Why you must never take vitamin B12 supplement at night
Team Metabolic Health
Vitamin B12 plays an important role in maintaining the health of your nervous system and red blood cells, said Dr Aniket Mule, consultant internal medicine, Wockhardt Hospitals, Mira Road
Often, we fail to follow the dos and don’ts when it comes to foods and medicines — simply because there is so much to remember. But that’s just us. You must always stick to having vitamin D capsules after breakfast or lunch because it is fat soluble, and vitamin b12 supplements during the day and not at night. Why, you ask? According to nutritionist Amita Gadre, taking vitamin B12 supplements at night can mess with your sleep cycle. “Since B12 boosts energy, it’s best to take it earlier in the day. Timing is everything when it comes to supplements,” said Gadre.
Vitamin B12 deficiency, following which the supplements are advised, usually presents symptoms like anaemia, feeling tired or weak, trouble while walking, weight loss, irritability, poor appetite, and diarrhea. According to the Cleveland Clinic, it is usually seen in people who do not get enough vitamin B12 from their diet or when their digestive tract does not absorb enough.

When is a good time to take a supplement? (Source: Getty Images/Thinkstock)
Vitamin B12 plays a vital role in maintaining the health of the nervous system and red blood cells, said Dr Aniket Mule, consultant internal medicine, Wockhardt Hospitals, Mira Road. “Vitamin B12 is best taken in the morning due to its role in energy production. It helps form red blood cells, supports nerve function, and contributes to DNA synthesis. As a result, it boosts energy levels and can increase alertness,” said Dr Ramesh A, consultant, internal medicine, Gleneagles Aware Hospital, L.B. Nagar, Hyderabad.
Agreed Dr Aniket Mule, consultant internal medicine, Wockhardt Hospitals, Mira Road, Mumbai, and said that vitamin B12 supplement plays a crucial role in energy metabolism and nervous system function and, hence, should be taken during the day. “This is so because the B12 can increase alertness and reduce feelings of fatigue, which could lead to difficulty falling asleep,” said Dr Mule.
Dr Mule added that one may also feel energetic and fail to sleep well at night. “It is also believed that B12 at night may not only impact the body’s absorption process but also interfere with other nighttime bodily functions that take place to repair and recover processes essential for overall wellness,” he told indianexpress.com.
Dr Ramesh recommended taking Vitamin B12 supplements earlier for optimal absorption and to avoid sleep disturbances.
This supplement is most often recommended to patients during the day. However, if your doctor has particularly advised you to take vitamin B12 at night, it is best to follow their instructions,” said Dr Mule.
If you have specific medical conditions or dietary restrictions, consult your healthcare provider for personalised advice on timing and dosage.
DISCLAIMER: This article is based on information from the public domain and/or the experts we spoke to. Always consult your health practitioner before starting any routine.
Credit: The Indian Express
Amgen’s weight-loss drug fails to impress in study; shares plunge
Team Metabolic Health
Amgen’s experimental drug MariTide helped overweight or obese patients shed up to 20% of their body weight in a mid-stage trial, but the results failed to meet lofty investor expectations and shares of the biotech company fell 4.8% on Tuesday.
The year-long trial involving 592 people tested several different doses of the drug as a monthly or bi-monthly injection. Amgen said it also planned to study quarterly dosing.
Analysts said the weight-loss benefit was in line with currently available once-weekly injected drugs from Novo Nordisk (NOVOb.CO), opens new tab and Eli Lilly (LLY.N), opens new tab, while Amgen’s drug had slightly more side effects.
Novo’s Wegovy led to 15% weight loss over 68 weeks, while Zepbound helped patients lose more than 22% of weight over 72 weeks in trials.
Trial data showed that about 11% of patients on MariTide dropped out of the study due to adverse side effects. That compares with about 6% discontinuations in late-stage studies of Zepbound, said J.P. Morgan analyst Chris Schott.
Amgen said nausea and vomiting events were mild and substantially reduced as the dose escalated.
“While Maritide is clearly effective and will offer less frequent dosing, the bar for efficacy in the class continues to move higher,” Schott said.
He added that the Street expects Novo and Lilly’s experimental drugs – CagriSema and retatrutide – to deliver a minimum of 25% weight loss.
Shares of Amgen fell 4.8% to $280.01 at close, erasing more than $7 billion from the Dow component’s market value.
Credit: Reuters
Biden proposes expanded Medicare, Medicaid coverage of obesity drugs
Team Metabolic Health
U.S. President Joe Biden on Tuesday proposed expanding coverage of anti-obesity drugs, like Novo Nordisk’s (NOVOb.CO), opens new tab Wegovy, for more than 7 million people with Medicare and Medicaid health coverage, which could cut out-of-pocket expenses for some by as much as 95%.
This would enable more Americans to afford new weight loss medications in the GLP-1 class that have been shown to reduce weight by as much as 20% on average and can help prevent type 2 diabetes but cost as much as $1,000 a month without insurance coverage. The drugs have also been shown in trials to lower the risk of heart attacks and cardiovascular-related death.
Injection pens and boxes of Novo Nordisk’s weight-loss drug Wegovy are shown in this photo illustration in Oslo, Norway, November 21, 2023. REUTERS/Victoria Klesty/File Photo
Current rules for the Medicare government health insurance program cover the use of GLP-1 drugs such as Eli Lilly’s (LLY.N), opens new tab Mounjaro and Novo’s Ozempic for conditions like diabetes, but not the versions of those drugs like Wegovy that have been approved to treat obesity as a condition on its own.
Medicaid programs, which are state-run, can cover the drugs but many choose not to.
Lilly’s shares were up 4.4%, while Novo’s U.S.-listed shares were up around 1.5% in afternoon trading.
The proposed regulation, which was posted on the Federal Register by the Department of Health and Human Services on Tuesday, would require Medicare to cover these drugs as a treatment for obesity, expanding access for an estimated 3.4 million Americans with Medicare.
It would also expand access to the medications for approximately 4 million adult Medicaid enrollees, according to the White House.
The program would be effective starting in 2026 if President-elect Donald Trump’s incoming administration backs the move; the rule’s comment period is open until Jan. 27, after the inauguration. Robert F. Kennedy Jr., Trump’s choice for health secretary, has said that America should tackle obesity through healthy eating, not medicine.
“This is setting up a political landmine for the Trump administration,” said Ge Bai, professor of health policy and management at Johns Hopkins University.
Because the incoming administration is going to be under pressure to cut costs, Bai said the move could help critics on the left build a narrative that Trump is taking away important health benefits.
Indeed, Democratic Senator Ron Wyden said on Tuesday that he was pleased to see the broader coverage and would be watchdogging the Trump administration to ensure there is no backsliding.
Credit: Reuters
Exclusive: Thousands turn to Wegovy copies each month as FDA considers shortage status
Team Metabolic Health
More than 200,000 prescriptions for copies of Novo Nordisk’s (NOVOb.CO), opens new tab weight-loss drug Wegovy are getting filled by U.S. patients each month, an industry group told the U.S. drugs regulator in a letter, saying it should consider their role in alleviating the obesity drug supply crunch before barring them.
The U.S. Food and Drug Administration is weighing whether to remove Wegovy from its shortage list, which has allowed compounding pharmacies to combine and mix copies of the highly sought-after drugs for more than a year.

Injection pens and boxes of Novo Nordisk’s weight-loss drug Wegovy are shown in this photo illustration in Oslo, Norway, November 21, 2023. REUTERS/Victoria Klesty/Illustration/File Photo
Americans who cannot afford Wegovy or have struggled to find it have been turning to often-cheaper compounded versions sold by pharmacies and telehealth providers like Hims & Hers Health (HIMS.N), opens new tab. Wegovy has been shown to help patients lose as much as 15% of their weight on average.
Once off the shortage list, the pharmacies could be forced to halt production, potentially pushing patients back to Novo, which has so far this year nearly tripled its weekly U.S. supply.
Monthly U.S. prescriptions of Novo’s Wegovy are running about four times that of these compounders, based on member survey results from the Alliance for Pharmacy Compounding, which represents compounding pharmacists and technicians.
The survey results and the compounding industry’s letter to the FDA have not been previously reported. The group said the count was likely conservative since not all members responded.
Novo Nordisk declined to comment. It has previously said it wants to ensure patients receive only FDA-approved, safe and effective semaglutide products, and has applied to the FDA to exempt the drug from U.S. regulations that allow it to be compounded.
The FDA said it was working to determine whether the demand or projected demand for semaglutide within the U.S. exceeds the available supply, and that while compounded drugs serve an important medical need for certain patients, they also present a risk because they are not approved by the agency.
Credit: Reuters
What’s keeping us awake and at what cost?
Team Metabolic Health
More and more Indians across ages are catching fewer hours of sleep than ever before. Here’s looking at India’s new tribe of ‘woke’ people
“Error 404: Sleep not found.” That was the insta message card that changed the life of 31-year-old Karthik Bhaskar, who would scroll his way to dawn, sleep at 5 am and wake up three hours later to be in time for his corporate job. “Being a movie buff, I devoured world cinema in my after-hours. My alertness levels went up, my brain could not wind down, my stress hormone cortisol was dangerously high and my body crashed after my 30th birthday. It turned me into a zombie. I felt disembodied and scared,” he says.
Studies have shown that 61 per cent of Indians reported fewer than six hours of uninterrupted night sleep over the past year (Illustration: Komal)
After intense self-help therapies, he now sleeps by 11 pm, goes for a morning run and then heads to office. “All my waking moments are so full and active these days that I fall asleep easily,” says the IIM Bangalore alumni, who has started an online wellness newsletter, ‘Tiny Wins, A Letter from Your Future Self on 0.1 per cent Growth Daily’.
“When it comes to sleep, motivation won’t take you places, discipline will. Discipline cultivates a habit and puts your life on autopilot,” says Bhaskar, who now helps young people restructure their lives, not just their sleep. There are many like him in the ‘vampire’ tribe who are battling sleeplessness, purely because of a habit of their own making, seldom because of an underlying health condition. Like Srigandh Nagaraj, 33, a Bengaluru-based environmental engineer working remotely for a Singapore firm, who had gotten so comfortable with the idea of not sleeping and living life in the moment that he literally woke up after blanking out while driving. “Watching reels is the new smoking,” he says.
Delhi’s Rishabh Chauhan, 27, would feel a workplace high even after two hours of sleep, till he felt cut off in his nocturnal island. Meanwhile in Chennai, Srijata Narayanan, 33, got so addicted to doomscrolling that she developed hyperanxiety.
Indians across age groups are sleeping less. Much of it is driven by habit rather than medical reasons. “Call it a brain pop, when the control centre of the human body is overstimulated and on a high. This has a cascading effect on the heart, gut, hormones and other organs. Then it becomes a vicious cycle of sleep-deficit causing disease and disease causing sleep deficit. Just going by the complaints of my patients, I would say that Indians today are sleeping no more than four hours,” says Dr Vivek Nangia, head of Pulmonology and Sleep Medicine at Delhi’s Max Hospital.
A social media platform, LocalCircles, has found that 61 per cent of Indians reported fewer than six hours of uninterrupted night sleep over the past year. The sleep solutions company, Wakefit, has found that in 2024, about 88 per cent respondents are on their mobile phones before going to bed, and as many as 54 per cent stay up beyond bed time to consume social media and OTT content.
What’s driving us to stay up?
“A lack of mindfulness and respect for oneself,” says Dr Nangia, bluntly. Of all our bodily functions, sleep seems to be the most negotiable, an indulgence rather than a necessity. Worst, in performance-driven lives, it seems like a frivolity. As Nagaraj says, “I, too, felt the pressure of building social accountability. A social media index is like a goalpost, not only for your peers but your friends, too. So you make time for it. Besides, late night is the only time most people can devote to personal freedoms without a stopwatch dangling over their heads. It’s easy to control the last few hours of your day. Two-and-a-half hours on Bengaluru roads, 12- to 14-hour work days, chores and regular activities had pushed sleep lower down my to-do list. I had given up sports, even talked to my five-month baby while driving so that he became familiar with my voice.”
This is what’s called the “revenge bedtime procrastination,” a pop psychology term since 2014, meaning a let-yourself-go moment with electronic device use. This ‘self-command’ mode is actually ‘self-defeatist’ because we do not understand the function of sleep. Dr Viny Kantroo, respiratory and sleep medicine expert at Delhi’s Indraprastha Apollo Hospital, says that one out of every 10 patients she sees has a sleep disorder. “We not only underestimate the value of sleep but its quality. Deeper planes of sleep are required for cell restoration. That’s the time when the body gets rid of toxins, which are inflammatory molecules in the body. Be it diabetes, obesity, heart disease, everything happens from inflammation. It is also the time when metabolic waste is flushed out from the brain, preventing dementia. The nutrient assimilation from the food we eat is incomplete when we sleep poorly,” she explains.
Research has shown that most lifestyle-induced diseases are controlled easily by eating, sleeping and waking up according to the diurnal cycle to which our bodies are programmed. Although compensatory sleep during day time is inevitable for shift workers, it is the night sleep that matters. “Cortisol, your wake-up hormone, is a day hormone.
Melatonin, the sleep-inducing hormone, kicks in during the evening, peaks at 10 pm and starts dipping post 2 am. So when you stay up late, the body and hormones get confused. The cortisol has to reactivate itself while the melatonin doesn’t know if it has to wind down. With continuous suppression, its levels get depleted and you remain sleepless. This also raises levels of ghrelin, your hunger hormone, and makes you raid the refrigerator in the middle of the night, piling up more calories than your body can burn at that hour,” says Dr Kantroo.
Young people have a high metabolism, so they have the energy reserve to sustain wear-and-tear caused by this mad tussle in the body. “My patients are usually in the 15-25 age group, who suppress sleep because of peer pressures and study load for competitive exams. Or in the 30-45 working professional age group. The background noise has happened but is not showing up. That’s why we see young heart attacks, early onset diabetes, hypertension and obesity,” says Dr Kantroo.
Sleep has many stages. The first stage is when you are still aware of your surroundings. The second and third stages are the deeper and restorative sleep, when you are not receptive to the environment. This should ideally last four hours or make up 60 per cent of your sleep, according to Dr Kantroo. The last stage is the rapid eye movement (REM) sleep where dreams happen and memories are consolidated, and should last one-and-a-half hours. If this pattern is broken frequently or crunched into two hours, like Chauhan did at one time, a sudden sleep attack during daytime could happen and can paralyse you. “I would crash without warning and sleep for 16 hours at a stretch after three days of barely sleeping for two hours,” he admits.
Nagaraj got worried when he started snoring, wondering if he had a medical condition like sleep apnea, when airways collapse and shallow breathing disrupts oxygen flow. Though his sleep therapist ruled that out and suggested melatonin supplements for sleep hygiene, he didn’t want to be dependent. He took a tough step, deactivating his social media accounts and signing out of chat applications at a certain hour. “I had to be healthy for my baby. I realised social media was not really knowledge-worthy, there’s always the Internet to refer to. I saved over two hours, slept earlier, woke up earlier and found time for Suryanamaskara. I limited partying, avoided drinking on Fridays. Now on weekends, we go on drives, visit my parents and engage in some real-world socialising. In short, I moderated every indulgence,” says Nagaraj, who claims to have understood his body’s needs like balancing an equation.
Bhaskar, who had pushed his bedtime to 2 am and then to 5 am, had a rude awakening one day when he felt utterly exhausted after climbing a flight of stairs. “I realised I had become a creature of habit. I stopped watching films at 11 pm which would keep me awake till 1 am. I chose reading self-help books like Atomic Habits (2018), which helped me make small changes every day. I rolled back my sleep time by 15 minutes at first, then half-an-hour. After 60 days, I could sleep by 12.30 am instead of 4 am,” he says. He now dozes off by 11 pm after a light dinner at 8 pm. He deleted video-streaming apps on his phone and reset the time settings to lock apps. “Just make bad habits difficult to access and half the battle is won,” says Bhaskar.
He now has daily conversations with his mother, something he missed earlier as he would wake up late and make a mad dash to work. “I have started the 100-day running challenge with my friends, beginning with 500 metres and hoping to do 10 km a day. Since it is a group project, I know I will commit to it,” says Bhaskar. He even has a checklist, realistically pushing work that’s not a priority to another day and evening out the work pressure over days. His newsletter is a hit and he uses his morning walks to gather feedback.
Chauhan is currently on talk therapy to deal with his deep-seated childhood trauma of his mother’s death, one that kept him awake and made him listless. “I now eat clean and do Vipassana, which helps you bring your mind to the present moment of body awareness. So if your body is tired, the mind will focus on it instead of wandering off, telling you to rest,” he adds. Research by the Department of Science and Technology has shown that Vipassana meditation practitioners transition from light to deep sleep faster and have a longer duration of deep sleep. It can even increase REM sleep states.
Both he and Narayanan are trying out sleep aids like mattresses and pillows made out of memory foam that support the body and help you fall asleep comfortably. Narayanan has taken her sleep hours so seriously that she’s become obsessed with the sleep tracker data on her smartphone. “The first thing I do in the morning is check my sleep quality,” she says.
This addiction is called orthosomnia, something that Dr Suhas HS, sleep medicine expert at Manipal Hospitals, Bengaluru, sees routinely in the IT hub. The problem is sleep trackers only measure your dormant state, not your quality. “Only a clinical study can tell you about heart rate, brainwaves, breath patterns, snoring index and diagnose if your sleep disorder is habitual or medical. Besides, why build up another stress? Just seeing the sun first thing in the day can recharge you,” he says. At least India’s youngsters are trying to find their sweet spot, with or without the sun.
Credit: The Indian Express
A Recipe for Better Obesity Care: Integrating GLP-1s with Food as Medicine
Team Metabolic Health
Nutrition isn’t a supplement — it’s foundational to metabolic health. It’s time we integrate more ‘Food as Medicine’ initiatives alongside the GLP-1 therapies that are gaining traction. GLP-1 receptor agonists, like Wegovy and Ozempic, have taken center stage in obesity and diabetes treatment, praised for their ability to curb appetite, reduce “food noise,” and slow digestion for dramatic weight loss results. While these medications play a strong role in chronic disease management, they’re no replacement for healthy nutrition. Food itself is one of the best therapeutic tools for long-term health — and it’s certainly less expensive than GLP-1 therapies. In fact, a recent study reveals that nationwide use of Medically Tailored Meals (MTMs) for patients with diet-sensitive conditions, like obesity and diabetes, could prevent around 1.6 million hospitalizations and save $13.6 billion every year. It’s time we stop treating nutrition like a side dish in healthcare. If we truly want to optimize population metabolic health, we need to integrate more ‘Food as Medicine’ approaches with pharmacotherapy for better obesity and diabetes outcomes — and cost savings.

Monica Vajani, Executive Director for mHUB’s MedTech Accelerator, discusses how mHUB is helping innovators transition healthcare towards value-based care.
To fully integrate Food as Medicine into chronic care, we need to focus on prevention, companion therapy, and post-medication strategies:
Prevention – Medically Tailored Meals (MTMs) and Groceries (MTGs) offer nutrient-dense, heart-healthy options for conditions like prediabetes and heart disease. Combining these with Medical Nutrition Therapy (MNT) and personalized plans could transform preventive care. Regular screenings, lifestyle counseling, and dietitian partnerships must become part of standard care to make this work.
Companion therapy – Registered dietitians can work with physicians prescribing GLP-1s to create nutrition plans that address muscle preservation, micronutrient intake, and gut health. Higher protein diets, functional foods like prebiotics and probiotics, and medically tailored meal replacements can complement GLP-1 therapy and improve outcomes. Taking advantage of diminished food noise when on GLP-1s, dietitians can help patients focus on mindful eating choosing foods to fuel their body rather than their emotions. Collaboration between dietitians, physicians, and pharmacists is essential.
Post-medication strategy – After GLP-1 therapy, Food as Medicine is critical to maintaining health. Research shows that many individuals experience a reversal in weight loss and other health markers (like fasting blood sugar levels, cholesterol, blood pressure, and more) when coming off anti-obesity medications. Prescriptive nutrition plans, coupled with medically tailored meals, can help sustain the positive outcomes achieved during therapy.
Driving innovation and collaboration in the Food as Medicine movement
There’s a lot of potential for creative collaboration. Healthcare providers and dietitians can partner with major food retailers like Kroger or Walmart to offer MTGs, with stores featuring dedicated sections for these products. “Food prescriptions” could be fulfilled through local or online grocers, blending convenience with clinical nutrition.
Food companies could team up with health systems to provide medically tailored meal services for chronic conditions. For example, a diabetes management meal plan delivered via a service like Hello Fresh, combined with nutrition education, could create lasting health impacts.
Digital health platforms are another avenue for innovation. As employers increasingly adopt digital health solutions for chronic disease management, FAM interventions can be seamlessly integrated, allowing companies to track engagement and health outcomes, demonstrating cost savings and better health for employees. According to this study, providing medically tailored meals increases dietary adherence above 90% and allows patients to realize significantly better chronic disease control. Dietitian-led obesity solutions present an opportunity to scale medically tailored meal support to whole populations.
Medically Tailored Meals could be a game-changer for underserved, food-insecure populations struggling with chronic conditions like type 2 diabetes and obesity. By partnering with social impact investors, public health agencies can make FAM programs a staple within Medicaid, Medicare, and SNAP, ensuring everyone has access to nutritious meals. Together, these collaborations can break down barriers to health equity and make healthy food accessible to all.
Building a future for sustainable health
Scaling the Food as Medicine movement requires cross-industry partnerships and creative solutions. By fostering collaboration between healthcare, technology, employers, insurers, and the food industry, we can make nutrition a core component of healthcare. Together, we can improve outcomes, drive innovation, and build a sustainable future where food truly is medicine.
Credit: medicitynews.com
China Leads the Boom in Continuous Glucose Monitoring Devices
Team Metabolic Health
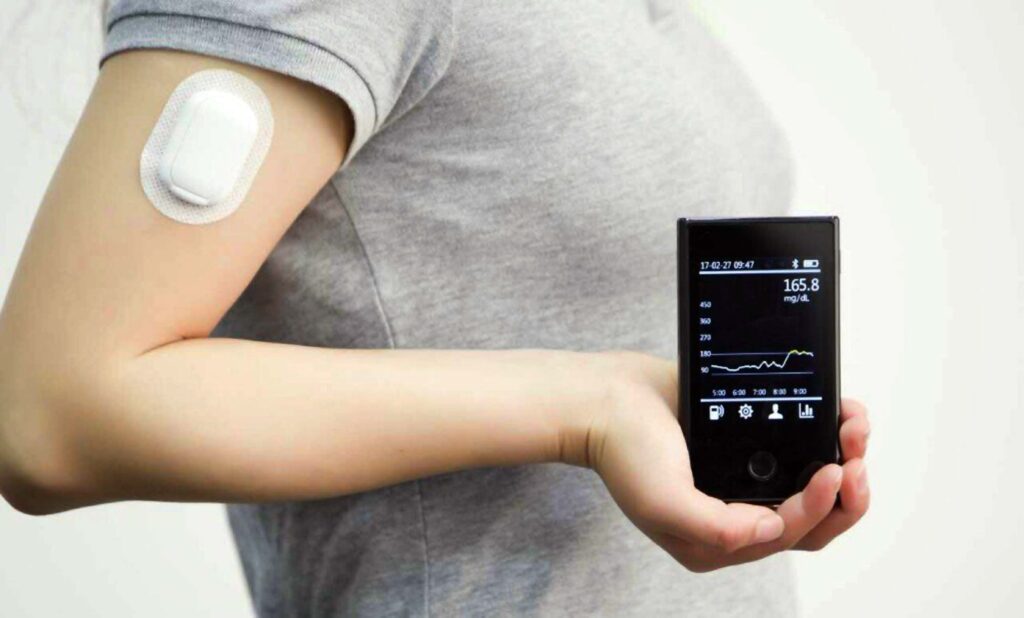
Over the past decade, China has emerged as a leader in the development and production of continuous glucose monitoring (CGM) devices. Several Chinese medical device companies have risen to challenge traditional leaders from the United States and Europe. Companies like Ypsomed, Lepu Medical, and Panasonic Healthcare have invested heavily in R&D and manufacturing to develop high-quality, affordable CGMs.
Lepu Medical was one of the first Chinese companies to commercialize a CGM system. Their Smart Sensor won regulatory approval in 2013 and quickly gained popularity in China and other Asian s. The device offered real-time glucose readings through a mobile app at a much lower cost than competing products from abroad. Recognizing the growth potential, many medical investors poured resources into CGM startups throughout China.
Exporting Quality CGMs Globally
Driven by cost advantages and technological progress, China Continuous Glucose Monitoring Devices exports have skyrocketed in recent years. Companies like Ypsomed have received FDA and CE Mark approval, allowing them to penetrate Western s. Their Balance CGM system matches the performance of leaders but retails at 30-50% lower price points. This value proposition has won over both individuals and institutional customers like hospitals and insurers.
Chinese manufacturers have also become major suppliers to North American medtech giants. Companies will often partner with Chinese OEMs for contract manufacturing or joint ventures. For example, Dexcom produces some of its CGM sensors in a Panasonic Healthcare factory in China. These partnerships allow global firms to keep costs low while China gains access to international sales channels and technical expertise.
Improving Technologies to Drive Future Growth
While China has achieved success exporting basic CGM devices, the next phase of growth relies on continuous technological advancement. Domestically, Chinese companies are striving to match the innovation of American and European competitors. Areas of focus include miniaturization, extended wear time, enhanced accuracy, and integration with artificial intelligence platforms.
Ypsomed’s Micro Pump system represents an innovative leap. The tiny pump and refillable CGM sensors can provide glucose readings for up to 90 days, removing much of the hassle of daily CGM use. If proven effective in clinical studies, Micro Pump could disrupt the CGM . Lepu Medical is developing algorithms using machine learning techniques to predict glucose trends, giving users more time to react to changing levels.
Regulatory Hurdles Remain
Although Chinese CGM technology is advancing rapidly, regulatory and quality approval remains an obstacle for broader global expansion. International standards like FDA clearance involves extensive clinical testing that Chinese companies have only recently been undertaking. Gaining the trust and acceptance of global medical authorities will be crucial for long-term success abroad.
Quality management also needs improvement to meet stringent Western requirements. Early issues with reliability and sensor accuracy meant Chinese devices faced distrust in some overseas s. Regulators are keeping a close watch to ensure patient safety as Chinese exports grow. Companies must demonstrate robust, consistent quality if they want to dominate as leaders rather than low-cost suppliers.
The Future Looks Bright
If Chinese CGM manufacturers can successfully navigate regulatory challenges and continue pushing technical boundaries, the future outlook is highly promising. With a large domestic diabetes population and lower manufacturing costs, China is primed to be a dominant global force. Cooperation with multinationals will also help Chinese players access international expertise while expanding sales networks. Although competition will remain fierce, China’s commitment to CGM innovation points to many more breakthrough products ahead that can transform diabetes management worldwide.
Credit: marketwebjournal.com
Google Invests $20 Million to Drive AI-Powered Scientific Discoveries
Team Metabolic Health
Google’s $20M Fund Aims to Revolutionize Science with Artificial Intelligence
Google is making a significant investment in the future of science and research by committing $20 million in funding and an additional $2 million in cloud credits. This initiative, spearheaded by Google.org, aims to empower scientists and researchers to tackle complex challenges and achieve groundbreaking discoveries using artificial intelligence (AI).
Demis Hassabis, CEO and co-founder of Google DeepMind, emphasized the transformative potential of AI in scientific endeavors. “I believe artificial intelligence will help scientists and researchers achieve some of the greatest breakthroughs of our time,” Hassabis stated. The fund, announced via Google.org, seeks to foster collaboration between public and private sectors while encouraging innovative applications of AI in science.

The funding program targets projects that leverage AI to solve intricate problems at the intersections of various scientific disciplines. According to Maggie Johnson, Google’s VP and global head of Google.org, fields such as rare and neglected disease research, experimental biology, materials science, and sustainability hold tremendous promise for AI-driven advancements.
Winning applicants will benefit not only from financial support but also from access to Google’s cloud infrastructure, enabling them to scale and power their research projects effectively. Johnson highlighted that the initiative aims to inspire excitement around AI’s potential in science and encourage other stakeholders to join in funding similar efforts.
This move by Google follows a broader trend of tech giants investing in AI-driven research. Recently, Amazon Web Services (AWS) announced $110 million in grants and credits to attract AI researchers to its ecosystem. The competition among tech companies to lead AI innovation underscores the growing recognition of AI’s pivotal role in shaping the future of science and technology.
Hassabis expressed optimism about the initiative’s impact, saying, “We hope the launch of our $20 million fund will inspire further collaboration and renewed enthusiasm for the power of AI and science.” By supporting interdisciplinary projects, Google aims to advance knowledge in areas that could benefit humanity significantly, such as sustainability and health care.
This also attests to Google’s philosophy of approaching other world leading scientific minds. Combined here are direct grants of cash and modern cloud solutions that allow the company to become an important partner of the scientific community in the search for new solutions.
The advent of Google fund is a clear testimony that technologies giant deem AI/Science as a perfect cocktail with which to address the challenges. That this race is intensifying towards actually applying AI for the greater good identifies this move as establishing a model for collaboration between tech executives and scientific scientists.
Credit: analyticsinsight.net
The Many Benefits of GLP-1 Weight Loss Treatment
Team Metabolic Health
Exploring the Whole-Body Benefits of GLP-1 Medical Weight Loss Treatments
The potential of GLP-1 receptor agonists, like Semaglutide and Tirzepatide, extends beyond weight loss to significant whole-body health improvements. Recent studies show GLP-1 medications reduce cardiovascular risks, supporting heart and vascular health, and benefit liver, kidney, and brain functions, helping prevent chronic conditions like fatty liver disease, chronic kidney disease, and cognitive decline.

Cardiovascular and Renal Health
In trials, GLP-1 treatments lowered cardiovascular events by up to 20% and kidney-related complications by 24%, especially in patients with type 2 diabetes. Patients with heart failure and kidney disease saw improved outcomes, underscoring these medications’ role in reducing risks tied to heart and kidney disease. Many cardiologists are now prescribing GLP-1 medications for qualifying patients as a longevity treatment to prevent heart disease.
Decreased Cancer Risk
Obesity significantly increases the risk of various cancers, including breast, colon, endometrial, kidney, and esophageal cancers. Excess body fat can lead to chronic inflammation and hormonal imbalances, such as elevated insulin and estrogen levels, which can promote cancer cell growth and proliferation. Additionally, obesity-related metabolic changes may impair immune function, reducing the body’s ability to fight off cancerous cells, thereby elevating overall cancer risk and impacting cancer prognosis and survival rates. Losing weight decreases your cancer risk!
Liver Health
Obesity is a primary cause of non-alcoholic fatty liver disease (NAFLD), now the most common liver disease in the U.S. Excess body fat contributes to the accumulation of fat in liver cells, leading to inflammation and liver damage over time. NAFLD often progresses without symptoms, but it can advance to more severe liver conditions like non-alcoholic steatohepatitis (NASH) and, eventually, cirrhosis. GLP-1 drugs also support liver health, lowering risks of liver complications and cancer in people with fatty liver disease. Studies show a promising link between these medications and reduced inflammation, potentially delaying or preventing the progression to cirrhosis.
Diabetes Treatment and Prevention
GLP-1 medications offer significant benefits in preventing and managing type 2 diabetes by improving insulin sensitivity, reducing blood glucose levels, and promoting weight loss—all essential factors in diabetes control. By mimicking the GLP-1 hormone, these medications enhance insulin release in response to food intake while suppressing glucagon, helping regulate blood sugar. Additionally, GLP-1 treatments slow gastric emptying, reducing appetite and aiding in sustained weight management, a critical element in diabetes prevention. These combined effects provide a powerful tool for reducing diabetes onset and managing existing cases effectively.
Bone and Joint Health
Beyond organs, GLP-1s may relieve musculoskeletal conditions like osteoarthritis, with patients in trials reporting improved knee pain and mobility. Weight loss provides substantial benefits for bone and joint health by reducing the strain excess weight places on joints, particularly the knees, hips, and lower back. Less body weight decreases the risk of joint damage and inflammation, common in conditions like osteoarthritis. For bones, weight loss can also enhance mobility, improving balance and reducing the likelihood of falls and fractures. Maintaining a healthier weight supports joint longevity, reduces pain, and enables greater physical activity, creating a positive cycle for musculoskeletal health overall.
Sleep Apnea
GLP-1 medication may reduce the severity of sleep apnea symptoms, enhancing overall sleep quality and reducing related health risks. Improvements in sleep apnea can lead to better cardiovascular health, mood, and energy levels, providing substantial relief for patients with this common but often disruptive condition.
Mental and Behavioral Benefits
GLP-1 medications may decrease symptoms of depression by influencing weight loss and modifying brain pathways tied to mood and reward. Studies suggest that GLP-1 treatments can reduce cravings and addictive behaviors, helping stabilize dopamine levels in the brain and potentially alleviating symptoms of depression. Additionally, the psychological benefits of weight loss, such as improved self-esteem and body image, likely contribute to better overall mental health. Together, these effects make GLP-1 therapies a promising option for enhancing emotional well-being.
Looking Ahead
Ongoing research continues to explore these drugs’ far-reaching health benefits across age groups, including patients with early-stage conditions. GLP-1 medications may indeed transform the landscape of weight loss and chronic disease management, making them an exciting option for those seeking comprehensive health improvements. These insights from recent studies reveal why GLP-1 medications may be a powerful tool in advancing whole-body wellness, benefiting patients seeking not only weight loss but also enhanced long-term health outcomes.
Credit: theflowwellness.com
Breaking Down The Winery Chart of Accounts Free Template!

We will work with you to create accurate financial statements and provide guidance on making sound business decisions. Navigating the financial ebbs and flows of seasonal production is a unique challenge for vineyards and wineries. The cyclical nature of grape cultivation and wine production means that cash inflows and outflows are not evenly distributed throughout the year. This irregularity necessitates a strategic approach to cash flow management to ensure that operations remain smooth and uninterrupted.
- Choosing the right location for your winery is crucial for success.
- Its purpose is to help you understand how your DTC shipping costs are managed.
- Sometimes the accounts you need will be dictated by your business circumstances.
- With thoughtful use of classes and tags, you’ll gain an unprecedented understanding of what drives your winery’s financial success.
- Software solutions like QuickBooks, Xero, and specialized agricultural accounting software such as Vintrace or AgCode can streamline the process of tracking and analyzing costs.
- Intuit actively invests in its software, and most of the features it rolls out are genuinely helpful and interesting.
- However, there are some nuances that you need to understand about how it works.
Download a winery chart of accounts example
One advantage of using parent accounts is that you can view your financial reports in both collapsed and expanded forms. When you view your reports in a collapsed form, all of the subaccounts will fold up into the parent account. You could dump all your revenue into one account called “Sales” and call it good. This might be adequate for tax purposes, but it is fairly useless when you are trying to compare how your tasting room is doing compared to your wholesale channels. While QuickBooks Online is a very robust and efficient bookkeeping software for wineries, there are still features within the platform that we don’t use.
Informative Content: Operating a Winery
However, for a growing winery, accrual accounting delivers a more accurate financial picture. We then calculate the cost of wine sold outside of QuickBooks and then post Wine COGS as a journal Online Accounting entry each month. In summary, QuickBooks Online is probably the best bookkeeping software for wineries. For most wineries, we recommend using the QuickBooks Online Plus Plan and then adding on external systems for functions such as payroll and inventory management.

Accounting and bookkeeping built specifically grow unique demands of wineries, only from Protea Financial
However, we’ve only touched the tip of the iceberg when it comes to keeping healthy books for your wine business. If you have more questions, need confirmation, or just want someone to take bookkeeping off of your hands altogether, we’re here to help. The Cost of Goods Sold (COGS) accounts include all of the costs that go into generating your revenue. This includes the costs of making your wine and purchasing merchandise and goods for resale.
- Having more than one sales channel is the reality for most wineries (wine club, tasting room, distributor, etc).
- If your shipping expense recovery ratio is decreasing, you may need to review your pricing strategies and how you charge customers for shipping.
- One commonly used method is First-In, First-Out (FIFO), which assumes that the oldest inventory items are sold first.
- At each stage of production, there are costs for materials, labor, and overhead.
- Common mistakes include not keeping accurate records, neglecting to track all expenses, and misunderstanding tax laws.
- The method you choose for your cost accounting is a crucial decision.
- Budgeting for ongoing expenses without immediate returns is critical during the maturation period.
See the benefits of winery accounting from Protea Financial

Wine accounting helps vineyard owners track income from grape sales, manage expenses related to cultivation, and monitor cash flows. By maintaining detailed financial records, vineyard winery bookkeeping managers can identify cost-saving opportunities, plan budgets more effectively, and improve overall financial health. This enables better decision-making and enhances the vineyard’s financial stability. When managing a winery, one of the most crucial decisions you’ll make is how to handle your accounting. It’s not just about keeping the IRS at bay; it’s about gaining insights into your business to make strategic decisions that enhance your profitability and growth.
Other Income

We publish reports on an accrual basis so you can keep in accurate view of your profitability. If you are on a cash basis for tax, we can provide cash basis reports to your tax preparer at the end of the year. Leveraging our proprietary winery data and industry reports, we offer industry benchmarking services. We compare your winery’s performance against industry peers, providing insights into key metrics such as gross margin, production efficiency, and distribution effectiveness. This benchmarking allows you to identify areas for improvement and make strategic decisions without losing sleep. Protea Financial has a team of experienced professionals who can help you navigate the complexities of wine accounting.
Overview of Accounting Methods
Every employee’s wages, benefits, and payroll taxes must be accounted for and apportioned. If you operate a vineyard in addition to winery, include those labor expenses in your total labor cost. While those costs Bookstime are being accounted for, it’s also vital to track the movement of your inventory. This includes keeping tabs on what materials and labor went into creating specific vintages and blends. Ready to elevate your winery’s financial management to the next level?

Time-restricted eating shows promising weight and metabolic benefits, study reveals
Team Metabolic Health
New research highlights the potential of time-restricted eating and calorie timing as effective, sustainable alternatives for weight management and improved blood sugar levels.
In a recent study published in JAMA Network Open, researchers performed a systematic review and meta-analysis of randomized clinical trials (RCTs) to explore the impact of meal timing strategies on body weight management and metabolic outcomes.
The efficacy of modern approaches to weight loss
The global prevalence of obesity and overweight is sharply increasing, partly because of modifiable lifestyle risk factors, including unhealthy dietary patterns and physical inactivity, both of which are associated with an increased risk of diabetes, cardiovascular disease, cancer, and premature death.
Current estimates indicate that most individuals consume food for more than 14 hours each day and snack late at night, which further increases the risk of type 2 diabetes and worsens glycemic control. Comparatively, intermittent fasting, which involves consuming foods during a six—to ten-hour duration during the active phase of the day, has emerged as a popular weight loss strategy.
Dietary modification, including calorie restriction, is considered the primary strategy for body weight management. Meal timing strategies, such as time-restricted eating (TRE), a form of intermittent fasting, meal frequency reduction, and alteration of calorie distribution throughout the day, have emerged as promising alternatives for people who find it challenging to monitor daily calorie intake for weight loss.
In the current systematic review and meta-analysis, scientists analyze published RCTs to evaluate the long-term impact of meal timing strategies on anthropometric and metabolic outcomes in adults with or without metabolic disease.

Study: Meal Timing and Anthropometric and Metabolic Outcomes. Image Credit: Pormezz/Shutterstock.com
Study design
The scientists searched various electronic databases to identify RCTs that investigated within-day meal timing patterns for at least 12 weeks and reported anthropometric outcomes, such as body weight and body mass index (BMI).
The final analysis included 29 RCTs involving 2,485 participants. The risk of bias analysis showed that about 76% of the selected trials provided low-quality data.
Meal timing strategies evaluated in the reviewed RCTs included time-restricted eating, meal frequency, and daily calorie distribution.
Time-restricted eating
The meta-analysis of RCTs investigating the impact of time-restricted eating on weight management revealed that this strategy can significantly reduce both body weight and BMI. However, time-restricted eating was not found to impact lean body mass or waist circumference.
Study participants with high BMI at baseline lost more weight than those with lower BMI. Greater weight loss was observed with eight hours or less of consuming food every day as compared to feeding times that exceeded eight hours each day.
Regarding metabolic outcomes, time-restricted eating was associated with reductions in fasting blood glucose, glycated hemoglobin (HbA1c), low-density lipoprotein (LDL) levels, and energy intake.
Meal frequency
Lower meal frequency was associated with small reductions in body weight and BMI; however, meal frequency did not appear to impact lean mass or waist circumference measurements. Likewise, meal frequency was not found to impact fasting glucose, HbA1c, LDL levels, or energy intake.
Calorie distribution
Consuming most calories earlier in the day leads to greater weight reduction, lower BMI values, and reduced waist circumference measurements compared to calorie consumption later in the day. Like meal frequency, no clear association was observed between calorie distribution and metabolic outcomes.
Study limitations
A subgroup analysis of the current study confirmed that the weight-reducing effect of meal timing strategies is persistent and does not depend on the training level of clinicians who delivered the interventions. However, most of the reviewed clinical trials enrolled participants from clinical settings and involved clinicians with nutrition training, which may restrict the generalizability of the findings. Similarly, all clinical trials on calorie distribution involved only female participants.
Another limitation of the current study is the low quality of evidence due to the risk of bias and inconsistency. Thus, additional clinical trials with larger sample sizes, similar intervention designs, and longer follow-up periods should be conducted to provide more conclusive results on the health benefits associated with time-restricted eating.
Conclusions
Meal timing strategies implemented for more than 12 weeks can moderately reduce body weight, BMI, and waist circumference measurements. Time-restricted eating was also found to reduce HbA1c and fasting glucose levels, thus indicating the potential utility of this strategy for the management of diabetes.
The strict nature of calorie counting in traditional weight loss interventions is one of the primary reasons contributing to its low adherence, in addition to its association with higher disinhibition, energy intake, and BMI. Comparatively, time-restricted eating may provide a simpler and more flexible approach for healthcare clinicians to support behavioral change in overweight or obese adults.
Credit: news-medical.net
Benefits of Ashwagandha and How Much to Take
Team Metabolic Health
The herbal medicine can increase energy, improve overall health and reduce inflammation, pain and anxiety
If you’re the nervous or stressed-out type, someone has probably given you a mini sermon about the wonders of ashwagandha.
They’ve probably told you that it can do just about everything including make you dinner and put the kids to bed. But if you’re skeptical about herbal medicine, you probably haven’t considered looking into ashwagandha. That’s OK. We’re going to do the legwork for you.
With the help of integrative medicine specialist Yufang Lin, MD, we’ll cover the basics and some of the medically proven benefits of using ashwagandha.

What is ashwagandha?
Ashwagandha (Withania somnifera), also known as “Indian Winter cherry” or Indian Ginseng,” is an evergreen shrub that’s found in India, Africa and parts of the Middle East.
So what is ashwagandha good for?
“Ashwagandha has long been used in Ayurvedic medicine to increase energy, improve overall health and reduce inflammation, pain and anxiety,” says Dr. Lin.
She adds that Ayurvedic medicine is the traditional medicine system in India. It’s a healing tradition that uses nutrition, exercise, mindfulness practices and herbs to promote balance between the body, mind, spirit and the environment.
Ashwagandha seems to fit the bill for those who prefer herbal medicines for several reasons.
Modern life is full of stress triggers. And that stress contributes to physical and mental illness. During stressful moments, the cortisol levels in your body become elevated, and this causes your heart to pump harder and faster. You breathe rapidly and your body generates more glucose for a quick burst of energy. Your mind becomes hyper-focused on any threats, and your body goes into fight or flight mode. When the stressful event is over, cortisol levels normalize and the associated symptoms resolve.
“Unfortunately, when a threat is chronic — whether it’s stress from finances or work — the stressful response also becomes chronic,” says Dr. Lin. “Over time, long-term stress can contribute to persistent inflammation and increases the risk for developing chronic conditions like obesity, diabetes, hypertension, heart disease, stroke, cancer, osteoporosis and fibromyalgia.”
Ashwagandha Benefits
So what does ashwagandha do? Research shows that it can help in several ways:
Normalizes cortisol levels, which reduces the stress response.
Reduces inflammation.
Reduces cancer risks.
Improves memory.
Improves immune function and anti-aging properties.
Eases stress and anxiety.
“People who are stressed or anxious, or people with chronic conditions might turn to ashwagandha to help ease their conditions,” says Dr. Lin.
How much should you take?
Ashwagandha comes in a variety of forms. It’s available in gummies, capsules, liquid drops and powders that you can mix into drinks.
So how much ashwagandha per day should you consume? Regardless of the form you use, Dr. Lin says dosing is usually 500 mg twice a day.
But is ashwagandha safe? Dr. Lin says it mostly depends on the quality of the supplements. Her advice is to look for supplements that have been independently tested and verified by an outside company such as ConsumerLab, United States Pharmacopeia (USP), or National Sanitation Foundation International (NSF International).
Ashwagandha side effects
While the side effects of ashwagandha are minimal, some people may experience:
Gastrointestinal upset, Diarrhea, Vomiting and Nausea.
“Most people can take this supplement, although it is always best to discuss it with your healthcare provider first,” says Dr. Lin.
If you have any issues with your thyroid, Dr. Lin strongly recommends checking with your healthcare provider before taking ashwagandha.
“Ashwagandha can augment thyroid function by increasing the conversion of the less potent thyroid hormone, T4, to the more active form of the thyroid hormone, T3,” says Dr. Lin. “Thus for some people, it can support a healthier thyroid function. On the other hand, if an individual’s thyroid is already borderline hyperactive, ashwagandha could contribute to frank hyperthyroidism.”
Other conditions which require caution when it comes to using ashwagandha include if you’re pregnant or breastfeeding, or if you have an autoimmune disease. In these cases, Dr. Lin advises talking to your provider before taking anything. She stresses this with pregnant women as ashwagandha could cause complications.
Overall, ashwagandha can be a part of your wellness plan — but remember it’s not a cure-all.
“Taking ashwagandha will not make the stress go away, but it may help reduce the symptoms so one feels more at ease,” says Dr. Lin. “But if you take the time to develop coping tools to help manage stress in the future, that will go much further in the long run.”
Credit: health.clevelandclinic.org
How GLP-1 went from being a hard-to-handle hormone to a blockbuster success
Team Metabolic Health
Lotte Bjerre Knudsen, chief scientific advisor in research and early development at Novo Nordisk, discusses the past and future of GLP-1s and related anti-obesity drugs.
Wegovy is now a household name. If not for Novo Nordisk’s Lotte Bjerre Knudsen, the GLP-1 drugs it represents might have been a footnote in drug development history.
Evidence started accumulating in the late 1980s that the GLP-1 hormone could be used to induce insulin secretion, hinting at a path to a new treatment for diabetes and attracting industry interest. Data quickly showed that GLP-1 had a role in obesity too, further raising the prospects for the hormone. But as drug developers struggled to overcome the peptide’s minutes-long half-life or to figure out a small-molecule workaround, investments in the obesity applications evaporated. “They all ran away,” recalls Knudsen, now chief scientific advisor in research and early development at Novo.
Novo had struggled with GLP-1 too, with little to show for it by the mid-1990s. Tasked with a last attempt at bringing the hormone to heel, Knudsen turned to a protein-engineering ‘fatty acid acylation’ strategy to extend the half-life of the hormone, inventing the once-daily GLP-1 analogue liraglutide. Thirty years later, Novo’s next-generation once-weekly GLP-1 analogue semaglutide is a medical and commercial phenomenon, with sales of over US$18 billion last year in diabetes and obesity. Its success has revitalized the hunt for anti-obesity drugs.
Knudsen shared the Lasker prize with Harvard’s Joel Habener and Svetlana Mojsov, now at the Rockefeller University, earlier this year for their contribution to this journey. For Knudsen, the importance of GLP-1 biology in obesity was never in doubt. “The interesting question is why we were the only ones who persevered here?”

Lotte Bjerre Knudsen, Credit: Novo Nordisk
Why did you decide to focus on fatty acid acylation to get to liraglutide?
We had a few ideas beforehand that didn’t work out, and that goes into the thinking on why I actually ended up with this technology.
We’d already tried to just use a native GLP-1 peptide, but that gave patients skin reactions. We’d also tried to stabilize the backbone, but then DPP4 enzymes would still clear the peptide. After one year of work on this, we went from a molecule with a half-life of two minutes to a half-life of five minutes. Great. And we had tried small molecules [GLP-1 receptor agonists] too, but these didn’t work at the time. So we had to come up with something else.
The theory behind our approach was that albumin [the most abundant protein in the blood plasma] can function as a transporter of all kinds of things — including fatty acids that are very poorly soluble in the blood. That physiological principle was already very well described at that time. So, we thought, let’s take this principle and use that to engineer a longer-acting drug molecule by attaching a fatty acid to the peptide.
People had already started to work with this, both on peptide hormones and with larger proteins like insulin, so there were hints that it might work. It sounded like a possible way to extend the drug’s half-life. But it was unproven whether it would work.
Another reason I picked this approach was that I could use my background to work on these molecules. I could have tried to harness GLP-1 by developing small-molecule DPP4 inhibitors, but I’m not an organic chemist. My training was in biotechnology, so I could see myself doing fatty acid acylation experiments.
How did these go?
We made about 200 compounds. It worked out pretty well.
We were really focused on using the native sequence for human GLP-1, because I was very focused on avoiding an antibody response. [Liraglutide has 97% homology with native GLP-1, with just one amino acid difference to make fatty acid acylation more practical.] That was a learning that I had taken from colleagues who worked with larger proteins, that small changes could drive antibody responses. Later on it turned out that this was absolutely true for the GLP-1 class too. Exenatide is still on the market but comes with neutralizing antibodies in a not-insignificant number of the patients. [Exenatide, a peptide with ~50% homology to GLP-1, is based on a protein from the venom of the Gila monster. It secured a first approval for the GLP-1 mimetic class in diabetes in 2005.] And Roche got all the way through to phase III with its taspoglutide but then never filed for approval because they had cases of anaphylactic shock with the drug. [Taspoglutide had 93% homology to native GLP-1, with 2 amino acid changes to improve its stability.]
What we learned is that our fatty acid acylated compounds come with really, really low levels of antibodies. It may be that the fatty acid acylation actually shields for antigenicity — which is something I cannot prove, but I think it’s a good hypothesis.
Once you had a molecule in hand, what was the closest liraglutide came to getting terminated?
We had lots of small delays. The biggest delay we faced was just in learning how to produce the drug, how to scale it up and how to formulate it. And we had to do a phase II trial twice, because the dose we used was too low and we hadn’t figured out how to titrate it yet. But I would still say the development time for liraglutide is not that bad. We formally sent the compound into clinical development in 1997 and our first approval in Europe was in 2009.
Several firms gave up on GLP-1 in that time. A case study showed how Pfizer and Metabio pulled back in the 1990s. Why was that?
There’s a really good quote in that paper from a senior Pfizer leader that said there would never be another injectable therapy for diabetes other than insulin. We also worked with Pfizer in the early 1990s, trying to co-develop a formulation of native GLP-1. But I had not heard that quote before.
I can also share some insight from Richard DiMarchi, who was head of research at Lilly at that point in time. He said earlier this year that he tried to get this project prioritized for obesity at Lilly, but was unsuccessful at the time. Svetlana Mojsov, who was one of my co-recipients for the Lasker, she was told so many times as well that these kind of molecules are not medicines. They’re not drug-like molecules. I also got that pushback when I tried to first get our work on liraglutide into the Journal of Medicinal Chemistry. One of the reviewers asked: why are you doing this, this is not a drug-like molecule. And I wrote back: yes, it is. It’s in phase I clinical development.
You started looking at the obesity applications early on, based on a finding that rats with GLP-1-producing tumours starved themselves to death. Tell me about that.
That was actually an important piece for us. That was back in the paper days, and we didn’t travel then as much as we do today. And Ole Madsen, who made this finding, was working as an independent researcher in Hagedorn Research Institute, back then in the Novo family. I met with him, and heard about that work.
Stephen Bloom’s paper in 1996 confirmed that finding, with a different methodology. Stephen Bloom’s paper showed that GLP-1 controlled feeding when it was injected directly into the brain of rats, but I knew from Ole’s studies that it actually could also potentially control feeding with peripheral administration.
We now know that GLP-1s drive weight loss via the brain. When did you figure that out?
That came later. Apart from actually coming up with these medicines, this is a piece of work that I’m really proud of because it has changed the view on how these medicines work.
In the beginning, we thought the effect of GLP-1 on obesity had something to do with peripheral fullness or effects on the stomach or something. But then we started to look more into the mechanisms, because we saw that there was so much stigma around the disease and these medicines and we were pretty convinced that we would need to explain the mechanism as well as we could if we wanted to get it approved for obesity.
We started to look more into how we could characterize uptake of GLP-1 into the brain, and found that liraglutide can access several parts of the brain. We characterized its effects on POMC neurons, for example, which are a well-established neuronal population with an effect on satiety. Plus it has effects in the hindbrain and in deeper brain regions.
That work was published in the Journal of Clinical Investigation in 2014, but we realized from around 2010 and onwards that GLP-1s had direct effects in the brain. And Randy Seeley, who is at the University of Michigan, showed in the same issue of JCI that when you knock out the GLP-1 receptor from the brain, you lose most of the effects on appetite. We now know that GLP-1 works on multiple GLP-1 receptors to orchestrate an overall reduction in energy intake.
These insights came after you discovered the longer-acting semaglutide, which has almost twice the weight-loss effect than does liraglutide. Semaglutide seems better at getting into the brain, which may contribute to its improved effect. Was that better brain access just a lucky turn of the cards?
Yes and no. There was a strategy for designing semaglutide, which was to make a molecule with a much-longer half-life, with optimized binding to albumin and with a better hydrophobicity profile than liraglutide. With liraglutide, there is a tiny amino acid spacer between the peptide and the fatty acid, whereas with semaglutide there is a whole extra molecule that was designed and put there to optimize the drug. [The team screened around 4,000 peptides before settling on the one that became semaglutide.] We knew that the physical and chemical properties of the drug were changed, we just didn’t know exactly what that meant pharmacologically.
We didn’t know that it would translate into more weight loss. So in that way, that was a really good surprise. And of course, I also have to say that the better brain uptake has only been shown in animals, because there really is no good way to do that in humans.
I think that we now have a very good understanding of the mechanism of action of these drugs on obesity. We have yet to see this understanding be used in drug design, but that could be the case now going forward.
These drugs are meant for chronic usage, but real-world data shows that only 30–50% of patients stay on them. What does that mean?
My take on that is that we just need a whole bunch more understanding of obesity as a serious, chronic disease. Some people still don’t fully buy into the idea that obesity is as serious as diabetes, and there’s still a lack of understanding in society that if people want to maintain the beneficial effects of GLP-1 on health, then these drugs have to be used as chronic treatments.
I think it’s a general problem with many other serious chronic diseases, as well, where there’s a lack of adherence.
What we really should be talking about with GLP-1 is all of the other benefits that they may offer, for the heart, the kidneys, the brain, the vasculature and there’s possibly more. There needs to be a better understanding of that.
Many trials of GLP-1 receptor agonists are ongoing in many other indications. Which of these are you most excited about?
The next big ones for us in phase III trials are our MASH [ESSENCE] trial and our Alzheimer [EVOKE and EVOKE plus] trials, which could show something that has not already been shown. [Results in metabolic dysfunction-associated steatohepatitis (MASH) are due in 2024, and in Alzheimer disease in 2025.]
What are you excited about beyond GLP-1?
The amylin biology, which is also a hormone that has effects on the brain. I’m not sure whether we should call it a neurotransmitter in the same way as GLP-1, but it’s definitely a hormone and it’s a little bit the same story in that it has been around for a while.
Actually, pramlintide [an amylin analogue] has been marketed for a very long time for diabetes, but it turns out that you can actually get much better weight loss if you make a long-acting version of this peptide. And it is complementary to GLP-1 in its physiology: amylin is released from the pancreas, whereas GLP-1 is released from the intestine; they both work on the brain but on different neurons; and they have complementary effects, which might lead to higher weight loss.
We’ve seen some data with GIP [gastric inhibitory polypeptide], and there’s some data coming with glucagon. Amylin is the next thing that will read out. [Novo expects first phase III data on CagriSema, a combination of the long-acting amylin analogue cagrilintide and semaglutide, on weight loss by the end of 2024.
Credit: nature.com
How GLP-1 Medications like Ozempic are Revolutionizing Weight Loss
Team metabolic Health
Whether you’ve seen commercials or read about them in the news, chances are you’ve probably heard of Ozempic and Wegovy. The prescription medications have become household names thanks to their success in helping millions of people lose weight after struggling to do so through diet and other traditional means.
Ozempic and Wegovy are in a class of medications known as the glucagon-like peptide-1 (GLP-1) receptor agonists (activators). These medicines mimic the effects of the GLP-1 hormone, which is naturally produced in specialized L-cells of the gastrointestinal tract. While Ozempic and Wegovy are probably the most well-known medications within the class, there are many other GLP-1 medications that you may not have heard about.
“GLP-1 medicines have been around for almost two decades and were originally developed for managing type 2 diabetes. These medications help regulate insulin secretion and appetite. More recently, the GLP-1s have gained significant attention in promoting weight loss,” says Ryan Centafont, PharmD, BCPS, Doylestown Health’s Director of Pharmacy.

What is GLP-1?
GLP-1 medications were first approved by the U.S. Food and Drug Administration (FDA) in 2005 to lower blood sugar in those with type 2 diabetes. The medication works by stimulating the pancreas to increase insulin production, which lowers blood sugar levels.
In addition to lowering blood sugar, GLP-1 agonists are also FDA approved to treat moderate to severe obesity. GLP-1 medications include:
Semaglutide (Ozempic, Wegovy, Rybelsus)
Dulaglutide (Trulicity)
Exenatide
Exenatide extended release
Liraglutide (Saxenda)
Tirzepatide (Zepbound)
GLP-1 medications are generally administered as an injection in the fatty tissue under the skin. It can be given in the abdomen, upper arm, or thigh. How often the medication is taken varies, but may be weekly, daily or in some cases, twice a day.
Ozempic vs. Wegovy
Today, the most commonly used GLP-1 medication is semaglutide, which is marketed as Ozempic, Wegovy, and Rybelsus. According to a Gallup poll released in May 2024, over 15 million Americans have used either Ozempic or Wegovy.
Ozempic and Wegovy contain the same active ingredient, which is semaglutide. “The main differences between Ozempic and Wegovy are the FDA approved indications and the dosage. Wegovy is approved specifically for weight management in adults with obesity or who are overweight. Ozempic has a lower dose compared to Wegovy and is used to improve glycemic control in adults with type 2 diabetes. Wegovy and Ozempic are both given as once-weekly injections,” says Centafont.
Ozempic and Wegovy are FDA approved to treat different conditions.
Ozempic was approved by the FDA in 2017 to lower blood sugar in those with type 2 diabetes
Wegovy was approved by the FDA in 2021 to promote weight loss in people who have moderate to severe obesity.
As far as similarities, both medications require a prescription and are used to reduce cardiovascular concerns such as heart disease and stroke. The dosage of Ozempic and Wegovy is increased over time until the maintenance dose is reached.
GLP-1 and Weight Loss
While GLP-1 medications were initially meant to treat type 2 diabetes, it was quickly apparent that they also helped people lose weight. “GLP-1s essentially help curb hunger because they slow down the digestion process, which makes you feel fuller faster and for a longer period of time. This results in eating less and ultimately losing weight,” says Centafont.
GLP-1 medications help you lose weight by:
Reducing hunger and appetite
Slowing down digestion
Increasing signals to the brain of feeling full after a meal
Hidden Benefits of GLP-1
Researchers are continuing to study the benefits of GLP-1 medications and are hopeful about some of the additional benefits they may provide. “I think we will continue to see additional studies and new indications for the GLP-1s in the future as their impact has potentially broad therapeutic use for metabolic and inflammatory-based conditions,” says Centafont.
Other additional benefits researchers are studying include:
Brain health – GLP-1s reduce brain inflammation and researchers believe they may improve cognitive function in those with Alzheimer’s disease.
Fertility – Women, especially those with polycystic ovary syndrome (PCOS) may be able to use GLP-1s to increase fertility.
Heart health – Clinical trials show those taking Wegovy had a 20% lower risk of a cardiac events such as a heart attack or stroke.
Kidney function – Studies show that certain GLP-1s improve kidney function and prevent the progression of diabetes-related kidney conditions.
Credit: doylestownhealth.org/blog
Steroidehaus On-line Kaufen, Bestellen 100% Echte Steroide
Steroidehaus On-line Kaufen, Bestellen 100% Echte Steroide
Ruzicka und Butenandt erhielten 1939 den Nobelpreis für Chemie für ihre Arbeit, aber die NS- Regierung zwang Butenandt, die Ehrung abzulehnen, obwohl er den Preis nach dem Ende des Zweiten Weltkriegs annahm. Die Verwendung von gonadalen Steroide vor-frei ihre Identifizierung und Isolierung. Jahrhundert, während seine Wirkung auf die Festigkeit noch untersucht wurde. Die Isolierung von Gonadensteroiden lässt sich bis ins Jahr 1931 zurückverfolgen, als der Marburger Chemiker Adolf Butenandt 15 Milligramm des männlichen Hormons Androstenon aus Zehntausenden Litern Urin reinigte.
Hi-Tech Pharmaceuticals setzt auf Diversität und Expertise, um sich in der Landschaft der Sports Nutrition als Marktführer zu behaupten. Mit cGMP-zertifizierten Anlagen in Georgia und Pennsylvania offeriert die Marke ein breites Spektrum an Ergänzungsmitteln, von Hormonoptimierern bis hin zu Muskelverstärkern. Die Präsenz in strategischen technologischen Zonen zeigt ihr Engagement für stetige Innovation und Weiterentwicklung in der Supplement-Industrie. Zudem fördert es die Produktion von roten Blutkörperchen, wodurch die Sauerstoffzufuhr zu den Muskeln verbessert und die Ausdauer gesteigert wird. Durch seine Anwendung wird die Proteinsynthese gesteigert und die Stickstoffretention im Muskelgewebe verbessert, was letztlich zu einer Zunahme der Muskelmasse und -kraft führt.
- Es ist klar das man für den zweiten Teil mehr al einen Durchlauf benötigt, aber genau das macht den Reiz aus.
- Es ist jedoch sehr wichtig, dass die Einnahme von Clenbuterol aufgrund von Stressfaktoren und Nebenwirkungen auf den Körper nicht länger als eight Wochen dauert, worauf später noch eingegangen wird.
- Die maximale effektive Dosis für die meisten Frauen sollte im Bereich von ca.
- In diesem Artikel werden wir genauer auf die Vorteile, die Dosierung und die möglichen Nebenwirkungen von Boldenone undecylenate eingehen.
- Die Messung der Dissoziation zwischen anabolen und androgenen Wirkungen bei AAS basiert weitgehend auf einem einfachen, aber veralteten und nicht ausgereiften Modell mit Rattengewebe-Bioassays.
Teil 1-Medikamente unterliegen vollständigen Ein- und Ausfuhrkontrollen, wobei der Besitz ohne entsprechendes Rezept strafbar ist. Es gibt keine Beschränkung des Besitzes, wenn es Teil eines Arzneimittels ist. Teil 2 Arzneimittel benötigen für die Ein- und Ausfuhr eine Genehmigung des Innenministeriums, es sei denn, der Stoff liegt in Form eines Arzneimittels vor und ist zur Selbstverabreichung durch eine Person bestimmt. Sowie andere wie 1-Dehydrierung (zB Metandienon, Boldenon ), IGF-1 LR3 kaufen 1-Substitution (zB Mesterolon, Metenolon ), 2-Substitution (zB Drostanolon, Oxymetholon, Stanozolol ), 4-Substitution (zB Clostebol, Oxabolon ) und verschiedene andere Modifikationen. Der Konsum von AAS stört die Hypothalamus-Hypophyse-Gonaden-Achse (HPG-Achse) bei Männern.
Während andere Steroide wie Testosteron teilweise dafür genutzt werden, Patienten mit chronisch entzündlichen Darmerkrankungen zu heilen, behauptet der „Anabolic Doc“, dass Boldenon sogar dazu führen könne, dass man einen Reizdarm entwickelt. Er habe Personen gesehen, bei denen die Einnahme des anabolen Mittels unmittelbar zu Verdauungsproblemen geführt habe. Doch das sei ungewöhnlich und solle ebenfalls von Person zu Person variieren. Zunächst kommt er auf die Geschichte hinter der Substanz zu sprechen und gibt preis, dass das, was wir heute umgangssprachlich als Boldenon bezeichnen, in aller Regel der Ester aus dem Steroid Boldenon und der Carbonsäure Undecansäure ist. Zusammengenommen lautet die korrekte Bezeichnung daher „Boldenon Undecanoat“, welches vom Pharmakonzern Pfizer unter dem Markennamen „Equipoise“ für tiermedizinische Zwecke hergestellt wird. Ursprünglich entwickelte man das Produkt jedoch zum Einsatz beim Menschen und die Veresterung mit der Säure machte es erst möglich, dass das Steroid im Körper nicht sofort abgebaut wird und überhaupt wirksam ist.
Verwendet
Androgene wurden in den 1930er Jahren entdeckt und als androgene (dh virilisierend) und anabole (zB myotrophe, renotrophe) beschriebene Wirkungen charakterisiert. Der Begriff anabole Steroide kann bis mindestens Mitte der 1940er Jahre zurückdatiert werden, als er verwendet wurde, um das damalige hypothetische Konzept eines Testosteron-abgeleiteten Steroids mit anabolen Wirkungen, aber mit minimalen oder keinen androgenen Wirkungen zu beschreiben. Dieses Konzept wurde auf der Grundlage der Beobachtung formuliert, dass Steroide ein signifikant unterschiedliches Verhältnis von renotropher zu androgener Potenz aufweisen, was darauf hindeutet, dass anabole und androgene Wirkungen dissoziierbar sein könnten.
Welche Strafen Drohen Für Die Einfuhr Von Boldenon?
Diese Dosis reicht aus, um die fettfreie Muskelmasse im Vergleich zu Placebo auch bei Probanden, die überhaupt nicht trainierten, signifikant zu verbessern. Dihydrotestosteron (DHT), bei medizinischer Anwendung als Androstanolon oder Stanolon bekannt, und seine Ester sind ebenfalls bemerkenswert, obwohl sie in der Medizin nicht weit verbreitet sind. Boldenon-Undecylenat und Trenbolonacetat werden in der Veterinärmedizin verwendet. Anabole Steroide, auch besser bekannt als anabole-androgene Steroide ( AAS), sind steroidale Androgene, die natürliche Androgene wie Testosteron sowie synthetische Androgene umfassen, die strukturell verwandt sind und ähnliche Wirkungen wie Testosteron haben. Sie erhöhen das Protein in den Zellen, insbesondere in der Skelettmuskulatur, und haben auch unterschiedlich starke virilisierende Wirkungen, einschließlich der Induktion der Entwicklung und Aufrechterhaltung männlicher sekundärer Geschlechtsmerkmale wie das Wachstum von Gesichts- und Körperbehaarung.
Boldenon Und Testosteron In Einer Spritze – Was Sind Die Vorteile Dieser Kombination?
Neben der oralen Aktivität verleiht die 17α-Alkylierung auch ein hohes Potenzial für Hepatotoxizität, und alle 17α-alkylierten AAS wurden, wenn auch selten und nur nach längerer Anwendung (unterschiedliche Schätzungen zwischen 1 und 17 %), mit einer Hepatotoxizität in Verbindung gebracht. Dementsprechend haben sich D-Ring- Glucuronide von Testosteron und DHT als cholestatisch erwiesen. Es wurde festgestellt, dass einige AAS, wie Testosteron, DHT, Stanozolol und Methyltestosteron, den GABA A -Rezeptor ähnlich wie endogene Neurosteroide wie Allopregnanolon, 3α-Androstandiol, Dehydroepiandrosteronsulfat und Pregnenolonsulfat modulieren. Es wurde vermutet, dass dies als alternativer oder zusätzlicher Mechanismus zu den neurologischen und verhaltensbezogenen Auswirkungen von AAS beitragen kann. Es gibt anekdotische Berichte über Depressionen und Selbstmord bei jugendlichen Steroidkonsumenten, aber nur wenige systematische Beweise. Eine Überprüfung aus dem Jahr 1992 ergab, dass AAS Depressionen sowohl lindern als auch verursachen kann und dass die Beendigung oder verminderte Anwendung von AAS auch zu Depressionen führen kann, erforderte jedoch aufgrund unterschiedlicher Daten zusätzliche Studien.
Grund dafür soll sein, dass Boldenon dafür bekannt sei, den freien Testosteronspiegel zu erhöhen und der kombinierte Gebrauch von Equipoise und Testosteron dazu führen könne, dass mehr Testosteron in Östrogen umgewandelt wird. Dies soll jedoch wie so oft von Person zu Person unterschiedlich stark ausgeprägt sein und von der Genetik abhängen. Die gleichzeitige Verwendung von Testosteron außen vor gelassen, habe Boldenon allein jedoch nur minimale androgene Nebenwirkungen, beispielweise Akne oder die Vergrößerung der Prostata. Allerdings könnte es die durch Testosteron verursachten Nebenwirkungen verschlimmern. Aufgrund einer strukturellen Veränderung in Form einer Doppelbindung besitzt Boldenon laut O’Connor zudem geringere androgene und östrogene Wirkungen als Testosteron.
Die Off-Label-Konsumenten der Droge waren hauptsächlich Bodybuilder und Gewichtheber. Obwohl Ziegler Sportlern nur kleine Dosen verschrieb, stellte er bald fest, dass diejenigen, die Dianabol missbraucht hatten, an einer vergrößerten Prostata und atrophierten Hoden litten. AAS wurde 1976 auf die Liste der verbotenen Substanzen des Internationalen Olympischen Komitees (IOC) gesetzt, und ein Jahrzehnt später führte das Komitee „Außer-Wettkampf“-Dopingtests ein, weil viele Athleten AAS eher während ihrer Trainingszeit als während des Wettkampfs verwendeten. Klinische Studien an Menschen, die entweder Methyltestosteron- Dosen oder Injektionen von Testosteronpropionat beinhalteten, begannen bereits 1937. Testosteronpropionat wird 1938 in einem Brief an den Herausgeber des Magazins Strength and Health erwähnt ; Dies ist der früheste bekannte Hinweis auf ein AAS in einem US-amerikanischen Gewichtheber- oder Bodybuilding- Magazin. Gerüchte, dass deutschen Soldaten während des Zweiten Weltkriegs AAS verabreicht wurde, um ihre Aggression und Ausdauer zu steigern, werden oft berichtet, sind aber noch nicht bewiesen.
