6 amazing benefits of starting your day with a morning run
Team Metabolic Health
Running in the morning offers numerous benefits, from boosting metabolism to enhancing mental clarity. Here are six amazing reasons to start your day with a run
Running is undoubtedly a fantastic way to achieve your fitness goals, embraced by millions for its numerous benefits. It’s one of the simplest forms of exercise, accessible to people of all ages. But did you know that running first thing in the morning feels like living two lives? The mental boost it gives your day, the thrill of a magical sunrise and the tranquillity of being immersed in nature while the rest of the world sleeps—there’s truly no better feeling. We often underestimate how powerful a morning run can be, whether it’s a solo journey or a pre-work running club. Check out some of the amazing benefits of a morning run below.

Running in the morning offers a range of incredible benefits that can enhance your overall well-being.(Unsplash)
1. Improved mental health
Running positively impacts your mental health and boosts your self-worth. A morning run, especially outdoors, lets you enjoy nature’s beauty and the calm of fewer people and cars, making it a refreshing and rewarding start to your day.
Explore Lifestyle, Entertainment, Culture & more with HT Brunch App. Download now!
2. Better Sleep
If you struggle to sleep, try running in the morning. Studies show it promotes deeper sleep, and establishing a routine of early runs can help you fall asleep faster and improve your sleep quality.
3. Improves heart health
Morning running is an aerobic exercise with numerous health benefits, especially for heart health. It raises your heart rate, strengthens your cardiovascular system, and, with consistency, reduces the risk of heart disease and related conditions.
4. Better joint health
Running in the morning can help prevent joint pain and injury. Our joints are naturally stiffer in the morning, making them less prone to injury. By running early, you allow your body to warm up gradually, reducing strain on your joints and preparing for a longer, safer run.
Promoted
5. Helps to create consistency
Starting your day with a run before work helps establish a consistent exercise routine and develop discipline. Committing to a morning run makes it easier to build the habit of regular exercise, which can boost your energy, productivity, and success in other areas of your life.
6. Jump-starts your metabolism
Morning runs can significantly boost your metabolism, the process that converts food into energy. Running early activates your body’s metabolic functions, increasing calorie burn throughout the day and aiding in weight loss.
Credit: Hindustan Times
Health Rounds: Next generation Lilly weight-loss drug shows added heart, liver benefits
Team Metabolic Health
This is an excerpt of the Health Rounds newsletter, where we present latest medical studies twice a week. To receive it in your inbox for free sign up here, opens new tab
Eli Lilly’s (LLY.N), opens new tab experimental next generation weight-loss drug mimics three hormones instead of just one or two and continues to show promising clinical trial results for additional health benefits, the company said.

Eli Lilly logo is shown on one of the company’s offices in San Diego, California, U.S., September 17, 2020. REUTERS/Mike Blake/File Photo
Researchers reported, opens new tab at the recent European Society of Cardiology meeting in London that Lilly’s retatrutide significantly reduced patients’ blood lipid levels and cardiovascular risks in a mid-stage trial.
At 48 weeks, for example, retatrutide had reduced levels of triglycerides by up to 40.6%, and levels of a protein called apoC-III involved in glucose metabolism and inflammation by 38%.
Lilly had earlier announced that in the same trial patients taking injections of retatrutide at the highest dose had lost roughly 24% of their body weight, exceeding what the current popular weight-loss drugs demonstrated in clinical trials.
Credit: Reuters
Blood test that can predict if weight loss can help manage sugar-Here’s all you need to know
Team Metabolic Health
They found that measuring certain fats in serum before one loses weight could predict which type of blood sugar will improve following weight loss.
A blood test that can measure fats in serums could help predict if weight loss can be effective in helping a pre-diabetic patient manage blood sugar levels. People with pre-diabetes have higher blood sugar levels but not yet in the diabetic range.
Analysing fats in blood serum, researchers at the University of Sydney, Australia, found that while weight loss through dieting significantly impacted several types of lipids (fats), changes in different fats affected different types of blood sugar.
Six baseline bioactive sphingolipids primarily predicted changes in fasting plasma glucose. (Image Credits: Pixabay)
For example, changes in fasting blood sugar were linked to certain sphingolipids — a type of fat found in a cell’s outer layer — while those in HbA1c, insulin and insulin resistance were linked to other fats in blood serum.
“Six baseline bioactive sphingolipids primarily predicted changes in fasting plasma glucose. In addition, a number of baseline lipid species, mainly diacylglycerols and triglycerides, were predictive of clinical changes in hemoglobin A1c, insulin and HOMA-IR (Homeostatic Model Assessment for Insulin Resistance),” the authors wrote as quoted by news agency PTI.
Weight loss through a low-energy diet — low-carb, fibre-rich — is commonly recommended to help pre-diabetic people bring blood sugar levels back to normal. However, the researchers said that over half of these individuals do not achieve normal blood sugar levels afterwards.
They found that measuring certain fats in serum before one loses weight could predict which type of blood sugar will improve following weight loss. The findings are published in The American Journal of Clinical Nutrition.
“Our findings reveal that certain fats in the blood can tell us a lot about a person’s chances of improving their blood sugar levels through weight loss,” lead author Yanfei (Jacob) Qi from the university’s Centenary Institute said.
For the study, blood serum samples from 104 pre-diabetic participants were analysed before and after they started a low-energy diet for eight weeks. In this duration, the individuals were found to have lost at least eight per cent of their body weight.
Lipidomics — the use of AI-based techniques to study changes in hundreds of different lipids — was used in analysing the serum samples.
“(The findings) could be a game-changer in how we approach diabetes prevention, allowing us to personalise treatment plans for those who are less likely to benefit from standard diet recommendations,” Qi said as quoted by PTI.
Credit: Financial Express
Eli Lilly jumps deeper into AI with $409M Genetic Leap deal
Team Metabolic Health
Eli Lilly has vaulted into an AI-enabled drug discovery deal, partnering with RNA specialist Genetic Leap in a pact worth up to $409 million in upfront and milestone payments.
New York-based Genetic Leap is built on AI models designed to support the discovery of RNA-targeted drugs. The stack features technologies for discovering new targets and finding ways to engage validated but undruggable targets. Astellas teamed up with the biotech to use the platform to find RNA-targeted small molecules against an undisclosed oncology target in 2022.

News of a deal with RNA specialist Genetic Leap comes after Eli Lilly pushed deeper into RNA by opening a $700 million nucleic acid R&D center. (Pix Credit: Getty Images Plus)
Now, Lilly has joined the list of Genetic Leap partners. The Big Pharma has entered into a research pact that will see Genetic Leap use its RNA-targeted AI platform to generate genetic drug candidates against selected targets. Lilly will pick targets in high-priority areas, and Genetic Leap will find oligonucleotide drugs against the targets.
The focus makes Genetic Leap part of a band of biotechs working to overturn traditional thinking about drugging RNA. As naturally polarized molecules with shallow binding pockets, the nucleic acid was seen as a poor fit for small molecules. However, over the past decade, biotechs such as Arrakis Therapeutics have set up shop and begun trying to target RNA.
Eli Lilly unwraps $700M nucleic acid R&D center in Boston Seaport, opens doors to biotechs
Neither party has disclosed the size of the upfront fee, which is typically a small proportion of the total value in such early-stage deals, but they have revealed Lilly will pay $409 million if the collaboration hits all its milestones. Tiered royalties could add to the total. News of the deal comes weeks after Lilly pushed deeper into RNA research by opening a $700 million nucleic acid R&D center in the Boston Seaport. Lilly invested in the site after identifying improvements in the delivery of DNA and RNA medicines as a way to unlock difficult to treat targets in key strategic areas such as neurodegeneration, diabetes and obesity.
Credit: ftp.digitalpharmaeast.com
Rethinking Addiction as a Chronic Brain Disease
Team Metabolic Health
Some researchers argue that the roles of social environment and personal choice have to be considered in order to make progress in treating people addicted to drugs.
The message emblazoned on a walkway window at the airport in Burlington, Vt., is a startling departure from the usual tourism posters and welcome banners:
“Addiction is not a choice. It’s a disease that can happen to anyone.”
The statement is part of a public service campaign in yet another community assailed by drug use, intended to reduce stigma and encourage treatment.
For decades, medical science has classified addiction as a chronic brain disease, but the concept has always been something of a hard sell to a skeptical public. That is because, unlike diseases such as Alzheimer’s or bone cancer or Covid, personal choice does play a role, both in starting and ending drug use. The idea that those who use drugs are themselves at fault has recently been gaining fresh traction, driving efforts to toughen criminal penalties for drug possession and to cut funding for syringe-exchange programs.
But now, even some in the treatment and scientific communities have been rethinking the label of chronic brain disease.
Pix Credit: Medar De La Cruz
In July, behavior researchers published a critique of the classification, which they said could be counterproductive for patients and families.
“I don’t think it helps to tell people they are chronically diseased and therefore incapable of change. Then what hope do we have?” said Kirsten E. Smith, an assistant professor of psychiatry and behavioral sciences at Johns Hopkins School of Medicine and a co-author of the paper, published in the journal Psychopharmacology. “The brain is highly dynamic, as is our environment.”
The recent scientific criticisms are driven by an ominous urgency: Despite addiction’s longstanding classification as a disease, the deadly public health disaster has only worsened.
Almost no one is calling for entirely scrapping the disease model . Few dispute that constant use of stimulants like methamphetamine and opioids like fentanyl have a detrimental effect on the brain.
But some scientists argue that brain-centric disease characterizations of addiction do not sufficiently incorporate factors like social environment and genetics. In the recent critique, researchers contended that, rather than emphasizing the brain’s brokenness in perpetuity, an addiction definition should include the motivation or context in which the person chose to use drugs.
That choice, they said, is often about seeking an escape from intractable conditions such as a fraught home, undiagnosed mental health and learning disorders, bullying or loneliness. Generations of family addiction further tip the scales toward substance use.
And in many environments, they added, drugs are simply more readily available than healthier, rewarding options, including education and jobs.

Kirsten E. Smith, an assistant professor at Johns Hopkins School of Medicine, disputes the definition of addiction as a chronic brain disease. “I am not in recovery,” she said. “I have recovered.” Pix Credit: Schaun Champion for The New York Times
Fentanyl Overdoses: What to Know
Devastating losses. Drug overdose deaths, largely caused by the synthetic opioid drug fentanyl, reached record highs in the United States in 2021. Here’s what you should know to keep your loved ones safe:
Understand fentanyl’s effects. Fentanyl is a potent and fast-acting drug, two qualities that also make it highly addictive. A small quantity goes a long way, so it’s easy to suffer an overdose. With fentanyl, there is only a short window of time to intervene and save a person’s life during an overdose.
Stick to licensed pharmacies. Prescription drugs sold online or by unlicensed dealers marketed as OxyContin, Vicodin and Xanax are often laced with fentanyl. Only take pills that were prescribed by your doctor and came from a licensed pharmacy.
Talk to your loved ones. The best way to prevent fentanyl use is to educate your loved ones, including teens, about it. Explain what fentanyl is and that it can be found in pills bought online or from friends. Aim to establish an ongoing dialogue in short spurts rather than one long, formal conversation.
Learn how to spot an overdose. When someone overdoses from fentanyl, breathing slows and their skin often turns a bluish hue. If you think someone is overdosing, call 911 right away.
Buy naloxone. If you’re concerned that a loved one could be exposed to fentanyl, you may want to buy naloxone. The medicine can rapidly reverse an opioid overdose and is often available at pharmacies without a prescription. Narcan, the nasal spray version of naloxone, has received F.D.A. approval to be sold over the counter and should be widely available by late summer.
Choosing drugs could then be understood not as a moral failing but as a form of decision making, with its own bleak logic.

Dr. Nora Volkow, director of the National Institutes on Drug Abuse, said the current model still holds value, and refers to addiction as “a chronic, treatable medical condition.” Pix Credit: Hailey Sadler for The New York Times
In combination with medications that subdue opioid cravings, therapists could help patients identify the reasons that led them to use drugs and then encourage them to make choices that result in meaningful, sustained rewards.
In a 2021 paper in the journal Neuropsychopharmacology, Dr. Markus Heilig, a former research director at the National Institute on Alcohol Abuse and Alcoholism, defended the brain-disease diagnosis, saying evidence has been amply documented. But, his paper acknowledges, “Brain-centric accounts of addiction have for a long time failed to pay enough attention to the inputs that social factors provide to neural processing behind drug seeking and taking.”
In clinical practice, the term “addiction” is becoming increasingly nuanced. John F. Kelly, a psychologist and professor of addiction psychiatry at Harvard Medical School, defines addiction as “a severe substance use disorder that is at the point where there are lots of changes in the prefrontal cortex as well as deeper areas of the brain” that regulate emotion and behavior.
But only a small minority of people meet that criteria, he said. “Even within that severe range, there’s a lot of different degrees of impairment that can occur,” Dr. Kelly added. Genetics can exacerbate the severity of the response.
He offered the analogy of boarding a speeding train. “It starts off being an exhilarating ride, but at some point it gets out of control and becomes derailed. It’s a matter of when you can pull the emergency cord and get off,” he said, noting that some drug users never get the chance to do so before it’s too late.
That moment differs for everyone: “People will only change when there are negative consequences, but also when there is hope and optimism that change is possible, likely and sustainable.”
In disputing the characterization of addiction as a disease marked by compulsive or relapsing use, a few experts have argued that some drug and alcohol users can quit without treatment — and even return to occasional safe use.
Dr. Smith began using drugs in adolescence and became addicted to heroin. During her darkest stretch, when she was 23, she was injecting four times daily. She was involved in two bank robberies and then served almost four years in federal prison, where she attended a modest treatment program. Upon release, she finished college and completed graduate and postdoctoral studies.
It has been more than six years since she used opioids and more than 15 since she was addicted to them. Dr. Smith is quick to credit the benefits of her middle-class background and family support.
She rejects the idea that she will always be shackled to a chronic brain condition.
“I am not in recovery,” she said. “I have recovered.”
Theories of addiction have been debated for centuries. In the 1780s, Dr. Benjamin Rush, a signer of the Declaration of Independence, began calling alcoholism “that odious disease.” (“The different preparations of opium are a thousand times more safe and innocent than spiritous liquors,” he wrote.)
Compounding the modern confusion about the nature of addiction, psychiatry keeps refining criteria for what it labels “substance use disorder.” In the current edition of its diagnostic manual, the D.S.M.-V, a person has a mild disorder if they meet at least two of 11 symptoms. The more the symptoms, the greater the severity of the disorder.
Research on drug use began to take off in the 1970s. By 1997 Alan I. Leshner, then the head of the National Institute on Drug Abuse, published the foundational position paper, “Addiction Is a Brain Disease, and It Matters.”
To the public, policymakers and even health care workers, he wrote, “Addiction as a chronic, relapsing disease of the brain is a totally new concept.”
But he did not overlook contributing factors. “Not only must the underlying brain disease be treated, but the behavioral and social cue components must also be addressed,” he wrote.
His much-cited research summary, which appeared a year after Purdue Pharma launched the highly addictive prescription opioid OxyContin, had a powerful, positive effect. The brain-disease designation would stimulate funding for research, be used to expand insurance coverage for treatment and prompt changes in public policy and criminal law, where newly minted drug courts—now increasingly called “recovery courts”—urged defendants into treatment. The brain-disease framework would eventually be adopted by mainstream medicine, including the surgeon general.
And it offered patients and families a building block toward compassion as well as ways to counter ubiquitous scorn.
The model continues to hold value, said Dr. Nora Volkow, who now leads the institute. She refers to addiction as “a chronic, treatable medical condition.”
In a statement, she added, “Acknowledging that addiction involves changes to the brain does not discount the many genetic, social, environmental and other factors that also play an important role.”
Whether the brain will ever sufficiently recover after long abstinence, however, needs further studying, argued a 2022 review of the research, though the authors suggested that evidence is promising.
But as academics wrestle with how to frame addiction, patients and loved ones struggle painfully with the lack of certainty.
Nadia, whose father fatally overdosed on fentanyl in 2023, said that defining addiction as a disease lets users off the hook of responsibility.
“It’s difficult to hear people call addiction a disease, like cancer or progressive illnesses,” wrote Nadia, who lives in Minneapolis but asked that her last name be withheld to protect her family’s privacy. “My father chose drugs, time and time again. He missed all three of my graduations, my wedding and the birth of my child, as well as all the milestones of my sister. It’s hard to be told that he can’t control it. That we weren’t important enough for him to overcome it.”
Nadia was among the hundreds of readers who responded to questions from The New York Times about their families’ struggles with substance use. Many said that they agonized: They were furious with the person using drugs or alcohol. Yet many also felt guilty for bitterly resenting a parent, sibling, child or spouse who, they also accepted, was sick with a disease.
“People want to relieve themselves of the burden of the mixed emotions they feel towards their loved one, but that’s the burden inherent in the condition,” said Keith Humphreys, a psychologist and an addiction expert at Stanford University. That is in part why, he said, it’s easier for people to see addiction in absolutist terms — as a choice or a disease.
Overwhelmingly, family members described their burnout. “When a loved one is addicted to drugs it’s like they’ve been bitten by a vampire,” wrote Robin Pratt, whose sister used opioids for a dozen years. “They never stop plotting what they can take from you to support their habit. The same person who, before drugs, you would have trusted with your life, becomes someone you wouldn’t even trust with your purse.”
Almost 30 years ago, when Dr. Leshner argued for the brain-disease designation, he did so in part to break through what he called the long-simmering “imprecision and misconception” around addiction.
He then added: “In fact, if it were possible, it would be best to start all over with some new, more neutral term.”
Credit: The New York Times
Experts highlight the effects of intermittent fasting on the body
Team Metabolic Health
It is crucial for individuals considering intermittent fasting to consult with a healthcare professional, particularly if they have underlying health conditions, mentioned Dr Kumar
Intermittent fasting (IF) has gained popularity for its potential benefits, including weight loss and improved metabolic health. However, concerns about its impact on the liver, a vital organ responsible for detoxification, metabolism, and digestion, and the heart are often not discussed.
Stating that intermittent fasting is a Western concept, Dr Shiv Kumar Sarin, gastroenterologist, the Institute of Liver and Biliary Sciences, told ANI, “IF requires you to eat in a particular window and to fast for 14 or 16 hours. That’s not a great idea. In fact, it can increase your cardiac problem.”
Let’s understand more about liver health (Source: Getty Images/Thinkstock)
Dr M Sai Sudhakar, director, Cath Lab, chief interventional cardiologist, chief cardiac transplant physician, Gleneagles Hospitals, Lakdi Ka Pul, Hyderabad said intermittent fasting, while popular for its potential health benefits, can have damaging effects on the heart if not approached carefully. “Prolonged fasting periods can lead to electrolyte imbalances, particularly in potassium, magnesium, and sodium, which are crucial for maintaining proper heart function. These imbalances can result in arrhythmias, or irregular heartbeats, which can be life-threatening. Additionally, fasting can elevate cortisol levels, the body’s primary stress hormone. Chronic high levels of cortisol increase blood pressure and heart rate, placing extra strain on the cardiovascular system and heightening the risk of heart disease over time,” said Dr Sudhakar.
However, Dr Ranjan Modi, senior consultant and head, interventional cardiology, Sarvodaya Hospital, Sector-8, Faridabad said research results on intermittent fasting are mixed. “Short-term studies suggest there is greater weight loss with intermittent fasting than with regular calorie cutting. But longer studies — from six months to one year — have not all found this to be true,” Dr Modi added.

Intermittent fasting and liver health: All you need to know (Source: Getty Images/Thinkstock)
A study from the American Heart Association’s Epidemiology and Prevention noted that restricting eating times to fewer than eight hours a day may be linked to a higher risk of dying of heart disease. “But a review of studies on intermittent fasting found that the weight and blood sugar changes reported were small. More research is needed to see whether regular fasting can reduce the risk of heart disease,” said Dr Modi.
Further, Dr Rajiv Kovil, head of diabetology, Zandra Healthcare and co-founder of Rang De Neela initiative said the liver is responsible for vital functions like aiding digestion, metabolism, detoxification, regulating hormones, and storing essential nutrients. “Non-alcoholic fatty liver disease (NAFLD) or fatty liver (steatosis) occurs when the fat starts to accumulate around your liver cells by slowing the process of breaking down fat,” said Dr Kovil.
From a medical perspective, Dr Chandan Kumar K N, senior consultant hematologist and lead T, Gleneagles Hospitals, Lakdi Ka Pul, Hyderabad said intermittent fasting generally does not damage different body parts like the heart or liver in healthy individuals. “In fact, some studies suggest that IF may have protective effects on the liver by reducing fat accumulation, lowering inflammation, and improving insulin sensitivity,” said Dr Kumar, adding that it can be particularly beneficial in preventing or managing conditions like NAFLD.
But according to a 2023 review published in Diabetes, Metabolic Syndrome and Obesity, although some studies suggest that IF may have potential benefits for NAFLD, the evidence is still “limited and inconclusive”.
However, IF could potentially stress the liver in individuals with pre-existing liver conditions, such as cirrhosis or advanced NAFLD, said Dr Kumar. “Prolonged fasting periods might lead to a drop in blood sugar levels, forcing the liver to work harder to produce glucose, which could exacerbate existing liver issues,” said Dr Kumar.
It is crucial for individuals considering intermittent fasting to consult with a healthcare professional, particularly if they have underlying health conditions, mentioned Dr Kumar. Personalised medical advice ensures that fasting practices are safe and appropriate for one’s health status, said Dr Kumar.
Credit: The Indian Express
Study reveals your nose can tell a lot about these hidden diseases
Team Metabolic Health
From acne to wolf’s nose, here’s how the nose can tell us a lot about our health.
The nose is a prominent feature on the face, but thanks to unconscious selective attention, we can choose to not let it get in our line of vision. However, even though the brain works hard to ignore this prominent feature from hindering our view, we should not take the nose lightly, for it can be the messenger of many hidden diseases. A recent study, led by Dan Baumgardt, University of Bristol, stated that the nose can help us diagnose external skin conditions and internal diseases.

The study states that the nose can help us diagnose external skin conditions and internal diseases. (Unsplash)
Acne vulgaris and acne rosacea:
Acne vulgaris is one of the most common types of acne that can affect the nose. It happens when the tiny glands in the skin get clogged and lead to blackheads. These blackheads can develop in larger lumps, get infected, inflamed and pus-filled and can scar the skin.
Acne rosacea, on the other hand, is an inflammatory skin condition that leads to reddening of the skin, mostly the nose and the cheeks. Acne rosacea can lead to rhinophyma – the condition where the skin of the nose starts to grow and thicken, making significant changes in the appearance.
Wolf’s nose:
Also known as Sarcoidosis, wolf’s nose is an inflammatory disease that can affect any tissues in the body, including the lungs and the lymph nodes. This condition can lead to bluish or purplish patches on the body, usually on the nose, ears, the fingers and toes. Sarcoidosis on the nose is referred to as lupus pernio.
Trigeminal trophic syndrome:
The damage to the trigeminal nerve can lead to this condition. The nerve branches in the area of the skin surrounding the nostrils can get damaged, leading to dysregulated sensation. This is categorised by numbness, desensitisation, or prickles. Repeated damage can also lead to ulcers around the nostrils. However, this is different from skin picking disorder, where a person may feel psychologically compelled to pick skin.
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always seek the advice of your doctor with any questions about a medical condition.
Credit: Hindustan Times
Should women stop smoking before conception? Is there ‘no safe period’ for smoking during pregnancy? Study answers
Team Metabolic Health
A new study sheds light on whether women should stop smoking before conception and if there is ‘no safe period’ for smoking during pregnancy.
Most women stop smoking when they learn that they are with a child. Every cigarette packet comes with a warning against smoking while pregnant. But is there any ‘safe period’ for smoking during pregnancy? Should one stop before conception? A new study is answering all these questions.

Women should stop smoking before pregnancy, a new study suggests. (Pexels)
Break the habit of smoking while you’re trying to conceive
A new study from China published by the Journal of Epidemiology & Community Health found out that before pregnancy, even light smoking (one to two cigarettes daily) can lead to some ‘serious health issues’ for the newborn baby. The study also reaffirmed the common belief that smoking at any point during pregnancy is dangerous for the growing fetus. Therefore, it is better for women to break the habit while still trying to conceive.
The study collected data from birth certificates in the US National Vital Statistics System between 2016 and 2019. The researchers analysed 12,150,535 mother-newborns and the number of cigarettes smoked per day, ranging from 0 to over 20. They found that the timing of smoking cigarettes during pregnancy matters. Their research found that smoking should be avoided during all stages of pregnancy and debunked the myth that light smoking is not as harmful if you do it before you get pregnant in the first three months of pregnancy.
Health effects of smoking
There are several researches out there that document the health effects of smoking during pregnancy. They reveal that it can lead to a greater risk for premature birth, low birth weight, and developmental issues in the womb. Since the effects after birth are less understood, it has led many women to think it’s safe to smoke before and after pregnancy.
The research stated, “There is no safe period and no safe level of cigarette smoking shortly before or during pregnancy.” They added that the findings of the study ‘re-emphasise the need to prevent smoking initiation for non-smokers and to promote smoking cessation for smokers’.
Top of Form
What did the study find out?
The study found that “newborns of smokers showed a higher rate of requiring assisted ventilation after birth, assisted ventilation for over 6 hours, NICU admission for mechanical ventilation, and surfactant replacement therapy. They also showed more significant risks for sepsis, seizures, or issues with the brain.”
Additionally, “smoking before pregnancy was associated with a 27 per cent higher risk of newborn health issues. The risk was 31 per cent to 32 per cent if the mother smoked anytime during pregnancy.” The study added, “Even smoking 1 to 2 cigarettes a day before pregnancy led to a 16 per cent higher chance of newborn health problems. The risk rose to 31 per cent if they smoked 20 or more cigarettes a day.”
Credit: Hindustan Times
Eye Drops To Eliminate Need For Reading Glasses to Hit The Indian Market by October
Team Metabolic Health
Mumbai-headquartered Entod Pharmaceuticals launched “PresVu” eye drops made using pilocarpine – the medicine that treats ‘presbyopia’ by reducing the size of the pupils which helps to see objects up close.
Starting first week of October, prescription-based drops will be available across pharmacies costing Rs 350. The medicine is indicated for the treatment of mild to intermediate presbyopia for people aged 40 to 55 years.
After deliberating over the medicine for over two years, the drug regulatory agency has approved India’s first eye drops to remove the need for reading glasses.
On Tuesday, Mumbai-headquartered Entod Pharmaceuticals launched “PresVu” eye drops made using pilocarpine – the medicine that treats ‘presbyopia’ by reducing the size of the pupils which helps to see objects up close. Presbyopia condition is the age-linked decline in the eyes’ ability to focus on nearby objects and this condition typically becomes noticeable mid-40s and worsens until about age of late 60s.
In an interview with News18, Nikkhil K Masurkar, chief executive officer (CEO) of Entod Pharmaceuticals said a single drop of the medicine starts working in just 15 minutes and its effects remain for the next six hours. If the second drop is also poured within three to six hours of the first drop, the effect will stay even longer.
“Till now, there was no medicine-based solution for blurry, near-vision except wearing reading glasses, contact lenses or a few surgical interventions.”

Entod Pharmaceuticals specialises in ophthalmic, ENT and dermatology medicines and exports to more than 60 countries.
Who can buy this medicine?
Starting from the first week of October, prescription-based drops will be available across pharmacies costing Rs 350. The medicine is indicated for the treatment of mild to intermediate presbyopia for people aged 40 to 55 years.
Masurkar claims that the medicine is the first of its kind in India which is tested on Indian eyes and customised as per the genetic fulcrum of the Indian population.
“Similar medicines are available in foreign countries. However, those formulations are not tested on Indian eyes which are much different from caucasian eyes. We have made several changes in the formulation,” Masurkar said.
The product will be sold only on prescriptions by registered medical practitioners. The company has started training its field force to inform and educate doctors about the usage of the latest product.
Phase III successful, gearing up for post-launch surveillance
Masurkar explained that the company had applied for the DCGI approval in early 2022 and the company was asked to conduct phase III clinical trials.
“We conducted the trials at ten sites across India with more than 250 patients. The results and data were submitted to the regulatory agency. The subject expert committee approved the study and recommended for approval from the drug controller general,” he said.
82 per cent of the total 274 subjects did not face any side effects. Remaining patients reported minor transient side effects including irritation and redness in eyes, blurring of vision and headache. “These all were transient side effects and resolved in couple of days. Once patient adapts, there should not be issues. No patient was discontinued from the trial,” he said.
While the results of the study are yet to be published in a peer-reviewed journal, the company plans to conduct post-marketing surveillance at several big eye-care centres across India including All India Institute of Medical Sciences (AIIMS), New Delhi.
“We will get the results published in medical journals as well but right now, we are preparing for post-marketing surveillance which can help us understand the different aspects of the medicine,” Masurkar added.
Credit: news18.com
Novo Nordisk’s Ozempic shortage expected to continue into Q4
Team Metabolic Health
A box of Ozempic made by Novo Nordisk is seen at a pharmacy in London, Britain March 8, 2024. REUTERS/Hollie Adams/File Photo
Novo Nordisk (NOVOb.CO), opens new tab said the shortage of lower strengths of its diabetes drug Ozempic has deteriorated, with intermittent shortages for all strengths expected into the final quarter of 2024 due to increased demand and along with capacity constraints at some of its manufacturing sites.
In a note published by the European Medicines Agency (EMA) on Monday, the obesity drug maker recommended healthcare workers continue limiting treatment initiation of new patients on Ozempic and its other diabetic drug, Victoza, until the supply situation improves.
Credit: Reuters
Dialysis May Prolong Life for Older Patients. But Not by Much
Team Metabolic Health
In one recent study, the challenging regimen added 77 days of life after three years. Often, kidney disease can be managed in other ways.
Even before Georgia Outlaw met her new nephrologist, she had made her decision: Although her kidneys were failing, she didn’t want to begin dialysis.
Ms. Outlaw, 77, a retired social worker and pastor in Williamston, N.C., knew many relatives and friends with advanced kidney disease. She watched them travel to dialysis centers three times a week, month after month, to spend hours having waste and excess fluids flushed from their blood.
“They’d come home weak and tired and go to bed,” she said. “It’s a day until they feel back to normal, and then it’s time to go back to dialysis again. I didn’t want that regimen.”
She told her doctors, “I’m not going to spend my days bound to some procedure that’s not going to extend my life or help me in any way.”
Ms. Outlaw was mistaken on one point — dialysis can prolong the lives of patients with kidney failure. But a new study published in the journal Annals of Internal Medicine analyzed data from a simulated trial involving records from more than 20,000 older patients (average age: about 78) in the Veterans Health Administration system. It found that their survival gains were “modest.”

An at-home dialysis machine. Credit: Veasey Conway for The New York Times
Administration system. It found that their survival gains were “modest.”
How modest? Over three years, older patients with kidney failure who started dialysis right away lived for an average of 770 days — just 77 days longer than those who never started it.
“I think people would find that surprising,” said Dr. Manjula Tamura, a nephrologist and researcher at Stanford and a senior author of the study. “They would have expected a greater difference.”
Moreover, those patients spent less time at home; they were in a hospital, a nursing home or a rehab center for about 15 more days than those who never started dialysis.
Another group didn’t begin dialysis early but continued with “medical management” (which could help alleviate symptoms if needed), though half of them started dialysis at some later point. They lived for about the same amount of time as those who started dialysis right away.
“Our field has really been debating about the role of dialysis in patients who develop kidney disease in old age,” Dr. Tamura said. “It’s lifelong therapy and a major change to your lifestyle. It can lengthen life, but there are trade-offs.”
About a third of the population over age 65 have chronic kidney disease, according to the U.S. Renal Data System. The pluses and minuses of treatment add up differently for them than for younger patients.
Among older adults who progress to kidney failure, most also have diabetes and many have heart failure, pulmonary disease or other serious chronic illnesses. They may not be candidates for transplants, the only cure for kidney failure, either because they’re too ill or frail for surgery, or because the wait for donated kidneys can be yearslong.
About 13 percent of the patients with kidney failure who register with the Renal Data System begin peritoneal dialysis at home — a more common treatment in other countries but one that, with Medicare incentives to providers, is gaining ground in the United States, too. It involves filtering blood through the abdominal lining.
But a great majority, almost 84 percent in 2021, still turn to dialysis centers, despite the challenges of transportation and the significant time commitment. Hemodialysis, the treatment offered in centers, requires a catheter, graft or fistula to allow access to a patient’s blood vessels, and it can cause side effects like infections, fatigue and itching. And, as the new study indicates, dialysis often means more time spent in health care centers, where most older adults don’t want to be.
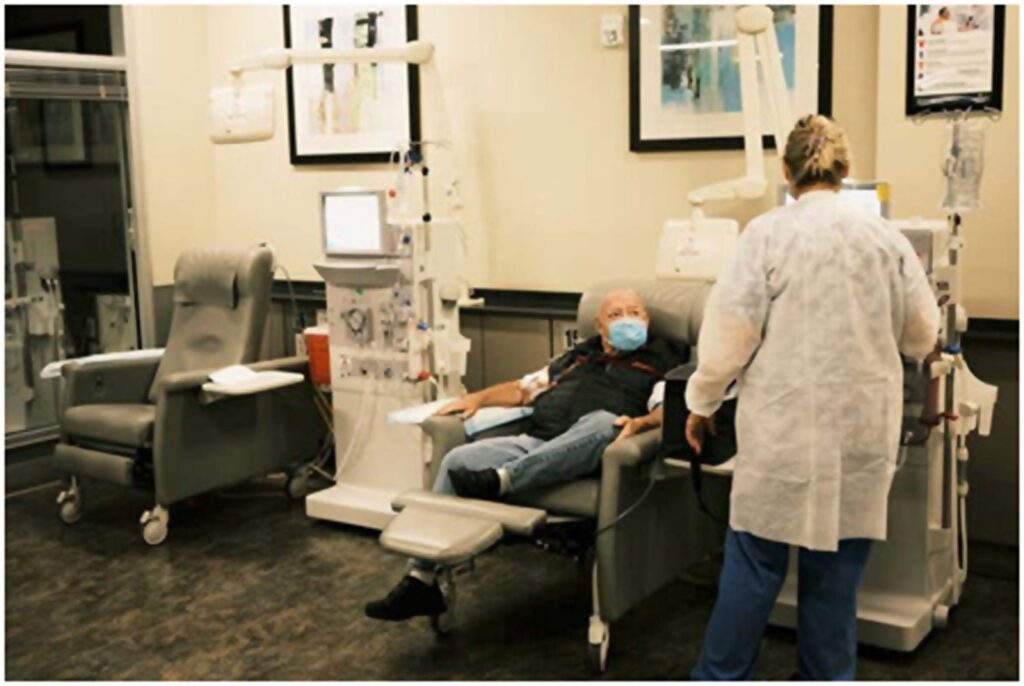
A patient undergoes dialysis treatment at the Cape Coral Kidney Center in Cape Coral, Fla.Credit: Zack Wittman for The New York Times
The alternative to dialysis goes by various names — medical management, conservative kidney management, supportive kidney care. In this scenario, nephrologists monitor their patients’ health, educating them about behavioral approaches, prescribing anti-nausea drugs like Zofran and diuretics like Lasix to reduce fluid retention, and adjusting their doses as needed.
Ms. Outlaw, for example, takes a diuretic, two blood pressure drugs and a phosphate binder, along with iron and calcium. Five years after her kidney failure diagnosis, she’s feeling fine, though sometimes a little weak or tired, she said. She still preaches once a month at Manifestation Church of Holiness in the neighboring city of Greenville.
Not everyone in conservative management remains that active. “Some of my other patients are in wheelchairs,” said Dr. Rasheeda Hall, a geriatric nephrologist who provides conservative care for Ms. Outlaw and others at the Durham VA Health Care System.
“They’re more complicated — we have to pay a lot more attention,” she said. “But they sleep in their own beds. They’re not in the hospital a lot. They have a better quality of life.”
Some older kidney patients find that strategy preferable, even if death should come a couple of months earlier.
Often, however, “if you ask patients, ‘Were you presented with a choice?’ many of them will say no,” Dr. Tamura said.
Dialysis “is definitely still the default,” Dr. Hall said. When she meets with older patients, “I say, ‘You know, dialysis is not the only thing — there are medications we have in our arsenal that can help,’” she said. “And they say, ‘Oh.’”
That response appears commonplace. Researchers at the University of Washington developed a “decision aid” — a booklet explaining conservative kidney management and its pros and cons — and tried it out on patients 75 and older with advanced kidney disease and their families. The goal: to prompt discussion of conservative management with a health care provider.
In the groups that received the booklet, about a quarter of patients and their relatives had such conversations. But among those who didn’t get the booklet, only 3 percent of patients discussed conservative management with a provider, and none of their family members did.
“I was quite pleased” with the results, said Dr. Susan Wong, a nephrologist and lead author of the study. “It can be intimidating for patients to bring up alternatives when a provider is pushing or recommending or positioning dialysis as the only right thing to do.”
In her clinic, she said, about a third of patients go to dialysis centers, a third begin dialysis at home and a third opt for conservative management without dialysis.
Practices are shifting somewhat among kidney patients and their doctors. The most recent statistics from the Renal Data System, for instance, show that the use of peritoneal dialysis at home more than doubled from 2008 to 2021; the proportion of patients traveling to dialysis centers declined.
“Several things in the kidney world appear to be getting better,” said Dr. Kevin Abbott, program director in the division of kidney, urologic and hematologic diseases at the National Institute of Diabetes and Digestive and Kidney Diseases.
The proportion of older Americans with kidney disease has fallen, in part reflecting the wider use of more effective blood pressure drugs in recent decades, he said. The new diabetes drugs that help reduce weight and blood sugar also show promise for treating kidney disease.
But it still often falls to patients themselves and their families to question whether they want to start dialysis, to ask about other options like conservative kidney management, and to weigh their choices.
If they’re waiting for health care professionals to alert them to the alternatives, they may have to wait quite a while.
Ms. Outlaw’s decision owed much to her spiritual beliefs. “I’ve had a good life, and I am still enjoying it,” she said. But “if I pass away, I know where I’m going. My relationship with the Lord is good.”
Like any kidney patient, she can always change her mind about treatment. But she insisted that she would not. “The Lord is taking care of me,” she said. “Dialysis is not in my future at all.”
Credit: The New York Times
Beat the bloat: 5 easy dietitian-approved tips to keep you feeling light and free
Team Metabolic Health
Feeling bloated can be a real downer, but you don’t have to put up with it. We’ve rounded up five easy, dietitian-approved tips to help you beat the bloat.
Ever had that “why did I eat so much?” moment when your belly feels like it’s about to burst? Bloating can totally ruin your day, leaving you feeling heavy and sluggish. And you’re not alone—nearly one in seven Americans experience this every week, according to a 2023 study published in Clinical Gastroenterology and Hepatology. That uncomfortable, tight feeling often comes with your abdomen swelling up, making you feel even more miserable. But don’t worry, there’s a lot you can do to ease the bloat. Simple lifestyle changes, especially in your diet and exercise habits, can make a huge difference in getting you back to feeling your best.

Check out five tips to reduce bloating and improve digestion according to experts. (Pexels)
Dt. Shubha Dhyani Senior Clinical Dietician, Founder & CEO, Right Diet With Shubha shared with HT Lifestyle five simple dietary tips to help reduce bloating.
1. Eat Smaller, More Frequent Meals
Consuming large meals can overwhelm your digestive system and lead to bloating as your stomach struggles to process the large volume of food. Instead, try eating smaller portions more frequently throughout the day. This approach helps maintain a steady flow of digestive enzymes and reduces the likelihood of overloading your stomach, which can prevent excessive gas and bloating. Aim for about five to six smaller meals rather than three large ones.
2. Reduce High-Fiber Foods Gradually
Fibre is essential for digestion and overall health, but an abrupt increase can lead to bloating and gas. High-fiber foods such as beans, lentils, and whole grains are known to cause bloating because they ferment in the gut, producing gas. To minimize this effect, gradually increase your fibre intake to allow your digestive system to adapt. Additionally, soaking beans and cooking them thoroughly can help reduce their bloating potential.
3. Limit Salt and Processed Foods
Excess salt can cause your body to retain water, leading to bloating and swelling. Processed and packaged foods are often high in sodium, so it’s beneficial to limit their consumption. Instead, focus on fresh, whole foods and use herbs and spices to flavour your meals. Reducing sodium intake helps manage fluid balance and can reduce bloating associated with water retention.
4. Stay Hydrated and Avoid Carbonated Beverages
Drinking plenty of water is crucial for digestion and can help reduce bloating by flushing excess sodium and waste from your system. On the other hand, carbonated beverages like soda can introduce extra gas into your digestive tract, leading to bloating. Opt for still water or herbal teas instead. Staying well-hydrated also supports healthy digestion and reduces the risk of constipation, which can contribute to bloating.
5. Incorporate Probiotics into Your Diet
Probiotics are beneficial bacteria that help maintain a healthy balance of gut flora. An imbalance in gut bacteria can lead to bloating and discomfort. Including probiotic-rich foods, such as yoghurt, kefir, sauerkraut, or kimchi, in your diet can improve digestion and reduce bloating. These foods help promote a healthy gut microbiome, which supports more efficient digestion and can alleviate bloating caused by digestive disturbances.
Following these tips can effectively manage and reduce bloating, leading to greater comfort and overall digestive health.
Credit: Hindustan Times
7 tips for parents to reduce child’s screen time as it could be leading to obesity, poor grades
Team Metabolic Health
Too much screen time could be turning your child into a zombie. Check out these 7 practical tips for parents on how to stop it
Excessive screen time can impact the child’s physical and mental well-being by impacting their sleep, mood, concentration and academic performance. We must understand how excessive screen time can take a toll on the child’s overall well-being, so we got an expert on board to roll out some practical tips for parents to regulate the screen time of their child.

7 tips for parents to reduce child’s screen time as it could be leading to obesity, poor grades (Photo by Today’s Parent)
In an interview with HT Lifestyle, Dr Anish Pillai, Lead Consultant – Neonatology and Paediatrics at Motherhood Hospitals in Kharghar, Mumbai, shared, “In today’s digitalised world, everyone is relying on smart gadgets, compared to traditional alternatives. From cookbooks to YouTube recipes, outdoor games to video games, meeting friends to online chatting, society is rapidly changing. Right from a young age, children are exposed to mobile phones, television, or tablets, to keep them engaged while eating or playing.”
He added, “These electronic devices provide respite to parents who are often busy with office work or household chores. However, this can increase their dependence on these devices and make them habituated. Children are more likely to mimic what they see, which is why most of their behavioural pattern is interlinked with the type of content they see. Excessive screen time can negatively impact their physical and psychological health.”
The following are some negative effects of excessive screen time in children –
Reduced attention span: Prolonged exposure to electronic devices can negatively affect attention span. This can cause side effects like difficulty in focusing on one task for a longer period, constantly being restless and fidgety, and trouble paying attention in class or while doing homework. That is because the content online often contains fast-paced images or scenes and a lot of exciting stuff all at once, resulting in constant brain stimulation. This is why kids often find slow-paced activities like reading or writing that require patience and focus as boring.
Poor academic performance: Your kids might often struggle to complete a single task without someone’s help. The key to keeping your kid’s brain active and sharp is learning new things and using logical reasoning to solve problems. When your child is busy engaging in watching online videos and games, they are constantly missing out on fun and brain-stimulating activities like chitchatting with others, playing games, or reading.
Obesity: Glued to an electronic screen for a prolonged period can limit one’s mobility. Sitting in one place for longer hours without taking a break can lead to sudden weight gain. This screen time is often accompanied by unhealthy snacks and treats that can significantly increase their calorie intake. Excessive weight gain can increase the risk of diabetes, heart disease, and high cholesterol levels.
Reduced social skills: In this ever-evolving digitalized era, kids have potentially forgotten the concept of socializing. They are often seen binge-watching videos on tabs or phones while attending social gatherings or parties. It becomes quite challenging for them to interact with others, meet new people, and make friends resulting in isolation and loneliness in the real world.
Practical tips to reduce screen time
- Encourage children to play outdoors with their friends to develop their cognitive skills.
- Use screen time for educational purposes, research, puzzles, and games for collective experience.
- Be attentive to the content your kid is watching. Ensure that you choose age-appropriate videos or games that help in improving their critical thinking.
- The American Academy of Pediatrics (AAP) recommends no more than 1 hour of screen time per day for children aged 2 to 5 and similar limits for older children.
- Parents should make strict rules by keeping electronic screens out of their dinner time, bedroom, and family time to create a healthy space for interaction and family bonding.
- Plan family outings to amusement parks, museums, libraries, and theatres to keep children engaged and involved instead of being glued to their smartphones.
- Parents should demonstrate healthy screen habits by limiting their own screen time and engaging in non-screen activities.
Credit: Hindustan Times
Diabetes medications might prevent memory loss and dementia? Here’s what your parents should know
Team Metabolic Health
Could your diabetes medicine protect you from dementia? New study suggests yes. These are the common type 2 diabetes meds that might protect against memory loss
Certain types of medicines used to treat type 2 diabetes might help to prevent some cases of dementia, according to new research that builds on previous evidence suggesting these drugs might be useful in countering debilitating diseases associated with memory loss and cognition.
New hope: These diabetes medications might prevent memory loss and dementia (Photo by Shutterstock)
Scientists found there was a 35% reduced risk of dementia associated with a class of drugs that includes AstraZeneca Plc’s Forxiga and Boehringer Ingelheim GmbH’s Jardiance, which are called sodium glucose cotransporter 2 inhibitors. They were compared with so-called dipeptidyl peptidase-4 inhibitors, a category that includes Novartis’s Galvus and Johnson & Johnson’s Invokana.
The study, using data from South Korea’s national health insurance database, was published in the British Medical Journal. It found that alongside a potential reduced risk for dementia associated with SGLT2 inhibitors, there was also a 39% reduced risk for Alzheimer’s disease and a 52% reduction in the risk for vascular dementia.
Because the study was only observational, it cannot ascertain cause and effect between the drug and the impact on dementia risk. The scientists have called for clinical trials to now be carried out to test this theory.
Other studies have also shown that SGLT2 inhibitors appear to be associated with a reduced risk of dementia.
“The mechanism through which these effects take place are unknown but likely relate to either affecting inflammation in the brain, reducing the risk for cerebrovascular events or modulating glucose metabolism in the brain,” said Ivan Koychev, senior clinical researcher at Dementia Platform UK, which is based at the University of Oxford. Re-purposing existing drugs for new indications also “reduces greatly the risk of the drug failing through safety concerns,” said Koychev.
Credit: Bloomberg
Gen-Z wellness revolution: Secret behind why they are spending big on beauty and health
Team Metabolic Health
Gen-Z’s obsession with health and beauty: Know the secret to confidence and success of the ultimate wellness warriors
Gen-Z is a very special generation in so many ways and their outlook towards health, beauty, wellness and finance is way different from other generations. They have a certain independence and awareness about what matters to them.

Gen-Z wellness revolution: Secret behind why they are spending big on beauty and health (Photo by Metro Parent)
McKinsey’s latest Future of Wellness research shows that Gen-Z is more interested in wellness spending that’s focused on appearance and overall health. In an interview with HT Lifestyle, Dr Rashmi Shetty, Board Certified Cosmetic Dermatologist, Owner and Founder of RA Aesthetic and Dermatology Clinic in Mumbai, revealed that every aspect of Gen Z’s life is determined by a need to put their best foot forward – be it in areas of financial independence, relationships, career goals and of course, their appearance and health.
According to her, some of the key reasons for this pivot in the generation are –
1. Evolution of beauty standards:
The concept of beauty is very different in the Gen-Z context. They are very particular about how they look and how they present themselves at work, in social gatherings or at parties. With all the information available, they are a curious generation that’s eager to know what goes inside their products, the sustainable choices they have whether in the skincare they choose or the makeup they use.
2. Onset of social media:
Gen Z have been a part of the social media boom and have seen the growth of Instagram, TikTok and other platforms. They value authenticity, real reviews and advice from influencers. They actually interact with brands on social media to raise concerns or resolve their challenges. It’s not a generation that’s submissive or laid back. They are highly motivated and make choices that keep themselves before other things. The visual-heavy medium is helping them look their best with all the guidance they have in doctors, experts, bloggers sharing information.
3. Witnessing a pandemic:
Gen Z has witnessed a catastrophic pandemic in their formative years. This has actually shifted their focus and made them more conscious of health and wellness. Covid-19 shaped them in many ways. It made them define their priorities and enabled them to take care of themselves physically, emotionally and financially.
4. Having an urge to excel:
Gen-Z are exposed to thousands of success stories, be it celebs or startup founders. They have a vision for themselves and are extremely self-aware. Excelling at whatever they pursue is the goal to success and not merely doing something to earn a living. They value the importance of impact and the consequences of their actions. This encourages them to choose best and look best at all phases and stages of their lives.
5. Having financial freedom:
This generation knows how to make money and how to use it constructively. They are not dependent on their life choices or decisions. They research, ask questions and prioritise the way they are perceived by the world. They are open to beauty treatments, skincare routines and sustainable skincare trends that make them look better and feel better.
Gen-Zers are clear, decisive and financially independent. They are unapologetic in the way they want to look. If they want to do their lips or colour their hair blue, they get it done. Unlike the previous generations they are not worried about what others would say. They are very financially independent and have a lot of financial freedom at hand.
How they perceive life is a summation of their experiences and observations of the world. That has played an integral role in their lifestyle choices and decisions. Studies have also shown their inclination towards things that were never centrestage for the other generations.
Just like how mental health is slowly being accepted and adopted, vanity is not looked down upon. The Gen-Z are open to taking care of their looks and even recommending their dermatologists openly. They take a lot of pride in pampering themselves and don’t shy away from putting their most beautiful self forward.
Credit: Hindustan Times
