A Nutritionist’s Take On Smoothie King’s New GLP-1 Smoothies
Team Metabolic Health
The retail food chain recently launched a new smoothie lineup for people taking GLP-1 weight loss drugs like Ozempic. While their nutritional profiles look promising, some may not differ from non-GLP-1 tailored options already on the menu.
Glucagon-like peptide 1 receptor agonists (GLP-1s), including Ozempic, Mounjaro, and Wegovy, have taken the weight loss arena by storm, becoming the drugs of choice among people with obesity. According to the latest data, 1,449,442 people in the United States were prescribed a GLP-1 between January 2018 and September 2024.
As a result of this Ozempic craze, food retailers are jumping on the GLP-1 bandwagon and launching new products designed to support the needs of people taking these medications. For example, Nestle recently launched Vital Pursuit — a lineup of meals developed to fill gaps in nutrition that might result from the effects of GLP-1s, such as decreased appetite.
On October 29, Smoothie King, a fast-growing retail food chain, followed suit and announced the launch of its new GLP-1 Support menu for people taking the blockbuster weight loss drugs. The company says the new smoothie lineup is designed to help GLP-1 users achieve their weight loss or weight management goals while providing nutrients needed to support hydration and accommodate side effects often associated with the medications.
“For over 50 years, Smoothie King has blended delicious, nutritious smoothies, and we are thrilled to launch this menu as part of our continued commitment to supporting our guests on their personal health and wellness journeys,” said Wan Kim, CEO of Smoothie King in a press release. “We know that every individual’s path is different, and with the rising use of GLP-1 medications across the country and our customer base, we want to ensure that Smoothie King provides the nutritional resources to match.”

Image by Healthnews
What’s in Smoothie King’s GLP-1 smoothies?
According to Smoothie King’s website, the newly launched menu has five smoothie options with 20 or more grams of protein, high fiber content, and zero added sugar. Customers can choose between 20-, 32-, or 40-ounce serving sizes.
The five GLP-1 options include:
Gladiator® GLP-1 in chocolate, vanilla, or strawberry: This GLP-1-tailored smoothie contains the customer’s choice of two of the following ingredients: almonds, almond butter, wild blueberries, strawberries, raspberries, organic ginger, kale, carrots, or spinach. Depending on serving size, the Gladiator GLP-1 has 220 to 560 calories and contains 45 to 61 grams of protein, 2 to 14 grams of fiber, and zero added sugar.
Slim N Trim™ GLP-1 Mango Greens: The GLP-1 Slim N Trim contains mangoes, Greek yogurt, Califia Farms® Almond Milk, Slim N Trim™ Blend, organic kale, ginger, and spinach. A 20-ounce serving provides 200 calories, 22 grams of protein, 5 grams of fiber, and no added sugar.
Keto Champ GLP-1 in berry or chocolate: The Keto Champ contains Califia Farms® Almond Milk, almond butter, wild blueberries, raspberries, a Keto Protein Blend, and 100% Cocoa. A 20-ounce serving has 420 to 450 calories, 24 grams of protein, 14 to 15 grams of fiber, and no added sugar.
The Activator® Recovery GLP-1 Almond Berry: This smoothie contains strawberries, wild blueberries, Califia Farms® Almond Milk, coconut water, and Gladiator® Protein Strawberry. Twenty ounces of the Activator has 200 calories, 24 grams of protein, 5 grams of fiber, and zero added sugar.
Power Meal Slim™ GLP-1 in chocolate, strawberry, or vanilla: This GLP-1 smoothie contains bananas, Califia Farms® Almond Milk, Power Slim Protein, and 100% Cocoa. A 20-ounce serving has 190 to 210 calories, 19 to 22 grams of protein, 6 to 10 grams of fiber, and no added sugar.
An expert’s take on Smoothie King’s GLP-1 menu
While the new Ozempic-tailored smoothie options may look promising, there are no universally accepted official dietary recommendations for people taking GLP-1s. So, maintaining a healthy, well-balanced diet is still essential for people using these medications.
Nonetheless, Sandra Vigelienė, BSc, a health researcher at Healthnews, examined the ingredients in Smoothie King’s new GLP-1 smoothies to determine their nutritional value. Overall, the products may benefit people taking obesity drugs, but they should not be relied on as the sole source of nutrition.
Protein content
American dietary recommendations suggest that protein should comprise 10-35% of the total daily calorie intake. For a person consuming 2,000 kcal per day, that would equal around 46 grams.
Moreover, adequate protein intake may be critical for GLP-1 users, as some research suggests that ingesting protein may help suppress appetite and promote a sense of fullness.
Vigelienė’s investigation revealed that all GLP-1 smoothies on Smoothie King’s menu have high protein levels.
“Even a small serving of smoothie provides more than half or, in some cases, even exceeds daily protein intake recommendations just in one smaller serving,” Vigelienė says.
However, Vigelienė says it’s important to note that people using GLP-1 medication may already experience delayed gastric emptying and appetite suppression. So, a smoothie with high protein levels may exaggerate fullness, potentially promoting an uncomfortable feeling in the digestive tract.
Moreover, people with kidney conditions may want to watch protein intake since consuming too much protein can stress the kidneys, which may eventually lead to organ failure.
GLP-1 smoothies and fiber intake
While data is limited on fiber’s impact on GLP-1s, and it’s unclear how fiber may affect people using the medications, dietary guidelines suggest that people should get around 14 grams of dietary fiber per 1,000 kcal. This equals around 28 grams of dietary fiber for those consuming 2,000 kcal daily.
The fiber content in Smoothie King smoothies varies between one to 15 grams per 20-ounce serving.
“Compared to the dietary guidelines, some of the Smoothie King smoothies provide almost half of the daily recommended dietary fiber intake,” Vigelienė notes. “However, due to the high variation in dietary fiber per serving, those seeking to support their fiber intake should make sure to choose the smoothies that have a higher dietary fiber content.”
Is Smoothie King’s GLP-1 menu brand new?
People might assume that Smoothie King’s new GLP-1 smoothie menu differs from its other offerings.
However, Vigelienė found that some GLP-1 selections are identical to the company’s non-GLP-1 options.
Both smoothies have the same calories, fat, protein, sodium, carbohydrates, fiber, and sugar content. Moreover, they both contain a minimal amount of caffeine.
In addition, the company’s Power Meal Slim GLP-1 smoothie has the same ingredients and nutritional profile as their non-GLP 1 Power Meal Slim.
Still, the ingredients and nutritional values of the remaining Smoothie King GLP-1 smoothies differ from their non-GLP-1 counterparts.
While people taking Ozempic or similar drugs for weight loss could consume these and other nutrient-dense smoothies to boost their protein and fiber intake, they should do so with caution.
“Smoothies may be a convenient option to include in a healthy and balanced diet occasionally, balancing them with whole foods throughout the day,” Vigelienė says. “However, it is important to note that smoothies should not replace varied and balanced meals in the weight loss plan and may only be used as a part of the healthy diet.”
Credit: healthnews.com
Studies Show Health Benefits of Ozempic and Wegovy Go Beyond Weight Loss
Team Metabolic Health
New trials reveal that the popular diabetes and weight-loss drugs Ozempic and Wegovy can offer even more health benefits.
These two injected drugs are versions of semaglutide. In multiple new data analyses, the drugs appeared to cut people’s odds for heart failure and its complications, reduce deaths from COVID-19 and lower deaths from any cause.
Semaglutide is a member of family of drugs called GLP-1 agonists, which work by mimicking the effect of a natural hormone that helps reduce appetite, hunger and food intake.
The latest findings were presented Thursday in London at the annual meeting of the European Society of Cardiology (ESC) and published simultaneously in the Journal of the American College of Cardiology (JACC).
The data show that “these groundbreaking medications are poised to revolutionize cardiovascular care and could dramatically enhance cardiovascular health,” said Dr. Harlan Krumholz, JACC Editor-in-Chief and a professor of medicine at Yale University.
Some of the findings derive from sub-analyses of data from a major trial called SELECT, which included more than 17,000 people who were overweight or obese and had been diagnosed with heart disease, but not diabetes.
The trial was funded by semaglutide’s maker, Novo Nordisk, and in findings published in November it found that the 2.4 milligram (mg) dose of the drug cut the odds of heart-related deaths, heart attacks and strokes.
Credit: Dreamstime
In the two new subset analyses from SELECT, data showed that people taking semaglutide had a lower odds for death from all causes, compared to people who got a weekly placebo injection.
Another SELECT analysis looked at differences in outcomes based on patients’ gender. It found that women appeared to gain more of a heart-health benefit from the drug compared to men, but that both sexes did see reductions in terms of heart-related events.
Semaglutide also appeared to help shield users from the worst effects of COVID-19.
In a SELECT study data analysis, obese or overweight people who were taking the drug were infected with COVID at rates similar to those who were on placebo.
However, if they did get COVID, they were less likely to die from the disease if they had been taking semaglutide, the research showed.
Another study presented at the ESC meeting and published in the JACC focused on a major killer, heart failure.
This time, researchers looked at data from the FLOW trial, published in May and also funded by Novo Nordisk. That trial involved more than 3,500 people with type 2 diabetes and chronic kidney disease who got semaglutide or a placebo and were followed for an average of nearly 3.5 years. It found lower rates of kidney-related death in semaglutide users.
However, having both type 2 diabetes and kidney disease can raise a person’s odds for heart failure, a condition where the heart loses its ability to efficiently pump blood.
The new subset analysis found that people in the FLOW trial who got semaglutide at the 1 mg dose had lower odds for new-onset heart failure or hospitalization for heart failure, compared to those getting the placebo injection.
In addition, three sub-studies of what’s known as the STEP-HFpEF program looked at the effect of semaglutide (2.4 mgs) among obese people with heart failure.
According to a JACC news release, “semaglutide improved heart failure-related symptoms, physical limitations and exercise function and reduced body weight” in all patients.
The drug also reduced levels of inflammation based on measurements of a common blood marker called C-reactive protein (CRP), and these reductions occurred regardless of weight loss, the study found.
Heart failure is often accompanied by the irregular heartbeat known as atrial fibrillation (A-Fib). The study also found “even greater improvements in heart failure-related symptoms and physical limitations in those with vs. without A-Fib, though improvements were seen in both groups,” according to the news release.
Finally, the heart failure study showed signs that use of semaglutide effected positive, healthy changes in the heart’s structure and function, based on echocardiogram results.
Overall, “this portfolio of publications, derived from three major trials, significantly advances our understanding of the wide-ranging benefits of GLP-1 agonists,” Krumholz said.
Credit: healthday.com
Tout Savoir sur les Stéroïdes Anabolisants Légaux : Prix et Informations
Tout Savoir sur les Stéroïdes Anabolisants Légaux : Prix et Informations
Les stéroïdes anabolisants légaux prix sont un sujet de plus en plus discuté dans le monde du fitness et du bodybuilding. Ils sont souvent utilisés pour améliorer la performance physique et augmenter la masse musculaire. Dans cet article, nous allons explorer les différents aspects des stéroïdes anabolisants légaux, y compris leur coût, leur efficacité et leur utilisation.
Qu’est-ce que les Stéroïdes Anabolisants Légaux ?
Les stéroïdes anabolisants légaux sont des substances chimiques qui imitent l’action de la testostérone dans le corps. Contrairement aux stéroïdes illégaux, ceux-ci sont souvent fabriqués à des fins médicales et peuvent être prescrits par des médecins pour traiter certaines conditions médicales. Voici quelques caractéristiques clés :
- Utilisés pour traiter des maladies comme l’anémie ou la perte de poids.
- Aident à augmenter la masse musculaire et à améliorer la performance sportive.
- Sont souvent disponibles sous forme de comprimés, d’injections ou de gels.
Prix des Stéroïdes Anabolisants Légaux
Le prix des stéroïdes anabolisants légaux peut varier considérablement en fonction de plusieurs facteurs, notamment la marque, la qualité et le type de produit. Voici une estimation des coûts :
- Comprimés : Entre 30 et 120 euros par mois.
- Injections : Environ 50 à 200 euros par cycle.
- Gels : Généralement entre 40 et 100 euros par tube.
FAQ sur les Stéroïdes Anabolisants Légaux
Quels sont les avantages des stéroïdes anabolisants légaux ?
Les avantages incluent une augmentation significative de la force physique, une meilleure récupération après l’exercice, et une augmentation de la masse musculaire.
Y a-t-il des effets secondaires ?
Oui, même les stéroïdes anabolisants légaux peuvent avoir des effets secondaires, tels que des troubles hormonaux, des problèmes cardiovasculaires ou encore des troubles psychologiques.
Comment choisir un bon produit ?
Il est essentiel de faire des recherches approfondies et de consulter un professionnel de santé avant de commencer tout traitement avec des stéroïdes anabolisants. Vérifiez également les avis des utilisateurs et la réputation belgiqueanabolisants.com de la marque.
Conclusion
Les stéroïdes anabolisants légaux prix varient selon le type et la qualité des produits. Il est crucial de peser les bénéfices potentiels contre les risques associés à leur utilisation. Une consultation médicale est vivement recommandée pour garantir une utilisation sécuritaire et efficace.
Obesity Drug Shows Promise in Easing Knee Osteoarthritis Pain
Team Metabolic Health
A large trial showed that semaglutide, sold as Ozempic for diabetes and as Wegovy for obesity, was better than any current medications in alleviating symptoms.
The blockbuster drug semaglutide, sold as Ozempic for diabetes and as Wegovy for weight loss, now has a new proven benefit: It markedly soothed knee pain in people who are obese and have moderate to severe osteoarthritis, according to a large study.
The effect was so pronounced that some arthritis experts not involved with the clinical trial were taken aback.
“The magnitude of the improvement is of a scope we haven’t seen before with a drug,” said Dr. Bob Carter, deputy director of the National Institute of Arthritis and Musculoskeletal and Skin Diseases. “They had an almost 50 percent reduction in their knee pain. That’s huge.”
Dr. David T. Felson, an arthritis expert and professor of medicine at Boston University School of Medicine, said the study “changes the landscape,” adding that the pain reduction is greater than anything that can be achieved short of knee replacement surgery.
The results were published Wednesday in the New England Journal of Medicine.
Knee osteoarthritis affects nearly one in five Americans over the age of 45. Those with obesity are especially likely to develop it because their weight puts more stress on the knee and because obesity is associated with inflammation, which contributes to deterioration of cartilage.
There are no good medical treatments. Doctors can suggest patients take over-the-counter pain relievers like acetaminophen or ibuprofen. But long-term use of those medications can damage vital organs.
A study of 407 people with obesity and knee osteoarthritis found those who got semaglutide had an average reduction of 41.7 points on a 100-point scale while those who got the placebo had a reduction of 27.5 points. Credit: M. Scott Brauer for The New York Times
When the pain gets bad enough, many turn to knee replacement surgery.
“The good news is that surgery works for most people,” Dr. Carter said. “The bad news is that it is hugely expensive,” draining money from Medicare.
“We desperately need an effective way to treat knee pain,” he added.
In the 68-week study by Novo Nordisk, the maker of semaglutide, 407 people with obesity and knee osteoarthritis were randomly assigned to receive semaglutide in the form of Wegovy or a placebo. All patients also received exercise counseling and a reduced calorie diet.
The participants were mostly women. They had an average age of 56 and an average body mass index of 40.3, placing them firmly in the obesity category. They had to have knee pain and meet additional criteria for knee osteoarthritis like stiffness in the morning or knees that creaked or clicked when they walked. Their average pain on a 100-point scale was 70.9 at the start of the study.
“They were really in pain,” said Dr. Henning Bliddal, the principal investigator for the study and a rheumatologist at Copenhagen University Hospital. “They can’t exercise. You are trapped with knees like this.”
As expected, those who received semaglutide lost a significant amount of weight — an average of 13.7 percent of their starting weight — while those who got the placebo lost 3.2 percent of their starting weight.
The study’s primary outcome was a change in a standard measure called WOMAC, which assesses pain, physical functioning and stiffness on a 100-point scale. Those who got semaglutide had an average reduction of 41.7 points, while those who got the placebo had a reduction of 27.5 points.
Dr. Carter said that placebo participants often reported some degree of pain relief in studies. But, he added, the 41.7 point drop in the pain score of semaglutide participants “is huge.”
“To be frank, this is what we had hoped for,” Dr. Bliddal said. “But it even exceeded our expectations.”
Semaglutide controls blood sugar, curbs food cravings and reduces appetite. But it also has other effects — it reduces the risk of having a heart attack, stroke or cardiovascular death in people with heart disease, and it reduces the risk of kidney complications, heart issues and death in people with kidney disease.
Doctors and many patients have high hopes that the drugs can do much more, and they cite observational studies leading to clinical trials now underway testing the drugs for treating addiction, Parkinson’s disease, Alzheimer’s disease, depression and schizophrenia.
One potential reason for some of these effects — and a possible reason semaglutide helped people with knee osteoarthritis — is that the drug seems to quell inflammation, a central factor in a variety of diseases, including obesity and osteoarthritis.
Until fairly recently, investigators thought knee osteoarthritis was a mechanical problem. Cartilage wears down. The natural cushioning around the knee joint erodes. And heavier people are more at risk because their greater weight puts more strain on their joints.
But the more they studied arthritis, the more researchers discovered that mechanical damage may not be the only factor.
“The pain seemed out of proportion” to the damage actually observed in patients, said Dr. Felson, who wrote an editorial accompanying the study.
And the pain is not just because cartilage that lies over the bone gets worn down, Dr. Carter added.
In arthritis, the lining of a thin rim of cartilage that lies over the bone becomes inflamed and sends pain signals to the spinal cord.
The bone itself also contributes to the pain. With arthritis the knee bone changes, Dr. Carter said. Pores open in the bones that didn’t use to be there, and nerves from the bone grow into the base of the cartilage.
Now, with the new study, it looks as if there is a way to treat both the mechanical problem caused by excess weight and the other factors with just one very expensive drug.
But Dr. Carter is hopeful. If it could be learned what exactly semaglutide is doing inside the joint, perhaps researchers could develop drugs that do the same thing and cost less.
“We never really understood where the pain was coming from,” he said. Now, perhaps, there is a handle to figure it out.
Credit: The New York Times
GLP-1 drugs like Ozempic may protect brain health, several studies show
Team Metabolic Health
GLP-1 drugs such as Wegovy and Ozempic (semaglutide) and Zepbound (tirzepatide) may offer benefits that extend beyond aiding in weight loss in people who have type 2 diabetes or obesity.
A new review takes a look at how GLP-1 drugs may offer neuroprotective benefits.
Since obesity can cause chronic inflammation, including inflammation in the brain, it can also increase the risk of developing neurodegenerative diseases such as Alzheimer’s disease.
The study examines how GLP-1 medications reduce inflammation in the brain and how these drugs may be able to strengthen the blood-brain barrier.
The use of the medications Wegovy, Ozempic, and Zepbound has skyrocketed as people turn to GLP-1 medications to treat diabetes and obesity.
While these medications are mainly associated with improved insulin sensitivity and weight loss, researchers are learning that the benefits of these GLP-1 drugs may go well beyond these effects.
In addition to research on how GLP-1 drugs may help with addiction and lower risk for certain cancers, a new review shines a light on how this class of medications may provide some degree of brain health protection.
The review examines how GLP-1 drugs can balance the neurovascular unit — the part of the brain that regulates blood flow within the brain — thereby creating the possibility of improving cognitive functioning.
The review appears in the journal Cell Metabolism.
Are GLP-1 drugs good for brain health? Accumulating evidence seems to suggest so. Image credit: Popartic/Getty Images
How does obesity affect cognitive function?
According to the Centers for Disease Control and Prevention (CDC), just over 40% of adults in the United States have obesity, which is defined as having a body mass index (BMI) of 30 or higher.
Obesity can increase the risk for a host of health issues including heart disease, sleep apnea, and type 2 diabetes.
Obesity also causes chronic low-grade inflammation. This type of inflammation affects the entire body, including the brain.
Chronic low-grade inflammation can contribute to insulin resistance, cause fatigue, and can cause achiness throughout the body. Insofar as the brain is concerned, chronic low-grade inflammation can impact cognitive functioning.
Recent research indicates that obesity and chronic low-grade inflammation are a “pathway” to developing Alzheimer’s disease. As scientists continue working to find ways to prevent and slow the progression of neurodegenerative diseases, the category of GLP-1 drugs has become a focus of research.
Researchers describe GLP-1 as a hormone naturally produced in the gut and the brain. The healthcare providers of people with either type 2 diabetes or obesity may opt to treat them with GLP-1 receptor agonist drugs (GLP-1 drugs) to assist with weight loss.
This class of drugs works by slowing down gastric emptying, lowering blood sugar levels, and improving satiety. These medications can also help improve metabolism.
Many people who take a GLP-1 medication experience a “clinically significant” amount of weight loss. This weight loss can help in many areas such as improving heart health, reducing the risk of developing cancer, and increasing energy levels.
How GLP-1 drugs may protect the brain
The benefits of GLP-1 medications are not limited to only weight loss and improved heart health. More studies are revealing that these drugs can also improve brain health.
Chronic low-grade inflammation can impact the brain by affecting glial cell functioning. Glial cells include:
Astrocytes, which perform neuroprotective tasks and form the blood-brain barrier
Microglia, which are immune cells that sustain the blood-brain barrier and remove damaged cells in the brain, but changes in which can lead to neurodegeneration.
The blood-brain barrier is especially important since it protects the brain from harmful substances and infection. Inflammation in people with obesity may result in reductions in their blood-brain barriers.
The review addresses how research shows that cell signaling from GLP-1 drugs may interact with these cells and provide brain health benefits.
The review authors noted that a study in mouse models showed the GLP-1 drug liraglutide (Victoza) increased the number of astrocytes.
According to the review, “[GLP-1 receptor] signaling in astrocytes regulates both central and peripheral metabolism, extending from energy balance to neuroplasticity.”
This signaling also enhances neuron growth, and an increase in astrocytes also increases neuron survival.
Another study the review mentioned tested a GLP-1 medication on mice with the neurodegenerative eye disease glaucoma, and found a reduction in “astrocyte transformation and retinal ganglion cell death.”
With microglia, the review shows that some studies believe GLP-1 receptor signaling can reverse inflammation.
“GLP-1R signaling on microglia attenuates neuroinflammation by suppressing the polarization of microglia to a proinflammatory state,” wrote the authors.
If inflammation in the brain could be reversed, this could be especially helpful in neurodegenerative diseases.
The review authors noted that research into the potential brain benefits of GLP-1 medications needs more research but are optimistic about the future of these drugs in how they may boost brain health.
Is treating Alzheimer’s disease with semaglutide on the horizon?
David Hunter, MD, an associate professor of neurology at UTHealth Houston, not involved in this review, spoke with Medical News Today about its findings.
“Decades of research into Alzheimer’s disease [have] shown that inflammation is a key step in disease pathology,” he told us.
Hunter explained how Alzheimer’s disease begins with amyloid plaques and explained that microglia “play a role in the steps that lead to brain cells dying.”
The doctor also said that different trials are just to see how well GLP-1 drugs can help treat Alzheimer’s disease and that “the drug that is closest to FDA [Food and Drug Administration] approval is semaglutide.”
Hunter expected that UTHealth’s own EVOKE trial will announce results on the use of semaglutide for Alzheimer’s in the fall of 2025.
José Morales, MD, a vascular neurologist and neurointerventional surgeon at Providence Saint John’s Health Center in Santa Monica, CA, also not involved in this review, told MNT that “microglia’s effect on the neurovascular unit has been associated with dementia.”
Morales also explained that in people who have glycemia or type 2 diabetes, the inflammation of the blood-brain barrier can “lead to progressive damage to the brain over longer periods.”
He noted that trials that combine neuroimaging techniques that measure the blood-brain barrier and GLP-1 treatment are needed and could prove that these drugs have neuroprotective benefits.
Credit: medicalnewstoday.com
Ultra-processed food linked to weight gain and lower well-being in adolescents
Team Metabolic Health
New research examines the impact of ultra-processed food, screen time, and maternal education on weight and well-being in adolescents.
In a recent study published in Nutrients, a group of researchers compared ultra-processed food (UPF) consumption, sedentary behaviors, and well-being between adolescent boys and girls and investigated their associations with overweight risk.
Background
Pediatric obesity is a growing public health concern linked to dietary behaviors and sedentary lifestyles, notably the increased consumption of UPFs among adolescents. UPFs, rich in added sugars, unhealthy fats, and additives but low in essential nutrients, contribute to excessive caloric intake and unfavorable metabolic outcomes.
Sedentary behaviors aggravate this issue and are particularly prevalent in Western countries and Southern Europe.
Precise assessment tools are needed to evaluate UPF consumption and its impact on obesity and well-being in youth, including potential associations with mental health. Further research is necessary to understand these relationships and develop effective interventions.

Study: Ultra-Processed Food Consumption and Its Association with Risk of Obesity, Sedentary Behaviors, and Well-Being in Adolescents. Image Credit: KatMoys/Shutterstock.com
About the study
A total of 245 adolescents (131 boys and 114 girls), aged 12 to 17 years (mean age 14.20 ± 1.09), were recruited from two randomly selected public high schools in the Coimbra (n = 101) and Viseu (n = 144) districts.
Anthropometric measurements, including height, weight, and body fat percentage using bioelectrical impedance, were collected to calculate body mass index (BMI), which was classified according to International Obesity Task Force guidelines.
UPF consumption was assessed using the NOVA-UPF screener, a questionnaire evaluating UPF intake on the previous day. Sedentary behaviors were self-reported, detailing time spent on activities like watching TV and using electronic devices during weekdays and weekends.
Well-being was measured using the Mental Health Continuum-Short Form and the physical well-being subscale of the KIDSCREEN-27 questionnaire. Parental education levels served as proxies for socioeconomic status.
Statistical analyses included descriptive statistics, t-tests, correlations, and logistic regression, controlling for confounders such as age, sex, sedentary behavior, parental BMI, and education. The study adhered to the Declaration of Helsinki, received ethical approval from relevant authorities, and obtained informed consent from participants and their guardians.
Study results
In the study involving 245 Portuguese adolescents aged 12 to 17 years (mean age 14.2 ± 1.09 years), researchers examined UPF consumption, sedentary behaviors, and well-being, focusing on differences between sexes. The sample comprised 131 boys and 114 girls.
Among the girls, 17.5% were categorized as overweight and 7.9% as obese; among the boys, 15.3% were overweight and 3.1% were obese.
The findings indicated that adolescents consumed similar levels of UPFs across the three food subcategories of the NOVA screener, regardless of whether the consumption was based on a 24-hour recall or occurred outside the home.
During weekdays, the most common sedentary activities were smartphone use, studying, and using a personal computer (PC). On weekends, adolescents reported spending more time using smartphones and PCs, as well as watching television.
No significant differences were observed between boys and girls in UPF consumption across different subcategories. However, girls exhibited higher BMI levels and body fat percentages than boys, with both differences being statistically significant (p < 0.001).
Boys reported higher levels of PC use during weekends (p = 0.025) and spent more time playing electronic games during both weekdays (p = 0.005) and weekends (p < 0.001) compared to girls.
Conversely, girls spent more time studying during weekdays (p = 0.006) and weekends (p = 0.007), and engaged more in activities like board games or reading during weekends (p = 0.026) than boys. Additionally, boys scored higher in all dimensions of well-being (p < 0.001) compared to girls.
Correlation analyses revealed that the 24-hour recall consumption of UPFs, including sugary drinks and yogurts, was positively associated with watching the TV on weekends, playing electronic games, and using weekday smartphones. It was negatively associated with body fat percentage and time spent studying during both weekdays and weekends.
Similarly, the consumption of UPFs like sugary drinks and yogurts outside the home was positively associated with total sedentary time during weekends and negatively associated with body fat percentage and weekend study time.
A similar pattern emerged for the 24-hour recall consumption of packaged and fast food UPFs, which showed positive correlations with weekday television watching and weekend smartphone use and negative correlations with body fat percentage.
The consumption of sweet and salty snack UPFs outside the home was negatively associated with body fat percentage. Importantly, no significant relationships were found between UPF consumption and any dimensions of well-being among the adolescents.
Logistic regression analyses, controlling for variables such as age, sedentary behaviors, sex, parental BMI, and parental education, indicated that UPF consumption tended to be associated with an increased risk of being overweight. However, this association was marginally significant (p = 0.06 to 0.09).
Notably, adolescents whose mothers had higher educational levels were less likely to be classified as overweight or obese (odds ratio = 0.83, 95% CI: 0.70–0.98, p = 0.02). Additionally, increased PC use during weekends was associated with a higher likelihood of being overweight (odds ratio = 0.99, 95% CI: 0.98–1.00, p = 0.04).
Conclusions
To summarize, the study found no gender differences in UPF consumption, mirroring some international findings. Although UPF consumption was marginally associated with a higher risk of being overweight, it was significantly linked to increased sedentary behaviors such as screen time.
Adolescents with mothers who had higher educational levels were less likely to be overweight or obese. No significant associations were observed between UPF consumption and well-being dimensions.
These findings underscore the complex interplay of dietary habits, sedentary behavior, and socio-economic factors in adolescent obesity.
Credit: news-medical.net
One Type of Fiber May Have Weight Loss Benefits Similar to Ozempic
Team Metabolic Health
Research on the gut microbiome has triggered a ‘revolution’ in nutritional science, and in the last few years, dietary fiber has become the “new protein” – added to foods in abundance to feed our gut and boost our health.
A recent study on mice, however, suggests not all fiber supplements are equally beneficial.
A form that is readily found in oats and barley, called beta-glucan, can control blood sugar and assist in weight loss among mice fed a high-fat diet.
Researchers at the University of Arizona (UA) and the University of Vienna say it is the only type of fiber supplement they tested that decreased a mouse’s fat content and body weight within 18 weeks.

(Courtneyk/Getty Images)
The other fibers considered, including wheat dextrin, pectin, resistant starch, and cellulose, had no such effect, despite shifting the makeup of the mouse microbiome significantly compared to mice fed no fiber supplements.
“We know that fiber is important and beneficial; the problem is that there are so many different types of fiber,” explained biomedical scientist Frank Duca from UA in July.
“We wanted to know what kind of fiber would be most beneficial for weight loss and improvements in glucose homeostasis so that we can inform the community, the consumer, and then also inform the agricultural industry.”
Dietary fibers are the main source of energy for bacteria living in our guts, and yet less than 5 percent of people in the US consume the recommended 25–30 grams (0.9–1 ounce) of fiber a day.
To make up for this, fiber supplements and ‘invisible fiber’-infused foods are growing in popularity. But fibers are extremely diverse, so which do we choose?
Some fibers, like oat beta-glucans and wheat dextrin, are water-soluble, meaning they are easily fermented by gut bacteria. Others, like cellulose and resistant starch, are less soluble or insoluble, meaning they stick to other materials to form stool.
(Imyskin/Getty Images)
Until now, writes biomedical scientist Elizabeth Howard from UA and her colleagues, “there is no study that has investigated the role of various fibers in one cohort.”
To make up for this, the current study tested several forms of fiber in one cohort of mice. Only beta-glucan was found to increase the number of Ileibacterium found in the mouse intestine. Other studies on mice have linked this bacterium to weight loss.
Sure enough, long before the 10-week marker, mice fed beta-glucan showed reduced body weight and body fat content compared to mice fed other forms of fiber.
The findings align with another recent study by Duca, which fed barley flour, rich in beta-glucan, to rodents. Even though the rats continued eating just as much of their high-fat diet as before, their energy expenditure increased and they lost weight anyway.
A similar outcome was observed in mice fed beta-glucan in the new study. These animals also showed increased concentrations of butyrate in their guts, which is a metabolite made when microbes break down fiber.
Butyrate induces the release of glucagon-like peptide-1 (GLP-1), which is the natural protein that synthetic drugs like Ozempic mimic to stimulate insulin release.
“Part of the benefits of consuming dietary fiber is through the release of GLP-1 and other gut peptides that regulate appetite and body weight,” said Duca.
“However, we don’t think that’s all of the effect. We think that there are other beneficial things that butyrate could be doing that are not gut peptide related, such as improving gut barrier health and targeting peripheral organs like the liver.”
Far more research is needed before these results can be extended to humans, but the findings suggest that some fibers may be better suited to weight loss and insulin control than others.
Credit: sciencealert.com
Weight-Loss Surgeries Drop 25 Percent As Americans Opt For GLP-1 Medications
Team Metabolic Health
A study shows a 25.6 per cent decline in weight-loss surgeries as more Americans turn to GLP-1 medications like Wegovy and Zepbound. Despite their popularity, high costs and side effects may lead to treatment discontinuation.
A new report indicates that the increasing popularity of GLP-1 medications, such as Wegovy and Zepbound, is leading to a significant reduction in weight-loss surgeries among Americans. The report highlights that prescriptions for this class of diabetes and weight-loss medications more than doubled from 2022 to 2023.
Led by Dr. Thomas Tsai, an assistant professor of surgery at Harvard Medical School in Boston, the study found a notable 25.6 per cent decline in patients opting for metabolic bariatric surgery during the same period. This trend coincides with the U.S. Food and Drug Administration’s approval of Wegovy in mid-2021, the first GLP-1 medication specifically designed for weight loss. Following this approval, sales of Wegovy and similar drugs, including Ozempic, Mounjaro, and Zepbound, have surged dramatically.
Weight-Loss Surgeries Drop 25 Percent As Americans Opt For GLP-1 Medications (Image Credits: iStock)
These GLP-1 medications have been recognized for their effectiveness in promoting rapid weight loss by inducing a sense of fullness, leading patients to consume fewer calories. Prior to the introduction of these medications, Americans seeking to lose weight primarily relied on diet and exercise or surgical options. However, the advent of the “Ozempic era” appears to be reshaping the landscape of weight-loss treatments, according to Tsai’s team. They observed that some health systems have even closed hospital-based metabolic bariatric surgery programs due to decreased demand for such procedures.
To analyze these trends more quantitatively, the researchers examined medical records from over 17 million Americans insured through private plans or Medicare Advantage, all of whom were non-diabetic but classified as obese. The study tracked prescription trends for GLP-1 medications used for weight loss during the last six months of 2022 and 2023, alongside the rates of bariatric surgery in the same time frame.
The findings reveal that prescriptions for GLP-1 medications rose by 132.6 per cent, while rates of bariatric surgery decreased by 25.6 per cent. However, the study raises questions about the sustainability of these trends. While medications like Wegovy and Zepbound are effective, Tsai and his colleagues warn that their high cost and gastrointestinal side effects may lead to treatment discontinuation and potential weight regain.
Additionally, the demand for weight-loss medications has exceeded supply, suggesting that if the ongoing national shortages of GLP-1s continue, the number of patients turning to weight-loss surgery might rise again. In light of these observations, Tsai’s team emphasizes the importance of policymakers and clinicians closely monitoring the balance between pharmacological and surgical approaches to obesity management, ensuring optimal access to effective treatments.
Credit: timesnownews.com
New 3D body scan method beats traditional imaging for tracking body fat
Team Metabolic Health
A novel 3D body shape method promises accessible and accurate body composition predictions, potentially transforming how we monitor health over time and detect risks.
In a recent study published in the journal npj Digital Medicine, researchers developed a novel method to predict body composition for three-dimensional (3D) body shapes. Body composition is linked to chronic disease risk. It can be assessed using computed tomography, dual-energy X-ray absorptiometry (DXA), and magnetic resonance imaging. However, due to ethical and practical constraints, these techniques are not readily available in epidemiological studies and clinical practice and are not easily accessible to the general public.
Conventional anthropometrics, such as waist-hip ratio, body mass index (BMI), and waist-hip circumferences, are used to infer body composition. Nevertheless, these methods do not differentiate between lean and fat mass and are inadequately accurate/convenient for longitudinal use, often requiring trained personnel and in-person visits. Thus, simple, accessible, inexpensive tools are needed to assess body composition accurately.
About the study
In the present study, researchers developed a novel method for body composition prediction using 3D body shape. They obtained DXA scans, metabolic health variables, and paired anthropometry data from the Fenland study established in 2005. The Fenland study involved 12,435 participants in Phase I and 7,795 in Phase II. Of these, 11,359 participants from Phase I and 6,102 from Phase II were included in the current study.
The team used 80% of Phase I data to train and derive 3D body shape composition models, and the remainder was used for validation. Phase II data were used as a test dataset for validation in a now older population. Moreover, a smartphone validation study was undertaken with 119 healthy adults, which, besides DXA scans, included air plethysmography and a mobile app capturing images. This sample was used to validate models derived from the Fenland study and assess the accuracy of 3D shapes obtained from smartphone images. Statistical validation metrics, including Pearson correlation coefficients and root-mean-square error (RMSE), were employed to measure the accuracy of these predictions.
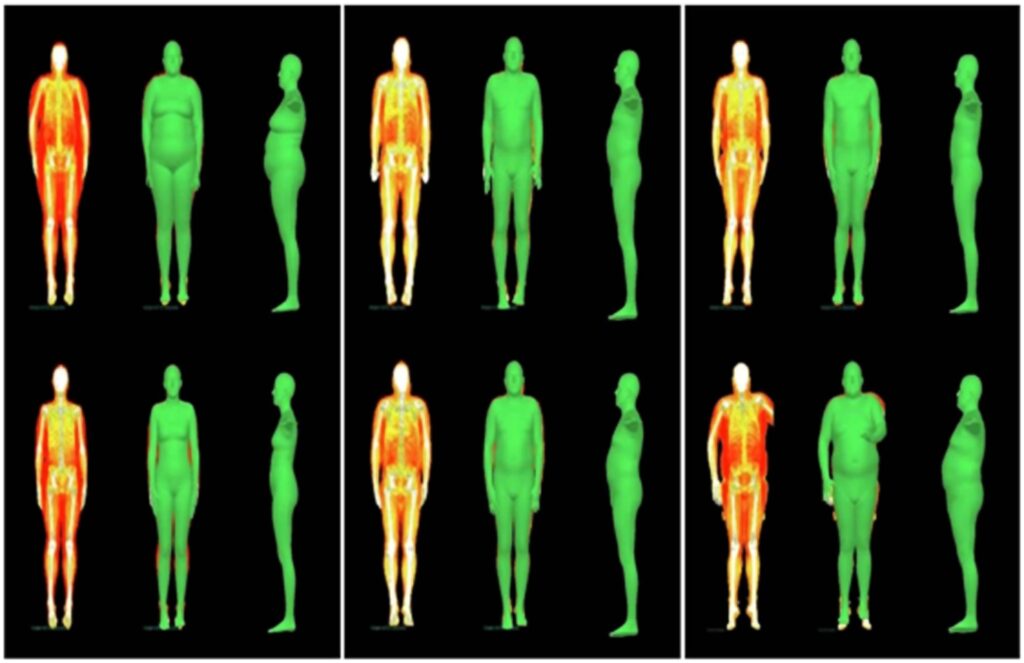
Each three columns shows one participant who lost (Columns 1–3), maintained (Columns 4–6) or gained (Columns 7–9) fat mass, their DXA scans and fitted meshes for Fenland phase 1 (Row 1) and phase 2 (Row 2). Changes in body shape for the first and third participants are significant.
2D images of the front, back, right-side, and left-side profiles were taken using a purpose-built mobile app that constructs a 3D body mesh. The researchers fitted 3D body meshes to DXA silhouettes with paired anthropometry measures, and the fitted parameters were used for predicting body composition metrics. To fit a 3D mesh, DXA silhouettes were augmented with paired anthropometrics using the skinned multi-person linear (SMPL) model in a two-stage approach.
First, the hierarchical kinematic probability distributions (HKPD) method was used for initial pose and shape estimates. Next, an optimization method was developed to refine this initial guess. Optimized SMPL shape parameters were used to regress body composition metrics. A feed-forward neural network was constructed for regression, which used 10 SMPL shape parameters, height, weight, gender, and BMI as the input. The network outputs included total lean mass, total fat mass, etc. Further, the HKPD method generated SMPL avatars using multi-view information from smartphone images. A model was developed to predict regional and total body composition metrics using these methods. Its performance was evaluated using root-mean-square error values. The associations between predicted values and DXA measurements were assessed using Pearson correlation coefficients.
Findings
The smartphone validation study participants were younger, leaner, and lighter than those in the Fenland study. The researchers noted that the optimized meshes agreed with the DXA silhouette much better than the initial shape and pose estimates. In the Phase I sample of the Fenland study, correlation coefficients between DXA and predicted parameters were robust for all lean and fat mass variables. Similarly, correlation coefficients were strong for all variables in the Phase II sample.
In addition, comparable results were observed in the external validation sample. The Pearson correlation coefficients exceeded 0.86 for most metrics, indicating strong agreement between predicted and DXA values. Further, a comparison study was conducted on different regressor model inputs. One model, which used only height and weight as inputs, showed some predictive ability. Performance increased by including waist and hip circumferences, respectively. The final model, which used SMPL, height, and weight as inputs, showed substantial improvements in estimating body composition metrics. The model demonstrated a root-mean-square error (RMSE) of less than 3.5% for percentage body fat predictions, highlighting its accuracy.
In the Fenland study, 5,733 individuals participated in both phases, allowing for the evaluation of the model’s ability to detect changes in body composition over an average of 6.7 years. The model detected changes for various fat mass metrics; lean mass changes were less well captured, mainly because lean mass remains essentially unchanged over time.
Conclusions
The researchers introduced a novel computer vision-based method fitting a 3D body mesh to a DXA silhouette with paired anthropometric data and generated a database of 3D body meshes. These meshes accurately predicted body composition metrics. Moreover, the model could detect longitudinal changes. However, the researchers noted that while the model was particularly effective at detecting changes in fat mass, its ability to track changes in lean mass was more limited, due to the stability of lean mass over time.
The team also illustrated that avatars generated from smartphone images could be used for body composition prediction. Overall, 3D body shapes generated from 2D images and relevant inference methods could be a viable alternative for clinical medical imaging. The study acknowledges the demographic limitations of the dataset, which predominantly included white European adults, suggesting further research in diverse populations for broader applicability.
Credit: mews-medical.net
Studies Show Health Benefits of Ozempic and Wegovy Go Beyond Weight Loss
Team Metabolic Health
New trials reveal that the popular diabetes and weight-loss drugs Ozempic and Wegovy can offer even more health benefits.
These two injected drugs are versions of semaglutide. In multiple new data analyses, the drugs appeared to cut people’s odds for heart failure and its complications, reduce deaths from COVID-19 and lower deaths from any cause.
Semaglutide is a member of family of drugs called GLP-1 agonists, which work by mimicking the effect of a natural hormone that helps reduce appetite, hunger and food intake.
The latest findings were presented Thursday in London at the annual meeting of the European Society of Cardiology (ESC) and published simultaneously in the Journal of the American College of Cardiology (JACC).
Credit: Dreamstime
The latest findings were presented Thursday in London at the annual meeting of the European Society of Cardiology (ESC) and published simultaneously in the Journal of the American College of Cardiology (JACC).
The data show that “these groundbreaking medications are poised to revolutionize cardiovascular care and could dramatically enhance cardiovascular health,” said Dr. Harlan Krumholz, JACC Editor-in-Chief and a professor of medicine at Yale University.
Some of the findings derive from sub-analyses of data from a major trial called SELECT, which included more than 17,000 people who were overweight or obese and had been diagnosed with heart disease, but not diabetes.
The trial was funded by semaglutide’s maker, Novo Nordisk, and in findings published in November it found that the 2.4 milligram (mg) dose of the drug cut the odds of heart-related deaths, heart attacks and strokes.
In the two new subset analyses from SELECT, data showed that people taking semaglutide had a lower odds for death from all causes, compared to people who got a weekly placebo injection.
Another SELECT analysis looked at differences in outcomes based on patients’ gender. It found that women appeared to gain more of a heart-health benefit from the drug compared to men, but that both sexes did see reductions in terms of heart-related events.
Semaglutide also appeared to help shield users from the worst effects of COVID-19.
In a SELECT study data analysis, obese or overweight people who were taking the drug were infected with COVID at rates similar to those who were on placebo.
However, if they did get COVID, they were less likely to die from the disease if they had been taking semaglutide, the research showed.
Another study presented at the ESC meeting and published in the JACC focused on a major killer, heart failure.
This time, researchers looked at data from the FLOW trial, published in May and also funded by Novo Nordisk. That trial involved more than 3,500 people with type 2 diabetes and chronic kidney disease who got semaglutide or a placebo and were followed for an average of nearly 3.5 years. It found lower rates of kidney-related death in semaglutide users.
However, having both type 2 diabetes and kidney disease can raise a person’s odds for heart failure, a condition where the heart loses its ability to efficiently pump blood.
The new subset analysis found that people in the FLOW trial who got semaglutide at the 1 mg dose had lower odds for new-onset heart failure or hospitalization for heart failure, compared to those getting the placebo injection.
In addition, three sub-studies of what’s known as the STEP-HFpEF program looked at the effect of semaglutide (2.4 mgs) among obese people with heart failure.
According to a JACC news release, “semaglutide improved heart failure-related symptoms, physical limitations and exercise function and reduced body weight” in all patients.
The drug also reduced levels of inflammation based on measurements of a common blood marker called C-reactive protein (CRP), and these reductions occurred regardless of weight loss, the study found.
Heart failure is often accompanied by the irregular heartbeat known as atrial fibrillation (A-Fib). The study also found “even greater improvements in heart failure-related symptoms and physical limitations in those with vs. without A-Fib, though improvements were seen in both groups,” according to the news release.
Finally, the heart failure study showed signs that use of semaglutide effected positive, healthy changes in the heart’s structure and function, based on echocardiogram results.
Overall, “this portfolio of publications, derived from three major trials, significantly advances our understanding of the wide-ranging benefits of GLP-1 agonists,” Krumholz said.
Credit: healthday.com
Study reveals liver-brain communication as key to managing circadian eating patterns and obesity
Team Metabolic Health
Research highlights the hepatic vagal nerve’s role in regulating food intake rhythms, offering new insights for potential anti-obesity treatments.
A recent Science study found that communication between the hepatic vagal afferent nerve (HVAN) and the brain influences circadian eating patterns. In mice, surgical HVAN removal corrected altered food intake and reduced weight gain from high-fat diets, suggesting HVAN could be a target for anti-obesity treatments.
Background
Circadian rhythms are 24-hour cycles regulating physical, mental, and behavioral changes in animals, typically aligned with light and dark cycles. While usually stable, these rhythms can be disrupted by changes in behavior or light exposure, as seen with jetlag or shift work, leading to desynchrony between organ systems.
The suprachiasmatic nucleus (SCN) serves as the master circadian clock, using light cues to establish feedback loops (TTFLs) of molecular-clock genes. Recent findings show that almost all somatic cells also maintain their own TTFLs, which help balance circadian rhythms with other processes, like food intake.
Synchrony between the SCN and food-entrained liver rhythms is crucial for maintaining metabolic balance amidst environmental changes. Studies in both rodents and humans suggest that desynchrony between these systems harms’ health, increasing the risk and severity of metabolic disorders like obesity and diabetes. However, the precise mechanisms and signals driving these interactions remain unclear.

Study: Hepatic Vagal Afferents Convey Clock-Dependent Signals to Regulate Circadian Food Intake. Image Credit: alexkich/Shutterstock.com
About the study
The present study investigates the mechanisms of circadian rhythm-establishing communication between the liver and the brain by deleting REV-ERBα/β nuclear receptors in murine model systems.
These nuclear receptors have previously been identified as central regulatory components of chrono-metabolic homeostasis. Consequently, their deletion induces desynchrony.
Contrasting previous investigations in the field, researchers used tail vein injections of REV-ERB deletion-capable adenoviruses, providing the present study with the unique advantage of location-specific (rather than system-wide) clock disruptions.
Specifically, this study methodology allowed for the observation and manipulation of asynchrony between the liver and the brain while leaving other organ systems unaltered, thereby substantially reducing background noise and confounding results.
Surgical and experimental interventions were carried out on three different cohorts of adult laboratory mice – C57Bl/6J, Nr1d1fl/fl/Nr1d2fl/fl, and Arntlfl/fl.
Outcomes under investigation include changes in gene expression between control (sham surgery) and case (HepDKO) mice and comparisons between their respective body weight gains during the study period.
The study additionally focused on the role of the hepatic vagus nerve (HV) in brain signaling and weight modulation. While previously known to serve as a transmission center for supplying the brain with liver metabolic data, HV’s explicit role in circadian communication and food intake rhythms remains hypothetical.
The present study explores HV’s role via the surgical removal of surgical ablation of HV in case mice and the subsequent comparisons of their weight gain with controls under diet-induced obesity (DIO) conditions.
Study findings
The present study emphasizes the role of food intake as a zeitgeber (an external cue that synchronizes biological rhythms) for circadian modulation in the liver, similar to how light-dark cycles serve as the zeitgeber for SCN-driven circadian rhythms across the body.
This means that daily cycles of hunger and satiation don’t necessarily need to match light-dark cycles; each rhythm operates independently based on its cue (food or light), with liver-brain communication maintaining balance between them.
In gene knockdown mouse models, deleting REV-ERBα and REV-ERBβ nuclear receptors disrupted food intake rhythms without affecting SCN-regulated cycles.
This deletion activated clock genes Arntl and Per2, known for their role in chrono-metabolic balance, leading to altered food intake patterns and increased eating during light periods, ultimately causing significant weight gain. Interestingly, severing the hepatic vagal afferent nerve (HVAN) reversed these effects, reducing food intake and resulting in weight loss.
This highlights HV’s crucial role in brain signaling for food-driven rhythms, with parallel studies showing contrasting outcomes: activating gut signaling afferents in humans led to weight loss, underscoring the complexity of gut-brain interactions in metabolic regulation.
Conclusions
The present study used murine model systems to identify the mechanisms underpinning chrono-metabolic homeostasis and corresponding food intake dysregulation.
Study findings revealed that the HV serves as a communication and signaling center, informing the brain of alterations in food intake rhythms detected via REV-ERBα/β nuclear receptors. This signaling results in increased light-cycle food intake and substantial weight gain.
Ablation of the HV was observed to reverse these effects, pinpointing it as a target in future weight loss research.
Credit: news-medical.net
Amgen dismisses bone density concerns related to its weight-loss drug
Team metabolic Health
Amgen (AMGN.O), has said that there was no link between its experimental weight-loss drug and changes in bone density, a day after those concerns wiped off more than $12 billion from the company’s market value.
The drugmaker’s stock slumped 7% on Tuesday after analysts at Cantor Fitzgerald said their review of early-stage data on Amgen’s MariTide showed a drop in bone mineral density, which can increase the risk of fractures.
But Amgen said “the Phase 1 study results do not suggest any bone safety concern or change our conviction in the promise of MariTide.” It plans to report data from its mid-stage study later this year.
Amgen’s shares rose 1.8% in early trading.
Investors are keenly awaiting more data on a drug seen as a contender in the estimated $150 billion market for weight-loss treatments.
Amgen shares react to obesity-drug
Cantor analysts said they found the bone mineral density changes when reviewing supplemental data that was published along with the results in February.
But at least four analysts said the concerns were overblown, since the company was conducting a mid-stage study and planned a larger late-stage trial.
A new safety signal would certainly cause alarm, but Amgen knows much more about MariTide than Wall Street, Piper Sandler analyst Christopher Raymond said in a note.
MariTide activates the GLP-1 hormone associated with the feeling of fullness, similar to popular weight-loss drugs such as Novo Nordisk’s (NOVOb.CO), Wegovy and Eli Lilly’s (LLY.N), Zepbound. MariTide also blocks the activity of another gut hormone called GIP, which has been linked to fat storage.
Amgen, one of the several companies developing weight-loss drugs, hopes the different approach will provide quicker weight loss and less frequent dosing compared to Wegovy and Zepbound.
MariTide cut weight by 14.5% in the 49-patient early-stage trial, according to the data, published in Nature Metabolism journal in February.
Credit: Reuters
Community-led intervention curbs childhood obesity and boosts quality of life
Team Metabolic Health
A new study finds that empowering communities with systems-based tools to fight childhood obesity not only reduced weight trends but also improved quality of life in boys—suggesting a resilient, community-first approach to lasting health changes.
The RESPOND randomized trial is a community-based systems intervention to prevent childhood obesity and non-communicable diseases.
Scientists at Deakin University recently evaluated the trial’s three-year behavioral, health-related quality of life, and body mass index outcomes. The study is published in the journal Public Health.
Background
Childhood obesity is a serious public health concern as it often persists into adulthood and increases the risk of several non-communicable diseases.
The complex and multifactorial nature of childhood obesity risk factors may lead to resistance to intervention. This complexity includes multiple factors that can influence a child’s food consumption, including early-life exposure to a variety of foods, food availability at home and within the community, and socioeconomic status.
Existing evidence indicates that multi-level interventions that apply multiple strategies across communities can significantly reduce children’s body weight.
Systems science and systems thinking are methods of understanding the relationships and connections between component factors driving complex systems. Thus, they can provide promising and innovative interventions to prevent childhood obesity.
The Reflexive Evidence and Systems Interventions to Prevent Obesity and Non-communicable Disease (RESPOND) trial was initiated to examine whether building the capacity of key community health staff at scale through systems-based training can develop a sustainable model for delivering such interventions for childhood obesity prevention.
In this study, scientists have evaluated the impact of the RESPOND trial on BMI z-scores (standardized body mass index), health-related quality of life, and related behaviors.

Study: Three-year behavioural, health-related quality of life, and body mass index outcomes from the RESPOND randomized trial. Image Credit: chanchai plongern/Shutterstock
Study Design
RESPOND was designed as a four-year randomized childhood obesity prevention trial involving 10 local government areas in northeast Victoria, Australia. The aim was to build community capacity to apply systems science to prevent childhood obesity and non-communicable diseases.
The intervention was initially implemented in the selected areas in July 2019 (step one) or July 2021 (step two). Baseline child-level data were collected between March and June 2019, and the follow-up data collection was planned for 2021 and 2023.
Due to the COVID-19 pandemic, however, step two communities could not begin their intervention as planned and were therefore treated as controls.
The step one communities partially implemented the intervention actions and were defined as “intervention communities.” The trial was altered to a cluster-parallel randomized design, allowing the researchers to compare outcomes in intervention and control communities.
In this study, scientists compared intervention versus control communities over three years (2019–2022). The study analyzed data obtained from 31 primary schools that participated in both March to June 2019 and March to August 2022 data collection waves.
The three-year outcomes included BMI z-scores, health-related quality of life, and self-reported health behaviors.
Important Observations
The analysis conducted within intervention communities revealed a small reduction in BMI z-scores and the percentage of overweight or obesity from 2019 to 2022. Within control communities, a small increase in BMI z-scores and the percentage of overweight or obesity was observed during the same period.
Self-reported health behaviors revealed limited effects of the intervention on any analyzed outcomes (physical activity, recreational screen time, and frequency of takeaway food consumption). However, a noteworthy intervention effect on daily water consumption was observed in boys.
Between 2019 and 2022, overall health-related quality of life deteriorated for children, likely due to COVID-19-related challenges. However, for boys, a significant improvement in quality of life and psychosocial health was observed within intervention communities.
Study Significance
The study finds a limited but positive effect of the community-based systems intervention (RESPOND) on psychosocial health, overall quality of life, and water consumption among boys who participated in the trial. However, the intervention had no significant impact on these metrics for girls.
The study also finds a general decline in several obesity-related behaviors among boys and girls in both intervention and control communities over the study period, which researchers attribute in part to the pandemic’s impact on lifestyle behaviors.
A non-significant but favorable effect of the intervention has been observed for BMI z-scores, overweight or obesity prevalence, and several other behavioral outcomes (active transport to and from school, sleep, and consumption of takeaway food and sweetened drinks).
The RESPOND trial utilized systems thinking to help communities identify and target local childhood obesity risk factors. The researchers emphasize that understanding these local factors is crucial in assessing the intervention’s overall merit.
The findings suggest that empowering communities to use systems thinking in obesity prevention could have a protective effect on children’s health, even in the face of major challenges like the COVID-19 pandemic.
Given the scarcity of effective interventions to address childhood obesity and non-communicable diseases, building capacity within communities to deliver systems-based interventions seems to be a promising approach.
Further analyses and investments in RESPOND’s findings could lead to broader training of community health workers in systems thinking and enable the creation of a learning system for effective and rapid knowledge acquisition. Further investigation is also needed into the observed gender differences in intervention effects.
Credit: news-medical.net
Can millets raise blood sugar levels too: A new study tells you when
Team Metabolic Health
Smart guide on which variety to look out for and how to have it
Have you been buying packaged millets from shop shelves thinking you are making a healthy choice? Chances are they are polished millets which could be spiking your sugar levels just like any other carbohydrate. While polished millets bring down the cooking time and ease digestion, they also lead to the loss of minerals and phytochemicals that make them healthy. Debranning — or removing the outer layers of the grain — also makes them starchy and high in glycemic index, according to Dr Shobana Shanmugam, head of the department of diabetes food technology at Madras Diabetes Research Foundation.

Millets cooked like rice are preferable to chapatis made of millets as they hold more moisture and are easier to eat. (File)
“Integrating different millets into the diet — instead of wheat and rice — can help in increasing food diversity. This is essential for combating the triple burden of malnutrition in India — undernutrition, overnutrition, and micronutrient deficiency. But debranning reduces food value,” she says. Her team recently published a paper in the journal Springer Nature on the impact of debranning on five Indian millets — foxtail, little, kodo, barnyard, and proso.
What happens when millets are debranned or polished?
Debranning leads to loss of minerals — iron, calcium, zinc, phosphorus, magnesium — in all five millets. “In fact, iron levels went below the level of detection in the grains in our studies,” says Dr Shanmugam. The process also led to the loss of protein content in all but two of the millets — little and barnyard millets. These are likely to contain the protein in the inner layers.
Significantly, the available carbohydrate went up across all five millets when polished by up to 11 gm per 100 gm of the millet. “We looked at the grains with electron microscopy to check which are the layers that have been removed. And, higher the degree of polish, the more starchy the grain becomes,” says Dr Shanmugam.
“While there is awareness that millets are better for your health, people might not know that these grains too can be polished. And, that the process can remove a lot of the nutrients. Yet, many polished millets make health claims that can be misleading,” she warns.
How can one tell whether the millet has been polished?
Dr Shanmugam suggests a few ways one can tell whether a grain has been polished or not:
1) Polished grains look whiter than the unpolished ones, which are dull.
2) Two, the grains should be glassy because of the oil content in the outer layers.
3) The polished grains are likely to be smoother to touch while the unpolished ones are rougher.
How can millets be integrated into our diets?
Millets cooked like rice are preferable to chapatis made of millets as they hold more moisture and are easier to eat. “If you see rice, it expands quite a bit when cooked. Around 70 per cent of the rice we eat is water; chapatis are the opposite and will have about 30 per cent water.”
Bottom of Form
She also warns against diabetics eating porridge made of millets. “When we make millet porridge, it again increases the glycemic index and can raise blood glucose levels.”
Credit: The Indian Express
Weight loss injections and cancer: 6 questions, answered
Team Metabolic Health
Most people know that losing weight has numerous benefits, but making major lifestyle changes can be extremely difficult. For example, obese people are often at risk for injuries when they start a new exercise routine, which can set them back or ultimately cause them to give up on it. As a result, more and more people have been turning to weight loss medications for help.
In the last couple of years, a new class of weight-loss injection drugs called GLP-1 agonists like semaglutide, tirzepatide, liraglutide and dulaglutide has made headlines for their promise to help people lose weight. The drugs go by several different brand names, and more are being approved all the time. But what are they, how do they work and are there things current cancer patients should be aware of if they’re considering these drugs?
For answers to these questions, we talked to endocrine neoplasia and hormonal disorders specialist Sonali Thosani, M.D.
How do these drugs work, and how are they different from previous weight loss drugs?
Previous weight loss drugs worked in a few different ways. Some suppressed appetite and made you feel fuller longer, but these could only be used for a limited time due to the side effects. Others inhibited fat absorption, but were hard to tolerate for many patients because they caused gastrointestinal issues.
This new class of drugs, the GLP-1 agonists, has been used for diabetes treatment since 2005, but they only have gotten approval for obesity treatment in the last decade. They work by slowing down gastric emptying. This makes patients feel fuller longer, helping them eat less. They also help balance blood sugars after eating by stimulating insulin secretion and inhibiting glucagon secretion.
Studies have shown that patients can lose up to 20% of their body weight with GLP-1 agonists. That makes these drugs comparable to surgical options, like gastric sleeve surgeries. However, they also have some side effects, with many patients experiencing nausea, vomiting and diarrhea. There have also been some recent reports that they might be linked to gastroparesis in some patients. This is a paralysis of the stomach that can be debilitating and hard to treat.
What’s also interesting about these drugs is that GLP-1 is a neuropeptide. This means it’s made in the neuronal cells in the brain and released in the hypothalamus, which controls several metabolic and cardiovascular functions. So, it will be interesting to see what we continue to learn about how these drugs work and what the long-term effects might be on other organ systems.
Can weight loss injections decrease your cancer risk?
This is a more complicated question than it seems because obesity is so closely associated with increased cancer risk. There are really two questions here:
Do the drugs themselves decrease cancer risk?
Does their ability to decrease obesity result in a lowered cancer risk?
There is significant evidence that the answer to the second question is yes, with the caveat that patients should know that these drugs aren’t meant to be taken forever. Many people take GLP-1 agonists or other weight loss medication, they lose weight, they go off the drugs and then they gain the weight back. That’s not going to help lower long-term cancer risk.
Where these types of drugs can be helpful is that many obese people have a hard time making healthy lifestyle changes because it’s very difficult for them to exercise. If taking these drugs for a limited amount of time can help some lose weight quickly so they can get on an exercise plan they can stick to, then that’s helping lower cancer risk long-term. But it all comes back to the person making and sticking to those lifestyle changes, even after they stop taking the drugs. If they can do that, then you’re probably seeing a net positive about long-term cancer risk or other long-term health risks.
As for whether the drugs themselves reduce cancer risk, it’s too early to say for sure. But there is some evidence that GLP-1 agonists like semaglutide may decrease cancer risk beyond just their ability to help people lose weight. A study published early this year showed that patients with diabetes who used weight loss injections were less likely to have colorectal cancer compared to patients on other diabetes drugs, regardless of whether the patients were overweight.
Are there concerns that weight loss injections could increase cancer risk?
There was an early study a couple of years ago that indicated a possible link to thyroid cancer, but that study had some limitations, and subsequent studies have shown that there is likely not a link there. The European Medical Agency even announced that they did not find a causal link after a months-long review of the data.
There has also been some concern that some of the side effects could increase the risk of pancreatic cancer, but so far, studies have not shown that to be the case.
If cancer isn’t a major concern, are there other concerns about these drugs?
There’s always a bit of wariness when a new class of drugs comes to market because we’ve seen several times where promising drugs came to market for weight loss and then they’ve had to be pulled back, due to safety concerns. What’s unique about GLP-1 agonists compared to other weight loss drugs is that we already have a lot of experience with them in patients with diabetes. We also know from the published data that these drugs have heart health benefits; this sets them apart from other weight loss drugs currently on the market.
The primary concern is the availability of these drugs for the patients who need them. They’re expensive, and it’s been hard to get insurers to cover them, even when a patient has a clear indication for them. And there are celebrities and influencers using them who don’t have indications for their use, adding to a national shortage and making them even harder to get.
And the gastroparesis issue is not a small thing. Doctors need to be selective when deciding whether a patient meets the criteria for these drugs because gastroparesis can be very difficult to manage. Guidelines from anesthesia and surgical societies recommend holding the weekly formulations of these drugs for at least a week before surgery, so careful planning is required if a patient is using these therapies.
Are there concerns about these drugs for people who have already had cancer?
There are a couple of things to note for cancer patients, which is why it is always very important to discuss these things with your care team.
We generally avoid GLP-1 agonists for pancreatic cancer patients, for example, because these patients are already at high risk for pancreatitis, and these drugs do carry some potential risk for that. We are also cautious about using these drugs if you’re on active cancer therapy and experiencing side effects such as nausea and vomiting; GLP-1 agonist therapy can sometimes worsen those.
These drugs cause dramatic weight loss, some of which is also a significant muscle mass loss. So, we need to carefully monitor their use in patients who are on active chemotherapy, as sarcopenia and weight loss can make it harder for patients to tolerate chemotherapy.
Are there alternatives to weight loss drugs that people should consider?
I think bariatric surgery is underutilized. And, of the 20 million adults in the US who suffer from severe obesity, less than 1% will undergo bariatric surgery annually. There was a study presented at a national meeting looking at the role of bariatric surgery in patients with obesity and the impact on cancer prevention, and it found a marked decrease in cancer diagnoses in patients with obesity who underwent bariatric surgery compared to those who didn’t. This was really the first study to address this question, and I think this exciting new area will have more studies coming out in the next 10 to 15 years.
Credit: mdanderson.org
