing challenges in communication that may arise after a stroke. Physical therapy is centered on exercises designed to help patients regain movement and coordination skills that may have been affected by the stroke, promoting strength, balance and mobility.
Credit: Hindustan Times
Can Drinking Alcohol Prevent Food Poisoning?
Team Metabolic Health
Claims on social media suggest it can. We asked experts for the sober truth.
“Cheers,” a woman says in a video on TikTok as she raises a shot glass filled with liquor to the camera. She tips it back, grimaces and then sticks out her tongue in disgust.
“It’s medicinal, it’s medicinal,” she reminds herself.
The reason for the shot was a recent meal, which she worried may have given her food poisoning, she said. And she had read in a study that because “alcohol is a sterilizer,” it can protect against food-borne illness.

Pix Credit: Derek Brahney
But can it really?
There may be an ounce of truth to the notion that drinking alcohol around the time you eat contaminated food can reduce the chances of food poisoning, experts said. But the evidence to support the claim is limited. And depending on how much you drink, alcohol could hurt your immune system more than it might help. Here’s what we know.
What the Research Suggests
Several small studies on food-borne illness outbreaks have indeed found that consuming alcohol was associated with protection from food poisoning, but they all have limitations.
In the study cited in the TikTok video, which was published in 2002, researchers described a salmonella outbreak that began at a 120-person banquet in Spain. At least 47 people became ill with vomiting or diarrhea, along with stomach cramps, fever or headache, after consuming contaminated tuna sandwiches and potato salad. The researchers found that those who reported having three or more drinks at the celebration were 46 percent less likely to become ill than those who didn’t drink; and those who had up to three drinks were 27 percent less likely to develop symptoms.
Likewise, in a 1992 study of a 61-person outbreak of hepatitis A from raw oysters in Florida, researchers found that those who reported drinking wine, whiskey or cocktails with the oysters were 90 percent less likely to get sick than those who did not drink. Those who consumed beer, however, did not seem to be protected — the researchers hypothesized this was perhaps because beer has a lower alcohol concentration than the other beverages.
These studies support the theory that alcohol might interrupt the pathogens in people’s guts before they can cause illness, said Donald Schaffner, a professor of food science at Rutgers University. This is plausible, he said, since alcohol can kill bacteria and inactivate some viruses; that’s why it’s used in hand sanitizers and surface disinfectants.
But these small, decades-old studies can only show correlations between drinking and fewer illnesses; they can’t prove that alcohol prevented food poisoning, said Matthew Moore, an associate professor of food science at the University of Massachusetts Amherst.
He recommended taking those findings “with a serious grain of salt.”
It’s possible, for example, that some of the people who didn’t drink in those studies were abstaining for health reasons, which could have explained why they were more susceptible to food poisoning.
Researchers have not directly tested how drinking might influence food poisoning risk in a clinical trial, which could control for differences between people who do and don’t drink, Dr. Moore said. And in at least one outbreak of 33 people sickened with hepatitis E from shellfish on a cruise, researchers came to a different conclusion: Only those who drank alcohol were infected while the abstainers remained healthy.
Alcohol Might Weaken Your Immune System
Your chance of getting sick from contaminated food can depend on various factors, including your health, the amount of pathogen present, the type of food and how much of it you ate, said Craig Hedberg, an epidemiologist and food safety expert at the University of Minnesota. How alcohol plays into that is not well researched in humans, he said. But in a 2001 study, scientists found that although red and white wine killed salmonella in petri dishes, feeding it to mice did nothing to protect them when they consumed the bacteria.
If you drink too much, it’s also possible that alcohol might make your intestine more susceptible to infections, said Dr. Gyongyi Szabo, a gastroenterologist and professor of medicine at Harvard Medical School.
Research from Dr. Szabo and her colleagues has suggested that binge drinking — defined as four to five or more drinks in about two hours for most adults — can cause inflammation and signs of “leakiness” in the gut lining, which can allow bacteria and toxins to more easily enter the blood.
It’s also clear that heavy, chronic drinking can reduce your immune system’s ability to fight infections, she said. Research has shown, for example, that people with alcohol use disorder are more susceptible to illness or even death from certain food-borne infections like listeria and vibrio.
And alcohol can cause dehydration, which may worsen food poisoning symptoms and prolong recovery time, experts said.
How to Protect Yourself From Food Poisoning
Drinking alcohol is an unproven and potentially risky approach to preventing food poisoning, experts said.
“It would be better just to not eat the dodgy food to begin with,” Dr. Schaffner said — though he acknowledged that it’s often not possible to tell if a particular food is contaminated.
A good way to stay safe is to pay attention to food recalls, Dr. Schaffner said. And in the kitchen, use proper food safety techniques. Those include washing your hands often; avoiding cross contamination from raw meat, poultry and fish by keeping those items separate from other foods; cooking all foods to proper temperatures; and avoiding leaving perishable foods at room temperature for more than two hours.
These strategies are especially important for people who are most susceptible to severe illness from food-borne pathogens, including those with weakened immune systems, or those who are pregnant, younger than 5 or older than 65.
Dr. Moore acknowledged that the proven ways to prevent food poisoning are “kind of boring.”
But they’re effective, he said, and that’s what matters.
Credit: The New York Times
Who is more likely to lose weight on tirzepatide and why?
Team Metabolic Health
Tirzepatide, a once-weekly GIP/GLP-1 receptor agonist, is a medicine used for weight reduction in adults with obesity.
A new analysis of the SURMOUNT clinical trials reveals that the medicine, administered as a once-weekly injection, leads to significant weight reduction.
Across all doses and trials, women lost up to 24.6% of their body weight compared to 18.1% in men, indicating a potential sex-based difference with regard to drug response.
Obesity is the most common chronic health condition globally, affecting around 650 million adults.
It leads to serious issues like heart disease and type 2 diabetes, which increase health risks and healthcare costs.
Scientists have found different weight loss results in people taking tirzepatide. NurPhoto/Getty Images
Recent studies have shown that drugs targeting specific hormones involved in energy balance, such as GLP-1, can help people lose weight effectively and safely.
Another hormone, GIP, also plays a role in controlling weight, and a combination treatment that targets both GIP and GLP-1 receptors may be even more effective.
Tirzepatide is a new medication that works on both GIP and GLP-1 receptors and is already approved for treating type 2 diabetes.
Early research showed that it helped mice lose more weight compared to treatments that only target GLP-1. In studies with people who have type 2 diabetes, it also showed promising results for weight loss.
For example, the SURMOUNT-1 (SM-1) trial looked at how well tirzepatide works for weight loss in people with obesity or overweight who do not have diabetes.
To further explore potential differences in how men and women respond to the treatment, researchers conducted a post-hoc analysis of the SURMOUNT (SM) program, which included four clinical trials (SM-1 to SM-4).
Their analysis shows that a weekly injection of tirzepatide results in substantial weight loss for both men and women, with women experiencing greater reductions in weight.
Their findings, presented at the Annual Meeting of the European Association for the Study of Diabetes (EASD) in Madrid (September 9-13), compared tirzepatide to a placebo over 72 to 88 weeks in 4,677 adults (2,999 women and 1,678 men) with obesity.
Lead author, Luis-Emilio García-Pérez, MD, PhD, MBA, explained the key findings to Medical News Today:
“This was a post-hoc sub-group data analysis of the SURMOUNT-1, SURMOUNT-2, SURMOUNT-3 and SURMOUNT-4 phase 3 trials that showed tirzepatide injections (5 mg, 10 mg, 15 mg) significantly reduced body weight compared to placebo regardless of sex, with greater body weight reduction associated with tirzepatide in females compared to males.”
— Luis-Emilio García-Pérez, MD
Impact of lead-in phases and sex on weight loss outcomes
While the SM-1 and SM-2 trials involved randomization immediately after a screening period, SM-3 had a 12-week lead-in phase with intensive lifestyle changes, and SM-4 had a 36-week lead-in with open-label tripeptide treatment.
In this analysis, body weight changes were evaluated in participants who had received at least one dose of tirzepatide (5, 10, or 15 mg) or placebo.
The study used a mixed model to assess differences in average weight change over time (from baseline to the end of the study: 72 weeks for SM-1 to SM-3 and 88 weeks for SM-4).
Logistic regression was used to evaluate whether male and female participants differed in achieving specific weight loss milestones, including reductions of 5%, 10%, and 15% of their body weight.
Across the four trials, women made up 51% to 71% of participants.
And at the start of the trials, women weighed less than men on average. For instance, in SM-1, the average weight of female participants was 99.8 kg, compared to 115.2 kg for men.
However, both men and women had similar body mass index (BMI) levels, indicating similar levels of obesity.
Sex-based variations in weight loss results
In terms of weight loss, the estimated reduction in body weight for those taking tirzepatide was significantly greater than for those on placebo, regardless of sex.
Women saw a greater percentage of weight loss than men across all doses.
For example, women lost up to 24.6% of their body weight, while men lost up to 18.1%. This difference was statistically significant in all studies.
When looking at specific weight loss thresholds, both men and women were far more likely to achieve reductions of 5%, 10%, and 15% body weight with tirzepatide compared to placebo.
However, in most trials, there was no significant difference between men and women in reaching these thresholds.
An exception was observed in the SM-3 trial, where women were more likely than men to achieve the 5% and 10% weight reduction goals.
The safety outcomes were generally similar for both men and women, though women reported higher rates of nausea and vomiting compared to men.
“The analysis showed that weight reduction happens consistently regardless of sex, however, tirzepatide was associated with greater weight loss in women than in men. Prevalence of obesity and treatment outcomes may differ between males and females as a result of physiological, sociocultural and environmental factors.”
— Luis-Emilio García-Pérez, MD
However, he added that “the results of this post hoc analysis have to be interpreted with caution as they are hypothesis-generating only.”
“The potential mechanisms of this finding need further research,” Dr. García-Pérez explained.
Findings could lead to more personalized treatment plans
Mark A. Anton, MD, medical director at Slimz Weightloss, not involved in this research, said that this research on body weight reduction with tirzepatide is promising and aligns with our clinical observations.”
“The findings could provide deeper insights into the efficacy of tirzepatide across different demographics, potentially allowing for more personalized treatment plans,” Anton explained.
“These findings could mean more tailored and effective weight loss solutions, enhancing the overall success rates and improving long-term health outcomes,” he added.
Mir B. Ali, MD, board certified bariatric surgeon and medical director of MemorialCare Surgical Weight Loss Center at Orange Coast Medical Center in Fountain Valley, CA, who was also not involved in the research, noted that “this is an interesting study comparing weight loss in males versus females.”
“This is somewhat contrary to what I see in surgical weight loss patients; to me this study demonstrates that females are more responsive to these medications, though both males and females showed significant benefits,” Ali added.
“These findings may help prescribing providers set more realistic expectations based on gender for patients seeking these medications. It would be helpful to see more research in this area and make a consideration for changing dosing based on gender.”
— Mir B. Ali, MD
View the original article on Medical News Today
Credit: aol.com
Deadly high blood pressure during pregnancy is on the rise
Team Metabolic Health
Sara McGinnis was nine months pregnant with her second child and something felt off. Her body was swollen. She was tired and dizzy.
Her husband, Bradley McGinnis, said she had told her doctor and nurses about her symptoms and even went to the emergency room when they worsened. But, Bradley said, what his wife was told in response was, “‘It’s summertime and you’re pregnant.’ That haunts me.”
Two days later, Sara had a massive stroke followed by a seizure. It happened on the way to the hospital, where she was headed again due to a splitting headache.

In August, Mary Collins and daughter Rory were both still recovering after Collins experienced severe high blood pressure in her pregnancy, which led to Rory’s premature delivery. Pix: Thom Bridge for KFF Health News
Sara, from Kalispell, Mont., never met her son, Owen, who survived through an emergency delivery and has her oval eyes and thick dark hair. She died the day after he was born.
Sara had eclampsia, a stroke in pregnancy caused by persistent high blood pressure, also known as hypertension. High blood pressure makes the heart work in overdrive, which can damage organs.
Sara died in 2018. Today, more pregnant women are being diagnosed with dangerously high blood pressure, a finding that could save their lives. Recent studies show the rates of newly developed and chronic maternal high blood pressure have roughly doubled since 2007. Researchers say the jump in cases is likely due in part to more testing that discovers the conditions.
But that’s not the whole story. Data shows that the overall maternal mortality rate in the U.S. is also climbing, with high blood pressure one of the leading causes.
A new threshold
Medical experts are trying to stem the tide. In 2022, the American College of Obstetricians and Gynecologists lowered the threshold for when doctors should treat pregnant and postpartum patients for high blood pressure. And federal agencies offer training in best practices for screening and care. Federal data shows that maternal deaths from high blood pressure declined in Alaska and West Virginia after implementation of those guidelines. But applying those standards to everyday care takes time, and hospitals are still working to incorporate practices that might have saved Sara’s life.

Mary Collins does not have some of the risk factors for preeclampsia, such as being over 35 or being overweight. Doctors and researchers are not sure of all the reasons that high blood pressure during pregnancy is becoming more common. Pix: Thom Bridge for KFF Health News
In Montana, which last year became one of 35 states to implement the federal patient safety guidelines, more than two-thirds of hospitals provided patients with timely care, said Annie Glover, a senior research scientist with the Montana Perinatal Quality Collaborative. Starting in 2022, just over half of hospitals met that threshold.
“It just takes some time in a hospital to implement a change,” Glover said.
“A natural stress test”
High blood pressure can damage a person’s eyes, lungs, kidneys, or heart, with consequences long after pregnancy. Preeclampsia — consistent high blood pressure in pregnancy — can also lead to a heart attack. The problem can develop from inherited or lifestyle factors: For example, being overweight predisposes people to high blood pressure. So does older age, and more people are having babies later in life.
Black and Indigenous people are far more likely to develop and die from high blood pressure in pregnancy than the general population.
“Pregnancy is a natural stress test,” said Natalie Cameron, a physician and an epidemiologist with Northwestern University’s Feinberg School of Medicine, who has studied the rise in high blood pressure diagnoses. “It’s unmasking this risk that was there all the time.”
But pregnant people who don’t fit the typical risk profile are also getting sick, and Cameron said more research is needed to understand why.
Mary Collins, 31, of Helena, Mont., developed high blood pressure while pregnant this year. Halfway through her pregnancy, Collins still hiked and attended strength training classes. Yet, she felt sluggish and was gaining weight too rapidly while her baby’s growth slowed drastically.
Collins said she was diagnosed with preeclampsia after she asked an obstetrician about her symptoms. Just before that, she said, the doctor had said all was going well as he checked her baby’s development.
“He pulled up my blood pressure readings, did a physical assessment, and just looked at me,” Collins said. “He was like, ‘Actually, I’ll take back what I said. I can easily guarantee that you’ll be diagnosed with preeclampsia during this pregnancy, and you should buy life flight insurance.’”
Indeed, Collins was airlifted to Missoula, Mont., for the delivery and her daughter, Rory, was born two months early. The baby had to spend 45 days in a neonatal intensive care unit. Both Rory, now about 3 months old, and Collins are still recovering.
The typical cure for preeclampsia is delivering the baby. Medication can help prevent seizures and speed up the baby’s growth to shorten pregnancy if the health of the mother or fetus warrants a premature delivery. In rare cases, preeclampsia can develop soon after delivery, a condition researchers still don’t fully understand.
Wanda Nicholson, chair of the U.S. Preventive Services Task Force, an independent panel of experts in disease prevention, said steady monitoring is needed during and after a pregnancy to truly protect patients. Blood pressure “can change in a matter of days, or in a 24-hour period,” Nicholson said.
And symptoms aren’t always clear-cut.
That was the case for Emma Trotter. Days after she had her first child in 2020 in San Francisco, she felt her heartbeat slow. Trotter said she called her doctor and a nurse helpline and both told her she could go to an emergency room if she was worried but advised her that it wasn’t needed. So she stayed home.
In 2022, about four days after she delivered her second child, her heart slowed again. That time, the care team in her new home of Missoula checked her vitals. Her blood pressure was so high the nurse thought the monitor was broken.
“You could have a stroke at any second,” Trotter recalled her midwife telling her before sending her to the hospital.
Trotter was due to have her third child in September, and her doctors planned to send her and the new baby home with a blood pressure monitor.
Measuring the problem
More monitoring could help with complex maternal health problems, said Stephanie Leonard, an epidemiologist at Stanford University School of Medicine who studies high blood pressure in pregnancy.
“Blood pressure is one component that we could really have an impact on,” she said. “It’s measurable. It’s treatable.”
More monitoring has long been the goal. In 2015, the federal Health Resources and Services Administration worked with the American College of Obstetricians and Gynecologists to roll out best practices to make birth safer, including a specific guide to scan for and treat high blood pressure. Last year, the federal government boosted funding for such efforts to expand implementation of those guides.
“So much of the disparity in this space is about women’s voices not being heard,” said Carole Johnson, head of the health resources agency.

Mary Collins and her daughter, Rory. Despite years of federal efforts to make birth safer, hospitals are still trying to match screening and treatment for preeclampsia with best practices. Pix: Thom Bridge for KFF Health News
The Montana Perinatal Quality Collaborative spent a year providing that high blood pressure training to hospitals across the state. In doing so, Melissa Wolf, the head of women’s services at Bozeman Health, said her hospital system learned that doctors’ use of its treatment plan for high blood pressure in pregnancy was “hit or miss.” Even how nurses checked pregnant patients’ blood pressure varied.
“We just assumed everyone knew how to take a blood pressure,” Wolf said.
Now, Bozeman Health is tracking treatment with the goal that any pregnant person with high blood pressure receives appropriate care within an hour. Posters dot the hospitals’ clinic walls and bathroom doors listing the warning signs for preeclampsia. Patients are discharged with a list of red flags to watch for.
Katlin Tonkin is one of the nurses training Montana medical providers on how to make birth safer. She knows how important it is from experience: In 2018, Tonkin was diagnosed with severe preeclampsia when she was 36 weeks pregnant, weeks after she had developed symptoms. Her emergency delivery came too late and her son Dawson, who hadn’t been getting enough oxygen, died soon after his birth.
Tonkin has since had two more sons, both born healthy, and she keeps photos of Dawson, taken during his short life, throughout her family’s home.
Credit: npr.org
Baking Soda Weight Loss Trend: Is It Worth Trying?
Team Metabolic Health
Social media users are claiming that drinking baking soda in water is a magic weight loss hack, but experts aren’t so sure.
Another day, another allegedly magical weight loss hack touted by social media users.
Online platforms are brimming with claims about quick and easy ways to lose weight, and the latest involves diluting baking soda in water and drinking it.
On TikTok, social media users claim that drinking sodium bicarbonate — baking soda — daily has helped reduce their appetite, shed unwanted pounds, and reduce cellulite.
But much like other social media weight loss trends, experts say any hack that seems too good to be true, probably is.

Image by New Africa via Shutterstock
Does drinking baking soda for weight loss work?
Social media users claim that baking soda aids weight loss by helping the body break down fat due to its alkaline nature and ability to neutralize stomach acids. The theory is that by increasing the body’s pH levels and making it more alkaline, fat storage efficiency and metabolism are enhanced by influencing enzyme activity and insulin sensitivity.
But there is no evidence to suggest that it can actually impact body fat in any way.
“Drinking baking soda in water for weight loss is a popular claim on TikTok, but there is limited scientific evidence supporting its effectiveness,” says Michelle Routhenstein, MS, RD, a preventive cardiology dietitian at EntirelyNourished.com.
While baking soda’s alkaline nature may temporarily increase feelings of fullness, Routhenstein says it does not directly lead to weight loss.
Naysha Isom, M.D., a board-certified physician specializing in preventive health and sustainable weight loss, likewise tells Healthnews that this claim remains entirely theoretical.
“Unlike controlled laboratory conditions, the human body tightly regulates its pH, making it unlikely that consuming baking soda would significantly impact weight loss,” she says. “This concept isn’t any different than drinking commercially available alkaline water found in most grocery stores.”
Plus, she says ingesting baking soda can cause temporary water retention, bloating, and gas, which some may mistake for appetite suppression. But these perceived feelings of fullness are not actually a sustainable method to suppress one’s appetite, she says.
Is drinking baking soda harmful?
In addition to the lack of evidence supporting baking soda’s ability to promote weight loss, Routhenstein and Isom say this trend also presents health risks.
“People should take extreme caution with online weight loss trends, especially if they have heart disease, are taking certain medications, or have medical conditions, as these claims often lack scientific validation, may interact with prescribed medications, and may overlook individual health conditions,” Routhenstein says. “Potential negative health issues from doing this include electrolyte imbalances, high blood pressure, and digestive problems due to its high sodium content.”
Baking soda’s high sodium content can also reduce the effectiveness of antihypertensive drugs, she says — such as ACE inhibitors and diuretics — by increasing blood pressure or causing fluid retention.
Sodium bicarbonate can also impact the efficacy of blood thinners by altering the body’s acid-base balance and potentially leading to increased bleeding risk, Routhenstein explains.
And excessive sodium intake from baking soda can negatively affect heart health by increasing blood pressure and straining the cardiovascular system, she adds.
Using baking soda with other antacids or proton pump inhibitors can also lead to excessive alkalinity, potentially causing metabolic alkalosis or diminishing the effectiveness of the other antacids.
Anyone who consumes too much baking soda can potentially disturb their body’s pH balance, leading to metabolic alkalosis, Isom adds. Symptoms of metabolic alkalosis include nausea, vomiting, muscle twitching, and confusion.
Overconsuming it can also disrupt essential electrolyte levels, she says, including potassium, calcium, and chloride — which are critical for proper muscle, heart, kidney, and brain function.
“Online weight loss trends often promise quick fixes and are enticing due to their perceived affordability, convenience, and availability of products or supplies,” Isom concludes. “However, these trends seldom deliver sustainable results.”
Credit: healthnews.com
