Diabetes and obesity can damage the liver to the point of failure – but few people know their risk of developing liver disease
Team Metabolic Health
Liver disease is frighteningly common worldwide.
Metabolic dysfunction-associated steatotic liver disease, or MASLD, is an umbrella term describing conditions related to a buildup of fat in the liver. Formerly known as nonalcoholic fatty liver disease, this condition affects 1 in 4 people worldwide. Among those with type 2 diabetes, insulin resistance, obesity or all three, the prevalence of MASLD increases to 3 in 4 people.
As a diabetologist, the possibility of liver disease is on my mind every time I see a patient. Understanding your risk of developing this common yet underrecognized condition is essential to treating it.
What is MASLD?
MASLD is a complex disorder with both environmental and genetic contributions. In its early stages, liver cells accumulate fat in a process called steatosis. Major sources of this fat include adipose tissue as well as fatty acids the liver makes in response to insulin resistance and excess caloric intake. This fat accumulation can enlarge the liver and interfere with its normal functioning.
Over time, fatty acids activate enzymes, which can produce toxic byproducts capable of causing liver cell injury, inflammation and scarring. This condition is better known as MASH, or metabolic dysfunction-associated steatohepatitis. Progression to MASH is more common in the presence of other risk factors such as type 2 diabetes, insulin resistance and metabolic syndrome.
Left unaddressed, MASLD and MASH can progress to liver scarring, failure and, in some cases, cancer. They also increase risk of death from cardiovascular disease and liver-related complications.
In the U.S., MASH is the leading cause of liver transplants due to hepatic cancer among women and in those 65 and older. It is also on track to overtake hepatitis B and C as the main reason people develop liver cancer and thus need a liver transplant.
Liver disease and type 2 diabetes
Three out of four people with type 2 diabetes have MASLD. Linking liver disease, type 2 diabetes and obesity is the key role insulin resistance plays in their genesis.
Obesity is associated with increased fat deposits around the internal organs and higher levels of fatty acids delivered to the liver. Accumulation of fat in the liver increases its resistance to insulin.
Normally, insulin suppresses glucose production in the liver when blood sugar is high. When the liver becomes resistant to insulin, it produces more glucose despite elevated blood sugar levels, which in turn contributes to the development of type 2 diabetes.
A 2015 meta-analysis found that people with MASLD have a nearly twofold greater risk of developing type 2 diabetes than those without the disease. MASLD is also more likely to progress to MASH in the presence of type 2 diabetes.
MASLD disproportionately affects certain ethnic groups. For instance, 1 in 5 people of Hispanic descent in the U.S. have MASLD, with or without diabetes. This is thought to be related to genetic mutations that affect how the liver cells process fat. One particular mutation more common in Hispanic people promotes steatosis by interfering with the cells’ ability to clear fat deposits.
Treating MASLD and MASH
The silver lining is that management of obesity and type 2 diabetes – such as through lifestyle changes – is very similar to management of MASLD. The most critical early interventions for type 2 diabetes can also help with MASLD, and this is not surprising given how closely interrelated these two conditions are.
The best way to reverse the early stages of MASLD is with weight loss through healthy eating habits and regular exercise. The aim is to shed at least 5% to 10% of initial body weight, maintain that weight loss through sustainable and realistic lifestyle choices, and avoid excess alcohol intake to limit additional liver injury.
New medications to treat diabetes, such as GLP-1 receptor agonists like Ozempic and Mounjaro, as well as SGLT2 inhibitors like Jardiance or Invokana, have also shown benefit in early stages of MASLD. These drugs promote weight loss, which in turn improves MASLD. In addition, studies have shown that Ozempic and Mounjaro could reverse MASH, even with inflammation and fibrosis.
Older medications used for diabetes, such as pioglitazone, typically can also help reduce the progression of MASH by reducing insulin resistance.
Liver disease progresses in stages of increasing damage.
In people with severe obesity or who have not had success with lifestyle changes and weight loss drugs, bariatric surgery is another highly effective option to treat MASLD, as it is associated with significant and sustained weight loss.
New drugs are also in the pipeline. The Food and Drug Administration recently approved a new medication called resmetirom to treat MASH with advanced liver scarring.
However, a cure for this chronic disease remains elusive. This is why it is essential to diagnose MASLD as early as possible and use proven measures that can be maintained long term. Treatments and lifestyle changes need to be deployed as early as possible, before inflammation and scarring have firmly set in. MASH gets trickier to treat in more advanced stages when liver damage becomes irreversible. For instance, while Ozempic may help treat early MASH, it doesn’t benefit patients with more advanced stages of liver scarring.
Ignorance is not bliss
Very few people are aware of MASLD and its health implications, including those living with it. While roughly over 35% of U.S. adults have MASLD, less than 5% are aware they have liver disease.
MASH can be difficult to diagnose because it either causes no symptoms or can be mistaken for other conditions. Patients may have the condition for years and not be aware that it is slowly and meticulously causing damage. In that sense, MASH is strikingly similar to type 2 diabetes or high cholesterol.
Young people are increasingly being diagnosed with early-onset MASLD. Indeed, MASLD with MASH is the most common pediatric liver condition, affecting nearly 8% of children and adolescents and over 34% of children with obesity in the U.S. These children and adolescents are at high risk of developing type 2 diabetes and have a significantly increased lifetime risk of cardiovascular disease and cancer.
Health care costs for people with type 2 diabetes and MASH are estimated to reach US$55 billion over the next 20 years, accounting for 65,000 liver transplants, 1.37 million cardiovascular-related deaths and 812,000 liver-related deaths.
These grim statistics need not be if MASH is tackled early and aggressively.
If you are one of the millions of Americans with prediabetes or diabetes and are also overweight, you most likely have some degree of MASLD or MASH. Being aware of MASLD and getting checked is the first step to addressing it.
Promptly determining the best way to treat your MASLD or MASH is the next step. An early referral to a liver specialist will help you halt the progression of this challenging and common condition and take advantage of the treatment breakthroughs researchers have made in the past few years.
Credit: theconversation.com
New research demonstrates potential for increasing effectiveness of popular diabetes, weight-loss drugs
Team Metabolic Health
A network of proteins found in the central nervous system could be harnessed to increase the effectiveness and reduce the side effects of popular diabetes and weight-loss drugs, according to new research from the University of Michigan.
The study, appearing today in the Journal of Clinical Investigation, focused on two proteins called melanocortin 3 and melanocortin 4, found primarily on the surface of neurons in the brain, that play a central role in regulating feeding behavior and maintaining the body’s energy balance.
Melanocortin 3 and melanocortin 4 impact everything from sensing long-term energy stores to processing signals from the gut regarding short-term fullness, or satiety, said U-M physiologist Roger Cone, who led the study.
The drugs known as GLP-1 agonists, which include semaglutides (e.g., Ozempic) and tirzepatides (e.g., Mounjaro), have received substantial attention recently for their effectiveness in treating not only type 2 diabetes, but also obesity, heart disease and potentially addiction. They work by mimicking a natural hormone that the gut produces when it is full, triggering the brain to reduce feeding behavior.
“So the obvious question for us was: How do these GLP-1 drugs, which work by manipulating satiety signals, function when we prime the melanocortin system?” said Cone, professor of molecular and integrative physiology at the U-M Medical School and director of the U-M Life Sciences Institute, where his lab is located.
Working in mouse models, Cone and his colleagues tested the effects of several hormones that reduce food intake. They compared the results in normal mice with mice that genetically lacked the MC3R protein, in mice that were given chemicals to block the activity of MC3R, and in mice that were given a drug to increase the activity of MC4R. (Because MC3R is a natural negative regulator of MC4R, meaning it decreases the activity of MC4R, blocking MC3R and increasing MC4R activity has similar effects.)
In all cases, Naima Dahir, first author of the study and a postdoctoral research fellow in Cone’s lab, and colleagues found that adjusting the melanocortin system—either by inhibiting MC3R or increasing MC4R activity—made the mice more sensitive to GLP-1 drugs and other hormones that affect feeding behavior. The mice that were given a GLP-1 drug in combination with an MC4R agonist or MC3R antagonist showed up to five times more weight loss and reduced feeding than mice receiving only the GLP-1 drugs.
“We found that activating the central melanocortin system hypersensitizes animals to the effects of not just GLP-1s, but to every anti-feeding hormone we tested,” Cone said.
The researchers also measured activity in parts of the brain thought to trigger nausea in response to GLP-1 drugs and observed no increased activation when GLP-1 drugs were combined with alterations to the melanocortin system. In contrast, priming of the melanocortin neurons significantly increased GLP-1 drug activation of neurons in hypothalamic feeding centers in the brain.
The findings indicate that pairing the existing GLP-1 drugs with an MC4R agonist could increase sensitivity to the desired effects of the drugs by up to fivefold, without increasing unwanted side effects. Ultimately, this approach could enable patients who are sensitive to the side effects to take a lower dose, or could improve the results in patients who have not responded to the existing drug dosages. Further drug development and clinical testing are needed before this can occur.
While this research has been conducted only in mouse models, Cone is optimistic that the results will translate well to humans.
“The melanocortin system is highly conserved in humans,” he said. “Everything we’ve observed in the mouse over the past decades studying these proteins has also been found in humans, so I suspect that these results would also be translatable to patients.”
In addition to Cone and Dahir, the study authors include Yijun Gui, Yanan Wu, Alix Rouault, Savannah Williams, Luis Gimenez, Stephen Joy and Anna K. Mapp, University of Michigan; Patrick Sweeney, University of Illinois; and Tomi Sawyer, Courage Therapeutics.
Credit: Medical Xpress
Popular weight-loss and diabetes medications show promise for curbing smoking, study suggests
Team Metabolic Health
A growing set of evidence suggests that using semaglutide could lead to decreased substance use, and a large new study shows a promising link between the medication and tobacco use. But experts emphasize that much more research is needed before using the medications off-label for smoking cessation.

A new study suggests that there’s a link between semaglutide use and lower rates of treatment for tobacco use disorder among people with type 2 diabetes. (Pix Credit: AP/File)
In a study published Monday in the journal Annals of Internal Medicine, researchers tracked the medical records of more than 200,000 people who started medications to treat type 2 diabetes, including nearly 6,000 people using semaglutide medications such as Ozempic.
Over the course of a year, people who started using semaglutide were significantly less likely to have medical encounters for tobacco use disorders, prescriptions for medications for smoking cessation or counseling for smoking cessation than those who started other diabetes medications such as insulin and metformin.
The study authors note that the reasons individuals might be less likely to seek medical treatment for tobacco use disorder vary widely; it could suggest that their tobacco use decreased or that they’ve become less willing to seek help to quit smoking, for example.
There might be a mix of medication-driven and patient-driven change, said Dr. Disha Narang, an endocrinologist and director of obesity medicine at Endeavor Health in Chicago, who was not involved in the new research.
“If I have a patient with type 2 diabetes who is on one of these agents and they do have a history of smoking, oftentimes, our visits involve a conversation about tobacco cessation,” she said. “These folks might start paying special attention to their long-term health and changing some habits because they are being treated for diabetes.”
Also, the new study did not measure the severity of tobacco use, such as the number of cigarettes consumed per day, cravings or withdrawal.
Understanding how semaglutide affects these factors is “crucial” to determining whether the medications could be used for smoking cessation, said Dr. Nora Volkow, director of the National Institute on Drug Abuse and a co-author of the new report. Also, more work would be needed to understand appropriate dosage and adverse effects before using the blockbuster drugs in new way, she said.
But other early research suggests that semaglutide and other GLP-1 medications could interact with the brain’s reward system in a way that helps modulate cravings, whether for food, nicotine, alcohol or other drugs.
“The main driver of why many of us overeat relates to those reinforcing positive responses that we get from eating certain foods. And it’s the same circuit for foods as for drugs,” Volkow said.
Although key questions remain, Volkow said she is struck by how consistent the findings have been when it comes to the relationship between semaglutide use and decreased substance use – across different substances and among different patient groups. The new study found similar links among those with and without obesity.
“A signal like this one cannot be ignored, particularly because of how consequential it could be if, in fact, we can have now a new medication for treating smoking cessation,” she said. “That could have a tremendous impact on health.”
Smoking rates in the United States have decreased over time, but cigarette smoking remains the leading cause of preventable disease and death, according to the US Centers for Disease Control and Prevention. A recent study from the American Cancer Society found that smoking contributes to nearly 1 in 5 new cancer cases and nearly a third of cancer deaths each year.
But fewer than 1 in 10 adult cigarette smokers succeed in quitting each year, according to the new study, and options for smoking cessation treatment haven’t changed much in decades.
Credit: CNN
You’ve Lost Weight Taking New Obesity Drugs. What Happens if You Stop?
Team Metabolic Health
Many patients are eager to discontinue Wegovy or Zepbound when their weight loss plateaus. But doctors say it’s difficult to go cold turkey.
Susana Parks was delighted when she lost 40 pounds on Eli Lilly’s obesity drug, Zepbound. But now that she is at her goal weight, she has questions: Can she stop taking the drug? And if she does, how can she maintain her weight loss?
“I can’t stop cold turkey or I will gain it back — that is clear,” said Ms. Parks, 60, of Bend, Ore. “Do I go to a lower dosage? Do I take it every two weeks instead of weekly? How do I maintain?”
These questions are becoming common, obesity medicine specialists say, as more and more people lose weight with obesity drugs. Some struggle to pay for the medicine, have difficulty finding it to purchase or just don’t want to stay on a drug longer than they believe they need to.
When doctors are confronted with these queries, here is what they advise — and what they can’t say.
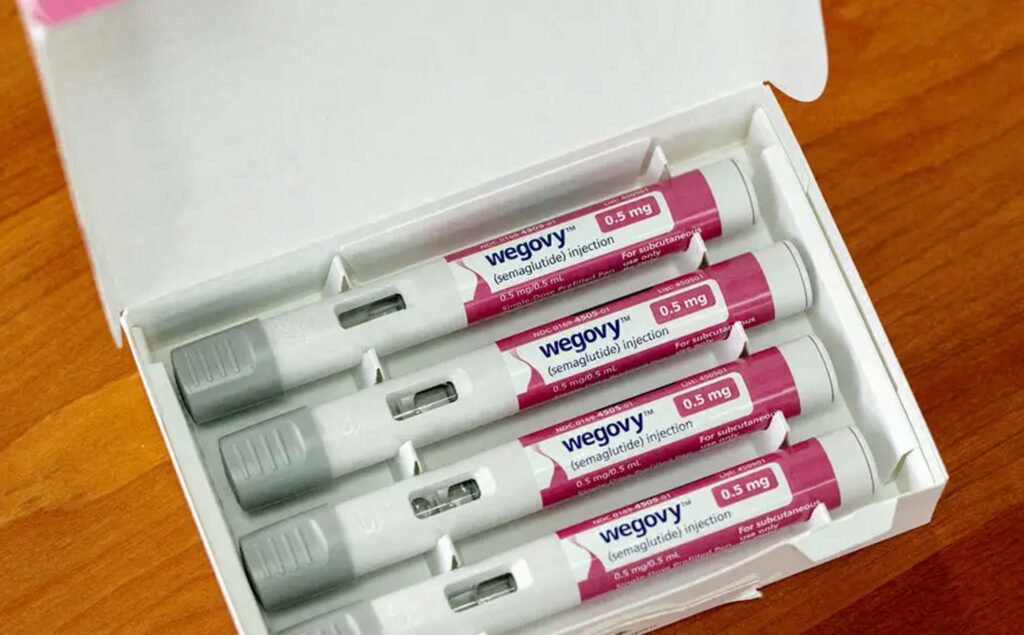
(Image Credit: Reuters)
What will happen if I stop taking the new weight-loss drugs after losing weight?
Dr. David Cummings, a weight-loss specialist at the University of Washington, has been asked this question by many patients. He explains that the makers of the drugs conducted large studies in which people took the drugs and then stopped.
“On average, everyone’s weight rapidly returned,” Dr. Cummings said. And, he said, other medical conditions, like elevated blood sugar and lipid levels, return to their previous levels after improving.
He also tells patients that while on average, weight is regained when the drugs are stopped, individuals vary in how much weight and how quickly it returns.
Hearing that, Dr. Cummings said, some patients want to take a chance that they will not need the drugs once they lose enough weight. He says some tell him, “I will be the one. I just need some help to get the weight off.”
So far, though, Dr. Cummings has not seen patients who have succeeded.
Will lowering my dose help me keep the weight off?
Doctors say they have no data to guide an answer to that question.
It “has not been studied in a systematic fashion,” said Allison Schneider, a spokeswoman for Novo Nordisk, the maker of Wegovy. The drug is based on the medication semaglutide, which the company also sells for diabetes treatment as Ozempic.
The same is true for tirzepatide, which Eli Lilly sells as Zepbound for weight loss and Mounjaro for diabetes.
When doctors do offer advice, it tends to be tentative.
“There is no magic bullet,” said Dr. Mitchell A. Lazar of the University of Pennsylvania’s Perelman School of Medicine.
What might happen if I experiment with my dose?
Ms. Parks said she was not interested in continuing to lose weight. For her, a 40-pound weight loss was perfect.
She’s grateful she got Zepbound — her doctor, she said, resisted prescribing it, her insurance would not pay for it and the drug was in such short supply that she called pharmacy after pharmacy each month to refill her prescription, paying out of pocket each time.
While Dr. Lazar does not treat Ms. Parks, when he heard about her case, he said she could try reducing her dose.
Or, he said, “she can monitor what she is eating now and do her best to eat the same amounts after she lowers or stops her dose.”
But, he added, that may be difficult without the help of the drug.
For the moment, Ms. Parks is adjusting her dose. When her weight fell to 150 pounds — she’s 5 feet 8 inches tall — she decided to try taking Zepbound every other week, instead of every week. She told her doctor what she was doing. Her doctor, Ms. Parks said, “had no opinion one way or another.”
Her new dosing schedule, Ms. Parks added, also saves her money.
After a week without the drug, she said, she gets hungry. It happens every time, predictably. Then she takes her next dose.
So far it is working — her weight has been steady.
Dr. Caroline Apovian, a weight-loss specialist at Brigham and Women’s Hospital, said there’s a lesson here for people struggling with their weight.
“It teaches patients that it’s really not under your control,” said Dr. Apovian, who used to consult for Novo Nordisk.
Does that mean I have to take Wegovy or Zepbound forever?
“Most patients want to lose as much as they can but don’t want to be stuck on the medicine for the rest of their lives,” Dr. Cummings said. “The most common question is, ‘How long do I have to take it?’”
“The proper answer is probably forever,” he said.
Some patients tell Dr. Cummings it sounds like he is giving them a life sentence, and others simply do not believe him.
In a study of electronic health records by Truveta, a health care data company, more than half of patients without diabetes stopped taking the drugs within a year. But about a third who stopped restarted.
Faced with these concerns, doctors stress that obesity is a chronic disease and, like high blood pressure and other chronic diseases, must be treated for life. But beliefs persist that obesity is different from a disease like high blood pressure — the perception is that weight can be controlled by lifestyle and willpower.
Is there any risk of losing too much weight on the drugs?
Patients also want to know if they risk losing weight indefinitely, becoming dangerously thin.
Unlikely, obesity medicine experts said.
Eventually, with the new weight loss drugs, patients reach a plateau where they stop losing weight.
Ms. Schneider of Novo Nordisk said that in the Wegovy trials, weight loss stopped after about 60 weeks.
When that happens, said Dr. Ania Jastreboff of Yale, who is on advisory boards for Novo Nordisk and Eli Lilly, hunger returns. So do food cravings, even though patients are still taking the drugs. But the person will naturally eat only enough to maintain the lower weight.
Do side effects return if people stop and then restart the drugs?
Many describe experiencing side effects like nausea and vomiting when they first start taking Wegovy or Zepbound. For most, but not all, patients, the side effects diminish as they adjust to the drugs.
But, Dr. Apovian warned, those side effects may return if patients stop and then restart the drugs. The longer they are off the drug, she added, the more likely it is that the side effects will return.
Credit: The New York Times
Here’s the real reason Ozempic-like weight-loss drugs are so popular
Team Metabolic Health
Overweight and obesity rates have reached crisis levels and are risk factors for diabetes, heart disease, cancer, dementia, and other diseases.
The CDC estimates that that almost a third of Americans are now overweight and 42% of adults “have obesity,” now categorized as a disease. Childhood obesity is up—one in five kids are estimated to be affected.
This isn’t just an American crisis. The World Obesity Federation predicts that 51% of the world’s population will be overweight or obese within the next 12 years.
Causes include sedentary lifestyles, as more people work and play in front of computer screens, the food and beverage environment, eating more out of home, fewer safe places for physical activity, genetics, and taking certain medications.
The new generation of weight-loss drugs may be attracting cohorts that were unresponsive to strategies such as portion control. (Bloomberg/Getty Images)
GLP 1 drugs in action
Along have come new, highly popular GLP 1 weight loss drugs, including Ozempic, Wegovy, and Mounjaro. Oprah Winfrey did a TV special: Shame, Blame and the Weight Loss Revolution. After years of up and down weight, Oprah says it’s not your fault: Obesity is a disease. She’s losing weight on one of the new drugs and helping move the market. However, insurance coverage, including Medicare, will have the biggest impact on usage.
Brian Kay of Numerator, a research firm, reports that some 12% of respondents in their household panel are using one of the new GLP 1 drugs for diabetes and/or weight loss. About 75% say they are consuming smaller portion sizes and – based on Numerator’s purchase data – their grocery bills are down 6 to 9%. Alcohol and ice cream purchases have decreased while fish and yogurt are up. However, the main reason consumers report discontinuing the drug is cost – and then grocery spending returns to previous levels.
All this has major financial implications for the food and beverage industries, restaurants, food service operators, health insurance companies, and Medicare. And the total cost in health care, lost productivity, corporate insurance, and long-term care is enormous.
How we got here
In recent decades, food consumption has increased dramatically. The portion sizes for bagels, cheeseburgers, ice cream, restaurant servings of spaghetti, meatballs, and more are ever larger.
Many restaurant chains compete on volume meals, and consumers often equate volume with value. One result is considerable waste. ReFED, a research group, estimated that 70% of food wasted in restaurants is left on plates.
The journal Addiction describes “hyper-palatable foods” as a kind of food engineering in which fat, sodium, sugar, and other additives can also drive people to crave and overeat. Northeastern University’s Network Science Institute indicates that 73% of the U.S. food supply is ultra-processed.
Getting consumers to change their behavior is a tall order. Many are confused, misguided, or indifferent about eating healthier.
A Navy officer once told me about the difficulty of re-enlisting highly trained non-commissioned officers who became too heavy to meet Body Mass Index guidelines. “We make ‘em taller. You’d be surprised how many 5’10” guys are now 6’2”—at least on paper.”
A decade ago, the McKinsey Global Institute found that portion control was the most promising strategy for promoting a healthier lifestyle. In response, the Portion Balance Coalition (PBC) was formed as an alliance of major food and beverage companies, nonprofits, academics, and government to reduce obesity and improve health. It is led by the Business for Impact Center at Georgetown University.
Credit: fortune.com
Weight loss drugs could be used to treat other life-threatening issues: Study
Team Metabolic Health
Drugs like Ozempic, Wegovy, and Zepbound are reshaping treatment for obesity and diabetes, and their benefits might extend further. Emerging research suggests that GLP-1 drugs could also help manage addiction, sleep apnea and even cancer.
These medications, which regulate hormones, slow digestion and reduce hunger, are showing promise in preventing cancers linked to obesity, such as breast, colon, liver, and ovarian cancers, according to research from the American Society of Clinical Oncology (ASCO).
Dr. Arif Kamal, the chief patient officers at the American Cancer Society, noted that GLP-1 drugs might significantly lower cancer risks and provide better protection for diabetics compared to insulin.
The ASCO research found that GLP-1 drugs could cut the risk of obesity-related cancers by 39%, compared to 22% with bariatric surgery over 10 years. Originally designed for diabetes, these drugs are now also approved for weight loss under names like Saxenda, Wegovy and Zepbound.
The link between obesity and cancer is complex, involving hormones like estrogen, which is elevated in fat cells and drives cancer growth. Kamal compared obesity’s impact on cancer to tobacco’s historical effect, emphasizing the significance of GLP-1 drugs in reducing cancer risk.
Cindy Lin, the co-author of the study, pointed out that GLP-1 drugs might offer protective effects beyond weight loss, including better glycemic control and anti-inflammatory benefits.
Credit: Straight Arrow News (SAN)
Weight-loss drugs like Wegovy may help stave off some cancers
Team Metabolic Health
Drugs like Ozempic, Wegovy and Zepbound have transformed treatment for obesity and diabetes. Now researchers are excited about their potential impact on other conditions, including addiction and sleep apnea — and even cancer.
Scientists see this class of drugs, called GLP-1 agonists, as a breakthrough because of how they act on the brain to regulate the body’s hormones, slow digestion, and tamp down hunger. And in several recent studies, they show early promise in preventing many common cancers — including breast, colon, liver, and ovarian — known to be driven by obesity and excess weight.
“It’s a hopeful story, which is, frankly, what people need,” says Arif Kamal, an oncologist specializing in breast cancer as well as chief patient officer at the American Cancer Society.
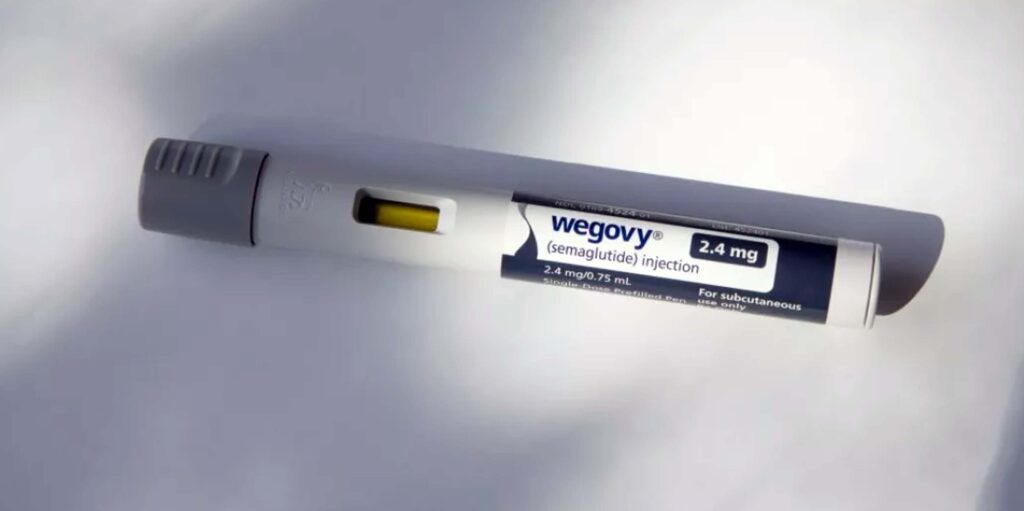
GLP-1 drugs, like Wegovy and Ozempic, may not be good only for diabetes and weight-loss. They are also showing promise for preventing some cancers. (UCG/Universal Images Group/Getty Images)
Though research on GLP-1 drugs is still in its relative infancy, so far studies fairly consistently show their benefit in staving off certain cancers. One research letter published in JAMA Oncology last year, for example, suggests GLP-1 drugs might reduce the risk of colon cancer, even among people who are not overweight. A more recent analysis in JAMA Network Open suggests GLP-1s provide far more protection against cancer for diabetic patients than insulin treatments.
Another recent study presented at the American Society of Clinical Oncologists meeting in June, showed both bariatric surgery and GLP-1 medications dramatically reduce the risk of the 13 obesity-related cancers. Among those who had bariatric surgery, that risk declined by 22% over 10 years compared to those who received no treatment. But among those taking GLP1 medications, risk dropped by a whopping 39%.
“And I think a 39% risk reduction is one of the most impactful risk reductions we’ve ever really seen,” says Kamal.
GLP-1 agonist drugs were originally developed to treat diabetes nearly two decades ago. Over the past decade, regulators started approving them as treatments for weight loss – first as liraglutide, sold under the brand Saxenda and, more recently, in the form of semaglutide or tirzepatide, under brands like Wegovy and Zepbound.
When it comes to cancer prevention, scientists are finding the link between obesity in cancer is complex and intertwined; the obesity-related cancers are heavily concentrated among organs involved in digestion and metabolism, like the liver and pancreas, for example, as well as among gynecologic cancers, including breast and uterus. Reproductive organs are highly sensitive to the hormone estrogen, which plays a role in allowing cells to grow rapidly during pregnancy, for example.
But Kamal says there’s also an especially close relationship between estrogen and cancer. “What we do know is that estrogen in particular — and possibly some other hormones, but estrogen for sure — drives the growth of many cancers,” he says. And fat cells increase production of estrogen.
That means women today are increasingly susceptible to cancer. Historically, men faced a much higher risk of developing cancers — in large part because they were more likely to engage in high-risk behaviors like smoking or drinking, Kamal says. But in recent years, the high prevalence of obesity among both men and women is closing that gender gap.
Obesity is also likely the most significant driver behind increasing cancer rates among younger adults, he says, just as tobacco was in generations past.
“Unhealthy weight is the smoking of our generation,” Kamal says.
That’s why indications that GLP-1 drugs may help slash that risk is so significant.
What’s more, that ASCO study suggests that GLP-1 drugs have a notable impact on cancer risk, even when patients don’t lose a lot of weight as a result of taking them. In other words, the medications seem to act on a number of the body’s mechanisms to reduce vulnerabilities to cancer.
“We think the protective effects of GLP-1s are probably multifactorial,” says Cindy Lin, resident physician at Case Western Reserve and co-author of the June ASCO study. “Part of it is weight [loss], but other factors may be contributing as well — better glycemic controls, anti-inflammatory effects.”
More research is necessary and inevitable — especially studies looking at the newer weight-loss formulations of GLP-1 medications, says Benjamin Liu, another resident physician at Case Western and co-author of the ASCO study.
He says he’s encouraged by the data so far. “It’s very exciting to have, especially since it’s more of a noninvasive strategy compared to bariatric surgery, and a lot more patients will be open to it.”
Credit: npr.org
Lilly lifts sales forecast by $3 billion as weight-loss drug powers results
Team Metabolic Health
Eli Lilly raised its annual sales forecast by $3 billion on Thursday, driven by surging demand and ramped up manufacturing capacity for its popular weight-loss drug Zepbound, lifting its shares more than 10% premarket.
The drugmaker also raised its annual profit forecast and said sales of its Zepbound crossed $1 billion for the first time in a quarter. The milestone for Zepbound comes a day after Danish rival Novo Nordisk reported a rare miss on quarterly sales of its weight-loss drug Wegovy and trimmed its full-year profit forecast.
Lilly and Novo are racing to increase manufacturing capacity to meet unprecedented demand for their popular weight-loss drugs that have been shown to help patients lose as much as 20% of their weight on average. It has invested an additional $5.3 billion in May on a manufacturing site in Indiana for production of tirzepatide, the active ingredient in Zepbound, as well as its diabetes drug Mounjaro.
Credit: The Economic Times
Medicine’s Lindsey Wang shares research findings linking weight-loss drugs to a lowered risk of cancer
GLP-1 drugs may lower risk of 10 obesity-related cancers, study shows
Team Metabolic Health
Lindsey Wang, researcher at the School of Medicine, discussed her new research showing that weight-loss drugs, including Ozempic, are linked to a lower risk of cancer. “Most notably, we observed a significant risk reduction across multiple gastrointestinal cancers,” Wang said. “This broad spectrum of effects is significant given the often poor prognosis associated with these cancers.”
Credit: The Daily
Very-low-calorie keto diet slashes fat and oxidative stress, boosting metabolic health in obesity
Team Metabolic Health
Obesity,Oxidative Stress,Stress
Study reveals that an 11-week, very-low-calorie ketogenic diet significantly reduces body fat and improves glucose metabolism in obese individuals, while also lowering oxidative stress markers, indicating better overall metabolic health.
A study published in the journal Free Radical Biology and Medicine demonstrates the impact of a multiphase, very-low-calorie ketogenic diet on serum markers of oxidative stress in individuals living with obesity.
Calorie-restricted diets with high levels of nutraceuticals and phytochemicals have been found to reduce obesity-related complications and increase life expectancy through anti-inflammatory and antioxidant activities. Important observations The analysis of baseline characteristics identified dyslipidemia as the most frequent comorbidity among participants. All of them were physically active; however, their activity levels were low.
Regarding metabolic effects, the intervention was found to improve glucose and lipid metabolism, with no changes in serum total protein and albumin levels. Study significance The study finds that intake of a multiphase, very-low-calorie ketogenic diet for eleven weeks has positive health effects, as demonstrated by reduced body weight and fat mass and improved glucose and lipid metabolism. These positive health effects are associated with reduced serum oxidative stress markers and improved serum redox balance.
Credit: Head Topics (UK)
Gluco6– Is It Right For You?
Team Metabolic Health
Maintaining optimal blood sugar levels is crucial for overall health, especially for those dealing with diabetes or weight management issues. The constant battle against fluctuating glucose levels can leave individuals feeling drained, overweight, and overwhelmed. Fortunately, Gluco6 has emerged as a beacon of hope for those seeking a natural solution to these challenges. This revolutionary product promises to help regulate blood sugar and aid in effective weight loss. With a unique blend of ingredients, Gluco6 aims to address the underlying issues contributing to blood sugar spikes while promoting a healthier lifestyle. This comprehensive review will explore what Gluco6 is, how it works, its key ingredients, benefits, pricing options, testimonials, and much more. By the end of this review, you will have a thorough understanding of Gluco6, allowing you to decide whether this product is the right fit for you.
What is Gluco6?
Gluco6 is a dietary supplement that supports healthy blood sugar levels and assists in weight loss. It leverages a scientifically backed formulation that targets the body’s insulin response and glucose metabolism, providing relief from the complications associated with high blood sugar. Gluco6’s unique approach is centered around addressing an often-overlooked issue known as “GLUT-4 Overwhelm.” This condition occurs when the pancreas is overworked due to high sugar intake and processed carbohydrates, leading to poor insulin sensitivity and blood sugar regulation.
By utilizing a potent blend of Mediterranean plants and supernutrients, Gluco6 helps combat GLUT-4 Overwhelm and promotes the natural balance of blood sugar levels and overall metabolic health. This product is particularly beneficial for individuals who have struggled with weight management, sugar cravings, and energy levels. Gluco6 has gained popularity among health enthusiasts and individuals seeking a practical solution to their blood sugar challenges. Its formulation promises to yield visible results in weeks, making it a compelling option for those looking to enhance their health and well-being.
Does Gluco6 Work?
The effectiveness of Gluco6 stems from its innovative formulation, designed to support the body’s natural processes rather than merely masking the symptoms of blood sugar imbalance. Many users report noticeable improvements in blood sugar levels and weight management after incorporating Gluco6 into their daily routine. The product’s ability to enhance insulin sensitivity and reduce glucose spikes is attributed to its carefully selected ingredients that synergize the body’s metabolic functions.
Clinical studies and user testimonials indicate that consistent use of Gluco6 can substantially improve blood sugar control, with many experiencing less frequent spikes and crashes throughout the day. This stability is crucial for those who are insulin-resistant or struggling with Type 2 diabetes. Furthermore, the product’s ability to curb sugar cravings enhances the weight loss benefits, which often sabotage dietary efforts. Overall, while individual results may vary, the collective feedback strongly suggests that Gluco6 is a viable option for anyone looking to manage their blood sugar levels and achieve their weight loss goals effectively.
Gluco6 Benefits
Improved Blood Sugar Control
One of Gluco6’s hallmark benefits is its ability to maintain stable blood sugar levels. The unique blend of ingredients, including Sukre, chromium, and Gymnema, targets various aspects of glucose metabolism to ensure that blood sugar remains consistent throughout the day. Many individuals experience significant fluctuations in their blood sugar levels, leading to fatigue, irritability, and cravings for sugar-rich foods. Gluco6 addresses these issues by enhancing insulin sensitivity, allowing the body to utilize glucose more effectively.
Users often report that they experience fewer energy crashes and a more stable mood, which is critical for overall well-being. Improved blood sugar control not only helps in the management of diabetes but also supports weight management efforts by minimizing the cravings that often accompany blood sugar spikes and drops. This stability promotes a healthier lifestyle, allowing individuals to make better dietary choices without the constant interference of fluctuating glucose levels.
Effective Weight Loss
Weight loss is a common concern for many individuals battling blood sugar issues, and Gluco6 addresses this need head-on. Enhancing insulin sensitivity and promoting better glucose metabolism helps the body utilize stored fat effectively, leading to weight loss over time. Gluco6’s ingredients work harmoniously to suppress sugar cravings, making it easier for users to adhere to their weight loss goals without the constant temptation of unhealthy snacks.
Moreover, Gluco6’s energizing properties help improve physical activity levels, further supporting weight loss efforts. By combining these effects, Gluco6 provides a multifaceted approach to weight loss that goes beyond fad diets and temporary solutions. Instead, it offers a sustainable method for individuals to achieve and maintain a healthy weight while effectively managing their blood sugar levels.
Reduced Sugar Cravings
One of the most challenging aspects of managing blood sugar levels is overcoming sugar cravings. Gluco6 tackles this issue by incorporating ingredients like gymnema and chromium, which have been shown to effectively reduce the desire for sugary foods. Gymnema, often referred to as the “sugar destroyer,” actively blocks the sweet taste receptors on the tongue, providing immediate relief from cravings.
By addressing the psychological and physiological factors that contribute to sugar cravings, Gluco6 empowers users to make healthier dietary choices. This reduction in cravings not only aids in weight management but also promotes better blood sugar control, creating a positive feedback loop for users. With fewer cravings, individuals can focus on nourishing their bodies with healthier foods that support their overall well-being, making Gluco6 an invaluable ally in the quest for a balanced lifestyle.
Enhanced Energy Levels
Maintaining high energy levels is essential for daily productivity and overall quality of life. Individuals dealing with blood sugar problems often experience fatigue due to spikes and crashes in glucose levels. Gluco6 counteracts this by providing ingredients designed to support sustained energy throughout the day. For instance, TeaCrine enhances cognitive function and mood, ensuring users feel alert and focused.
The product’s ability to stabilize blood sugar levels means that energy levels remain consistent without the drastic fluctuations that can lead to lethargy. Users frequently report feeling more energetic and less tired, enabling them to engage more effectively in physical activities and daily tasks. This renewed vitality is beneficial for physical health and positively influences mental well-being, creating a holistic improvement in lifestyle.
Antioxidant Support
The presence of antioxidants in Gluco6 adds another layer of health benefits to the product. Ingredients like green tea and cinnamon are rich in antioxidants, which help combat oxidative stress in the body. Oxidative stress is linked to various health issues, including inflammation and chronic diseases, making supporting the body’s defenses crucial.
By incorporating antioxidants, Gluco6 helps protect cells from damage caused by free radicals. This protection is significant for individuals with blood sugar imbalances, who are often at greater risk for oxidative stress. Improved antioxidant support can lead to better overall health, aiding recovery and enhancing the body’s natural resilience. This comprehensive approach ensures that users manage their blood sugar levels and bolster their overall health.
Heart Health
Heart health is a significant concern for individuals managing blood sugar levels, as diabetes and high blood sugar can elevate the risk of cardiovascular disease. Gluco6 supports heart health through its carefully selected ingredients, promoting healthy circulation and lowering inflammation. Components like green tea provide cardiovascular benefits by improving lipid profiles and reducing plaque buildup in the arteries.
Additionally, the weight loss benefits associated with Gluco6 can further enhance heart health. As individuals shed excess weight, they often experience lower blood pressure and improved cholesterol levels, reducing the risk of heart-related issues. By prioritizing heart health in its formulation, Gluco6 addresses blood sugar concerns and contributes to a healthier heart, promoting long-term wellness for its users.
Credit: Peninsula Daily News
Research shows our bodies go through rapid changes in our 40s and our 60s
Team Metabolic Health
For many people, reaching their mid-40s may bring unpleasant signs the body isn’t working as well as it once did. Injuries seem to happen more frequently. Muscles may feel weaker.
A new study, published in Nature Aging, shows what may be causing the physical decline. Researchers have found that molecules and microorganisms both inside and outside our bodies are going through dramatic changes, first at about age 44 and then again when we hit 60. Those alterations may be causing significant differences in cardiovascular health and immune function.
The findings come from Stanford scientists who analyzed blood and other biological samples of 108 volunteers ages 25 to 75, who continued to donate samples for several years.
“While it’s obvious that you’re aging throughout your entire life, there are two big periods where things really shift,” said the study’s senior author, Michael Snyder, a professor of genetics and director of the Center for Genomics and Personalized Medicine at Stanford Medicine. For example, “there’s a big shift in the metabolism of lipids when people are in their 40s and in the metabolism of carbohydrates when people are in their 60s.”
Lipids are fatty substances, including LDL, HDL and triglycerides, that perform a host of functions in the body, but they can be harmful if they build up in the blood.
How ‘bio hackers’ are exploring options to reverse aging
The scientists tracked many kinds of molecules in the samples, including RNA and proteins, as well as the participants’ microbiomes.
The metabolic changes the researchers discovered indicate not that people in their 40s are burning calories more slowly but rather that the body is breaking food down differently. The scientists aren’t sure exactly what impact those changes have on health.
Previous research showed that resting energy use, or metabolic rate, didn’t change from ages 20 to 60. The new study’s findings don’t contradict that.
The changes in metabolism affect how the body reacts to alcohol or caffeine, although the health consequences aren’t yet clear. In the case of caffeine, it may result in higher sensitivity.
It’s also not known yet whether the shifts could be linked to lifestyle or behavioral factors. For example, the changes in alcohol metabolism might be because people are drinking more in their mid-40s, Snyder said.
For now, Snyder suggests people in their 40s keep a close eye on their lipids, especially LDL cholesterol.
“If they start going up, people might want to think about taking statins if that’s what their doctor recommends,” he said. Moreover, “knowing there’s a shift in the molecules that affect muscles and skin, you might want to warm up more before exercising so you don’t hurt yourself.”
Until we know better what those changes mean, the best way to deal with them would be to eat healthy foods and to exercise regularly, Snyder said.
Dr. Josef Coresh, founding director of the Optimal Aging Institute at the NYU Grossman School of Medicine, compared the new findings to the invention of the microscope. “The beauty of this type of paper is the level of detail we can see in molecular changes,” said Coresh, a professor of medicine at the school. “But it will take time to sort out what individual changes mean and how we can tailor medications to those changes. We do know that the origins of many diseases happen in midlife when people are in their 40s, though the disease may occur decades later.”
The new study “is an important step forward,” said Dr. Lori Zeltser, a professor of pathology and cell biology at the Columbia University Vagelos College of Physicians and Surgeons. While we don’t know what the consequences of those metabolic changes are yet, “right now, we have to acknowledge that we metabolize food differently in our 40s, and that is something really new.”
The shifts the researchers found might help explain numerous age-related health changes, such as muscle loss, because “your body is breaking down food differently,” Zeltser said.
Credit: NBC News
Eating less of this vitamin can make you live longer, say scientists
Metabolic Health Team
Scientists at Texas A&M AgriLife Research discovered that reduced folate intake could improve metabolism and promote longevity in older adults. Their study found that middle-aged animals on folate-limited diets transitioned better between carbohydrate and fat metabolism, maintained energy levels, and exhibited no adverse health effects, suggesting potential metabolic benefits from reduced folate in later life.
While an excess of vitamins is always harmful, in some cases less of it may be more beneficial. The same applies to folate intake, as scientists in a recent research found eating less of it could bring more benefits in older adults.
Among the factors that play a huge role in slowing down the ageing process, diet plays an important role. Adding the right foods to your diet with the right mix of proteins, carbohydrates, vitamins, minerals and fibre has an anti-ageing effect.
However, when it comes to choosing foods for healthy ageing, one must also stay updated on latest research.
Role of folate in overall health
In a recent study published in Life Science Alliance, scientists from Texas A&M AgriLife Research discovered that eating less folate is linked to healthy metabolism in aging animal models. Folate or folic acid found in dark green leafy vegetables, orange, lemon, melons, nuts and seeds, and pea among other foods, is crucial for red blood cell formation and healthy cell growth and function. It is particularly important for children, young adults, and pregnant women as it plays an important role in growth processes.
Folic acid supplementation is considered important before and throughout pregnancy. It is important for development of foetus. According to research, folic acid supplements taken before to conception may help reduce birth abnormalities, including significant neural tube disorders like spina bifida, encephalocele, and anencephaly. Prenatal vitamins with 400 micrograms (mcg) of folic acid can help prevent brain and spinal cord birth abnormalities.
Cutting folate could boost longevity in older adults
In this study, researchers sought to study the impact of cutting folate intake in lesser-studied age groups. Researchers cut folate from diet of animal models at an age corresponding to human middle age. Another group continued with a diet inclusive of folate.
It was found that the female folate-limited models were able to transition more quickly between carbohydrate metabolism and fat metabolism across night and day compared to females on folate-rich diet.
“Optimal folate intake may vary depending on an individual’s age. While higher folate is crucial during early life for growth and development, a lower intake later in life may benefit metabolic health and longevity,” said Michael Polymenis, Ph.D., professor and associate head of graduate programs in the Texas A&M College of Agriculture and Life Sciences Department of Biochemistry and Biophysics, who led the study. Polymenis said that when one sleeps, their metabolism burns fat while when awake and active, carbohydrates are burnt for quicker energy. However when one gets older, it takes “longer to switch between these fat-burning and carbohydrate-burning states, but this metabolic plasticity seems to be better maintained in animal models on a folate-limited diet.”
As per this study, the males on folate-limited diets registered an overall increase in their metabolic rate during active periods, potentially helping them to maintain energy levels and physical activity.
Heidi Blank, Ph.D., first author of the study, said the folate-limited group could maintain their weight and body fat in old age compared to the other group. Also, the folate-limited models showed no signs of anemia or other negative health consequences, as per the study.
How much folate should you eat daily?
Folate or Vitamin B9 is an inseparable part of your diet. It plays a crucial role in red blood cell formation and for healthy cell function. It is important to take around 400 gm of folate. Folate is even more important during pregnancy and the dosage for expecting mothers ranges from 400 to 1,000 mcg per day. This nutrient should be available in the body for reducing risk of birth defects of brain and spine.
Folate and vitamin B12 are micronutrients required for essential metabolic functions. The metabolism of both vitamins is closely intertwined. Deficiencies of folate and vitamin B12 are common clinical conditions with significant subclinical and clinical health consequences. Several studies show that individuals with low levels of these micronutrients tend to have elevated markers of oxidative stress
Should you eat vitamins daily?
The benefits of long-term vitamin use have not been established conclusively. A new NIH study published in JAMA Network Open, didn’t find any association between regular multivitamin use and a lower risk of death in healthy US adults. However, one should include multivitamin in their diet on advise of their healthcare provider.
Credit: The Times of India
This morning, have a protein-rich breakfast for these benefits
Team Metabolic Health
From making us feel satiated to inducing better metabolic health, here are the many benefits of having a protein-packed breakfast. The morning breakfast should be power packed to fuel the body for the entire day ahead. Having a nutritious breakfast is mandatory to start the day right. In an interview with HT Lifestyle, Dietitian Ridhima Khamersa, founder of Ridhima Khamersa Diet Clinic, said, “Breakfast is the first meal of the day and extremely rampant to kick start our metabolism. Eating a well-balanced meal complete in all macros keep us healthy and energetic for the day.” Here are some of the benefits of adding the right amount of protein to breakfast, explained the Dietitian.

“Eating a well-balanced meal complete in all macros keep us healthy and energetic for the day,” said Dietitian Ridhima Khamersa. (Unsplash)
Satiety and appetite regulation:
People who consume a protein rich breakfast have greater satiety and reduced calorie consumption in their subsequent meals. A high-protein breakfast raises the level of the appetite-regulating hormone peptide YY (PYY), which makes us feel satiated for a long time.
High energy levels and cognitive development:
Including a protein rich breakfast in the morning keeps your energy levels up in the morning and also improves cognitive function. A meal high in protein maintains a stable level of blood glucose levels and reduces the dips in energy levels as seen after consuming a high carbohydrate meal.
Better metabolic health:
When you consume a breakfast loaded with protein, it raises the body’s thermogenesis, the mechanism by which the body generates more heat and burns calories. This rise in the body’s metabolism aids in the body’s weight management too.
Muscular growth and recovery:
A protein loaded meal provides all the essential amino acids that are needed for muscular growth and recovery.
Reduction in cravings:
Eating a meal rich in protein makes is crave less sugary and fatty foods during the rest of the day. This happens due to regulation of blood glucose levels and increased satiety, reducing the chances of cravings.
Protein rich foods contain amino acids that are the precursors of neurotransmitters such as dopamine or serotonin, having an important role in mood enhancement.
Heart health:
Having a protein rich meal has shown to reduce the levels of LDL cholesterol (bad cholesterol) while raising the levels of HDL cholesterol (good cholesterol).
Healthy protein breakfast includes besan chilla, dal chilla, eggs, quinoa, hung curd sandwich, sprouts, beans and paneer sandwiches.
Credit: Hindustan Times
GLP-1 Agonists For Weight Loss: What You Need To Know
Team Metabolic Health
Though traditionally used to treat diabetes and lower blood sugar levels, a class of medications called glucagon-like peptide 1 (GLP-1) agonists can also decrease appetite and promote weight loss, making their use for shedding weight increasingly popular.
Some brands are prescribed off-label for weight management, while others are Food and Drug Administration (FDA) approved for weight loss for people with obesity or overweight.
Read on for everything you need to know about GLP-1 agonists including how they work, whether or not they’re effective and who might be a good candidate for these medications.
What Are GLP-1 Agonists for Weight Loss?
GLP-1 agonists are a class of medications used to treat type 2 diabetes and obesity. Only two types of GLP-1 agonists are approved for chronic weight management for people with overweight or obesity (without type 2 diabetes): Wegovy and Saxenda. Other GLP-1 agonists, such as Ozempic, are approved for the treatment of type 2 diabetes, but may also be prescribed off-label for weight loss in some cases. Ozempic is the same chemical compound as Wegovy, but packaged as Ozempic for the treatment of diabetes.
Keep in mind that all GLP-1 agonists should be used alongside diet and exercise to promote long-term weight loss, and like all weight loss medications, these drugs are intended for long-term use in order to be effective. Weight regain is likely after you discontinue use of the medication.
How Do GLP-1 Agonists Work for Weight Loss?
GLP-1 agonists work by mimicking the effects of a hormone called GLP-1, which is produced naturally in the body in response to food consumption. This hormone is involved in regulating insulin secretion, feelings related to hunger and the emptying of the stomach. GLP-1 agonists bind to GLP-1 receptors in the body, thereby resulting in the same effects.
“By activating receptors in the pancreas, [GLP-1 agonists are] able to regulate insulin and control blood sugar,” explains Spencer Nadolsky, D.O., an obesity specialist physician based in Portage, Michigan and medical director of Sequence, an online weight loss program. “But they also activate receptors in the brain to curb appetite and in the gut to slow stomach emptying.”
A GLP-1 agonist can impact satiety and cravings to support weight loss, he adds. “It helps you eat fewer calories by making you feel more satisfied with decreased cravings.”
How Effective Are GLP-1 Agonists for Weight Loss?
“Studies demonstrate that a GLP-1 agonist along with a diet and exercise program will result in up to 15% body weight loss,” says Jason Balette, M.D., a bariatric surgeon at Memorial Hermann in Houston, Texas. “The patients in these same studies with diet and exercise alone lost on average about 2.4% body weight.” (note that this study was funded by Novo Nordisk, a pharmaceutical company that produces GLP-1 agonists).
One study comparing the effects of the GLP-1 agonists semaglutide and liraglutide—both of which are approved specifically for weight loss—found that participants (all of which did not have diabetes but did have obesity) lost an average of 15.8% and 6.4% of their body weight, respectively, after 68 weeks[1]. Another study on the effectiveness of liraglutide found that 62% of participants lost at least 5% of their body weight after six months, while around 17% experienced at least 10% weight loss[2].
Who Is a Good Candidate for GLP-1 Agonists for Weight Loss?
“GLP-1 agonists are not intended for individuals looking to lose a few pounds,” says Dr. Nadolsky. He explains that you must meet specific FDA guidelines and criteria to qualify for a prescription, including having a body mass index (BMI) of at least 30 or a BMI of at least 27 with at least one weight-related condition, such as high cholesterol, type 2 diabetes or high blood pressure.
GLP-1 agonists are also not recommended for certain groups, including people who are pregnant, those with digestive conditions like inflammatory bowel disease (IBD) or gastroparesis and individuals with a family or personal history of pancreatitis or thyroid issues, such as multiple endocrine neoplasia or medullary thyroid cancer. A doctor can help determine if you might be a candidate for a GLP-1 agonist based on your medical history and weight loss goals.
Credit: Forbes
